## Clinical Scenario Analysis This patient presents with **isolated posterior uveitis** (vitritis with minimal anterior chamber involvement, normal fundus on initial examination). The key clinical features are: - Sudden onset with floaters and photopsia - Vitritis (2+ cells) without anterior reaction - Normal fundus examination - No retinal detachment on B-scan - No systemic symptoms at presentation ## Diagnostic Approach to Posterior Uveitis **Key Point:** Posterior uveitis has a broad differential diagnosis spanning infectious, granulomatous, and idiopathic causes. Systemic workup is mandatory before initiating immunosuppressive therapy. ### Differential Diagnosis Requiring Investigation | Diagnosis | Key Investigation | Clinical Clue | |-----------|-------------------|---------------| | Sarcoidosis | Chest X-ray, ACE level, serum calcium | Granulomatous uveitis, systemic involvement | | Tuberculosis | Tuberculin skin test, IGRA, chest imaging | Granulomatous pattern, risk factors | | Toxoplasmosis | Serology, fundoscopy (focal retinochoroiditis) | Geographic distribution, immunostatus | | CMV retinitis | Serology, CD4 count (if immunocompromised) | Hemorrhagic border, immunosuppression | | Idiopathic | Exclusion diagnosis | After infectious/granulomatous ruled out | ## Why Systemic Workup is the Next Step **High-Yield:** In a patient with isolated posterior uveitis and no anterior chamber reaction, the first priority is to exclude **sarcoidosis** and **tuberculosis**—the two most common granulomatous causes in India. These require different management and have systemic implications. 1. **Chest X-ray** — screens for pulmonary sarcoidosis or TB 2. **ACE level and serum calcium** — markers of sarcoidosis activity 3. **Tuberculin skin test (or IGRA)** — TB exposure/infection status **Clinical Pearl:** Starting corticosteroids without ruling out TB can lead to disseminated tuberculosis. Similarly, missing sarcoidosis delays systemic evaluation and risk stratification. ## Why Not the Other Options? **Immediate vitrectomy** is premature. Diagnostic vitrectomy is reserved for: - Diagnostic uncertainty after initial workup - Severe vitritis obscuring fundus view (this patient has normal fundus) - Suspected CMV or other infections requiring culture/PCR **High-dose corticosteroids without workup** risks: - Unmasking or worsening occult TB - Missing sarcoidosis diagnosis - Inappropriate immunosuppression if infectious cause present **Observation alone** delays diagnosis and risks disease progression (e.g., macular edema, epiretinal membrane formation). ## Management Algorithm ```mermaid flowchart TD A[Posterior Uveitis Presentation]:::outcome --> B{Anterior Chamber<br/>Involvement?}:::decision B -->|Minimal/None| C[Systemic Workup:<br/>CXR, ACE, TST, IGRA]:::action B -->|Significant| D[Anterior Uveitis Protocol]:::action C --> E{Granulomatous<br/>or Infectious?}:::decision E -->|TB Suspected| F[Anti-TB Therapy]:::action E -->|Sarcoidosis| G[Systemic Corticosteroids]:::action E -->|Idiopathic| H[Topical + Systemic Steroids]:::action E -->|CMV/Other Infection| I[Specific Antimicrobial]:::action ``` 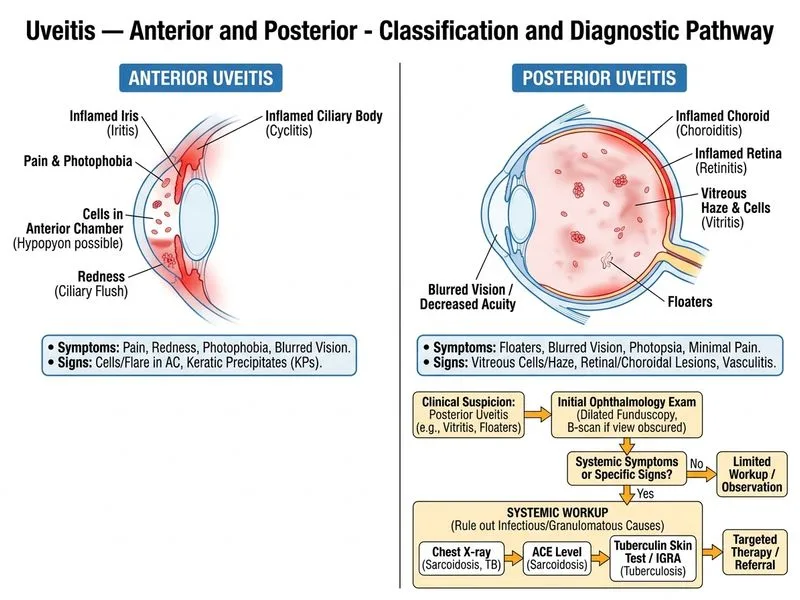
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.