## Epidemiology of Anterior Uveitis **Key Point:** In immunocompetent individuals, approximately 50% of anterior uveitis cases are idiopathic, with no identifiable systemic or ocular cause. ### Causes of Anterior Uveitis — Frequency Distribution | Cause | Frequency (%) | Notes | |-------|---------------|-------| | Idiopathic | 40–50 | Most common; HLA-B27 association in subset | | HLA-B27–associated (AS, ReA, IBD) | 15–25 | Acute, recurrent, unilateral | | Herpes simplex/zoster | 5–10 | Keratic precipitates, iris atrophy | | Tuberculosis | 5–10 | More common in endemic regions (India) | | Syphilis | 2–5 | Secondary/tertiary; rare in modern era | | Trauma/surgery | 5–10 | Post-operative inflammation | | Sarcoidosis | 3–5 | Granulomatous; systemic features | **High-Yield:** Even in endemic TB regions like India, idiopathic anterior uveitis remains the single most common diagnosis overall. TB uveitis is more common in posterior uveitis or panuveitis presentations. **Clinical Pearl:** When anterior uveitis is acute, unilateral, and recurrent, think HLA-B27–associated disease (ankylosing spondylitis, reactive arthritis, IBD); when chronic and granulomatous, consider sarcoidosis or TB. ## Why Idiopathic? Many cases of anterior uveitis have no demonstrable systemic association despite thorough investigation. This is a diagnosis of exclusion, not a diagnosis of ignorance — it reflects the limits of current diagnostic modalities. 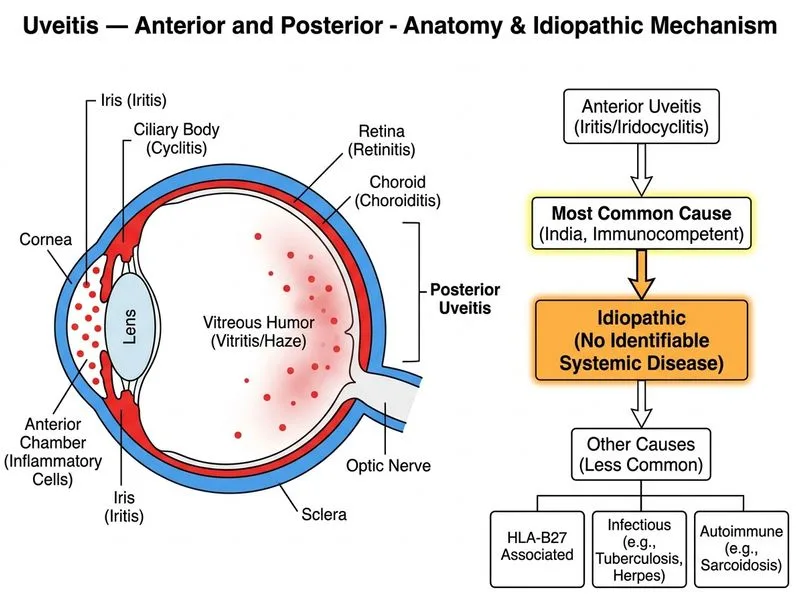
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.