## Clinical Scenario Analysis This is a case of **acute anterior uveitis (AAU)** with: - Severe anterior chamber inflammation (3+ cells, fibrin, hypopyon) - Posterior synechiae (indicating previous episodes or severe current inflammation) - HLA-B27 positive ankylosing spondylitis (associated with recurrent AAU) - Reduced vision (6/24) - First presentation or acute exacerbation ## Management Hierarchy for Acute Anterior Uveitis **Key Point:** The primary goal in acute AAU is rapid suppression of inflammation to prevent complications (posterior synechiae, cataract, secondary glaucoma, vision loss). Topical corticosteroids and cycloplegics are first-line; systemic therapy is reserved for severe, refractory, or bilateral cases. ### Treatment Pyramid ```mermaid flowchart TD A[Acute Anterior Uveitis]:::outcome --> B{Severity Assessment}:::decision B -->|Mild-Moderate<br/>Unilateral| C[Topical Steroids + Cycloplegic]:::action B -->|Severe<br/>Hypopyon/Fibrin| D{Bilateral or<br/>Recurrent?}:::decision D -->|No| E[Intensive Topical Therapy]:::action D -->|Yes| F[Add Systemic Steroids]:::action E --> G[Review 24-48 hrs]:::action F --> H[Review 24-48 hrs]:::action C --> I{Response to<br/>Topical?}:::decision I -->|Good| J[Taper Topical Steroids]:::action I -->|Poor/Recurrent| K[Consider Systemic Therapy]:::action ``` ## Why Topical Therapy is the Correct First Step **High-Yield:** Even in severe unilateral AAU, topical corticosteroids achieve excellent intraocular concentrations and are the standard of care. Systemic steroids are added only if: 1. Bilateral involvement 2. Recurrent episodes (>2 per year) 3. Failure to respond to topical therapy in 48–72 hours 4. Posterior segment involvement ### Topical Regimen for Severe AAU | Component | Dose | Rationale | |-----------|------|----------| | Prednisolone acetate 1% | Hourly (or 2-hourly) initially | Rapid anti-inflammatory effect; achieves high aqueous concentration | | Cyclopentolate 1% | 3–4 times daily | Relieves ciliary spasm, prevents posterior synechiae, reduces pain | | NSAIDs (topical) | 4–6 times daily | Adjunctive anti-inflammatory; reduces prostaglandin-mediated inflammation | **Clinical Pearl:** Posterior synechiae in this patient suggest previous inflammation or severe current inflammation. Aggressive cycloplegia is essential to prevent further adhesions. ## Why Not the Other Options? ### Option 1: Oral Prednisolone as First-Line (Option B) **Incorrect timing.** Systemic corticosteroids are not indicated for unilateral acute AAU in the absence of: - Bilateral involvement - Recurrent episodes - Posterior segment disease - Failure of topical therapy Starting oral steroids prematurely increases systemic side effects without additional benefit in unilateral cases. ### Option 2: Anterior Chamber Paracentesis (Option C) **Inappropriate procedure.** Paracentesis is not a primary management step for AAU. It may be considered in: - Acute angle-closure glaucoma (not the case here) - Diagnostic purposes (aqueous tap for culture/PCR in suspected infectious uveitis) - Severe elevated IOP unresponsive to medical therapy This patient's vision loss is from inflammation and corneal edema, not acute glaucoma. ### Option 3: Systemic Immunosuppression (Option D) **Premature escalation.** Methotrexate or azathioprine are reserved for: - Chronic or recurrent uveitis (>2 episodes/year) - Bilateral involvement - Failure of topical and systemic corticosteroids - Steroid-dependent cases First-line therapy must be exhausted before immunosuppression. ## Monitoring and Follow-Up **Tip:** Review the patient at 24 hours to assess response: - If improving: begin tapering topical steroids over 4–6 weeks - If static or worsening: add oral prednisolone 0.5–1 mg/kg/day - If recurrent episodes develop: consider systemic immunosuppression **Warning:** Do not taper topical steroids too rapidly; this risks rebound inflammation and posterior synechiae formation. 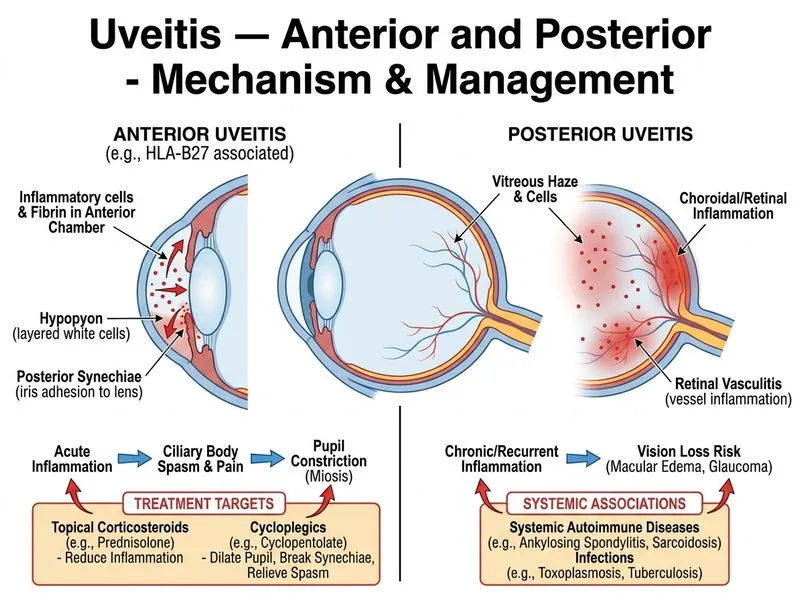
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.