## Clinical Presentation Analysis The combination of **granulomatous anterior uveitis** (mutton-fat KPs, granulomatous appearance), **posterior uveitis** (vitritis, yellowish infiltrates), and **systemic findings** (bilateral hilar lymphadenopathy, hypercalcemia) is pathognomonic for **sarcoidosis**. ### Key Diagnostic Features **Key Point:** Sarcoidosis is a multisystem granulomatous disease that commonly presents with ocular involvement (25% of sarcoid patients have uveitis). | Feature | Sarcoidosis | TB Uveitis | Syphilis | Behçet's | |---------|-------------|-----------|----------|----------| | **KP type** | Mutton-fat (granulomatous) | Granulomatous | Non-granulomatous | Non-granulomatous | | **Vitritis** | Snowball opacities, infiltrates | Caseating granulomas | Mild | Severe hemorrhagic | | **Systemic signs** | Hilar LAD, hypercalcemia | Pulmonary TB, constitutional | Rash, serology+ | Oral/genital ulcers | | **Hypercalcemia** | Common (25%) | Rare | No | No | | **Chest X-ray** | Bilateral hilar LAD | Apical infiltrates ± cavitation | Normal | Normal | ### Pathophysiology Sarcoidosis causes **non-caseating granulomatous inflammation** in the uvea. The **hypercalcemia** results from extrarenal 1α-hydroxylase activity in activated macrophages within granulomas, leading to increased calcitriol production. **High-Yield:** The **combination of mutton-fat KPs + bilateral hilar lymphadenopathy + hypercalcemia** is diagnostic for sarcoidosis until proven otherwise. ### Diagnostic Workup 1. **ACE level** (elevated in 60% of sarcoid patients) 2. **Serum calcium & 24-hour urinary calcium** 3. **Chest X-ray** (bilateral hilar lymphadenopathy is hallmark) 4. **Tuberculin skin test** (negative in sarcoidosis; positive in TB) 5. **FTA-ABS / RPR** (to exclude syphilis) 6. **Conjunctival biopsy** (non-caseating granulomas confirm diagnosis) **Clinical Pearl:** Sarcoidosis-associated uveitis is typically **chronic and bilateral** (though may present unilaterally initially), whereas TB uveitis is often **unilateral and acute**. ### Management - **Topical corticosteroids** (prednisolone acetate 1% QID) for anterior inflammation - **Systemic corticosteroids** (prednisolone 1 mg/kg/day) for posterior involvement and hypercalcemia - **Immunosuppressants** (methotrexate, azathioprine) for steroid-dependent cases - Monitor serum calcium and renal function during treatment 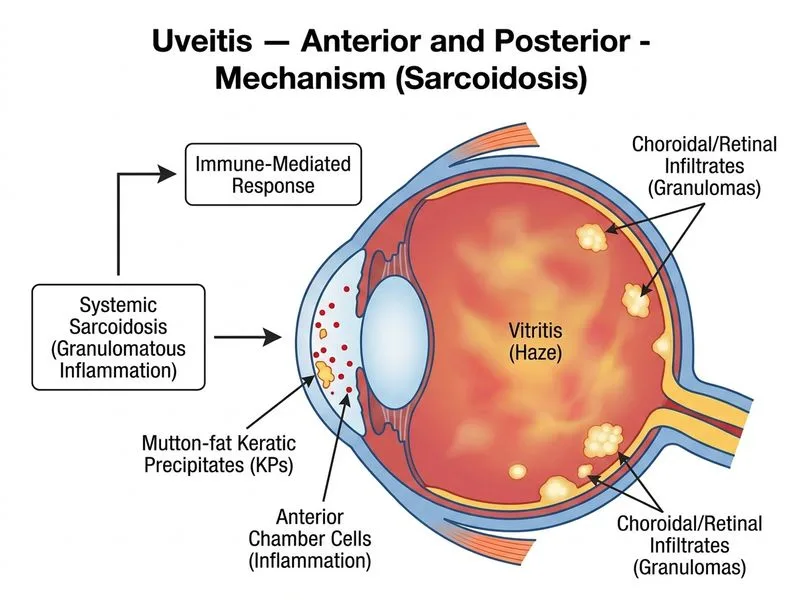
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.