## Clinical Presentation Analysis This patient presents with features highly suggestive of **tuberculous posterior uveitis**: - History of TB (treated 6 months ago) - Floaters, photopsia, and blurred vision (posterior uveitis symptoms) - Quiet anterior chamber (typical of posterior uveitis) - Multiple yellow-white granulomatous lesions in posterior pole - Mild vitritis - Early hyperfluorescence on FA (granulomatous lesions) ## Diagnosis: Presumed Tuberculous Uveitis **Key Point:** In a patient with a history of TB presenting with granulomatous posterior uveitis and characteristic fundal lesions, the diagnosis is presumed tuberculous uveitis until proven otherwise. Treatment should not be delayed pending culture confirmation (which takes 2–8 weeks). ## Management Strategy ### Step 1: Confirm TB Etiology (Clinical + Radiological) Before starting antituberculous therapy (ATT), confirm: 1. **Chest X-ray** — look for active or healed TB lesions 2. **TB serology** — QuantiFERON-Gold, IGRA, or Mantoux test (though history of TB makes this less specific) 3. **Clinical pattern** — granulomatous lesions, vitritis, characteristic FA findings **High-Yield:** In endemic regions (India), a treated TB patient with granulomatous posterior uveitis and compatible fundal findings has a very high pre-test probability of TB uveitis. Waiting for culture results (2–8 weeks) delays treatment and risks vision loss. ### Step 2: Initiate Antituberculous Therapy + Systemic Corticosteroids Once TB etiology is confirmed (or highly presumed): | Component | Regimen | Duration | Rationale | |-----------|---------|----------|----------| | **ATT** | RIPE (Rifampicin, Isoniazid, Pyrazinamide, Ethambutol) | 2 months intensive + 4 months continuation | Standard TB treatment; rifampicin penetrates ocular tissues | | **Systemic corticosteroids** | Prednisolone 0.5–1 mg/kg/day, taper over 8–12 weeks | Concurrent with ATT | Controls inflammation, prevents immune recovery uveitis (IRU) | | **Topical corticosteroids** | Prednisolone acetate 1% 4–6× daily | As needed for anterior chamber involvement | Adjunctive anti-inflammatory | **Clinical Pearl:** Systemic corticosteroids are ESSENTIAL in tuberculous uveitis to prevent immune recovery uveitis (IRU), a severe inflammatory rebound that can occur as ATT takes effect. They also improve visual outcomes by controlling granulomatous inflammation. ### Timing of Treatment Initiation ```mermaid flowchart TD A[Granulomatous Posterior Uveitis + TB History]:::outcome --> B{Presumed TB Uveitis?}:::decision B -->|Yes: compatible fundal lesions + CXR findings| C[Confirm TB etiology: CXR, TB serology]:::action B -->|No: atypical features| D[Investigate other etiologies]:::action C --> E[Start ATT RIPE regimen]:::action E --> F[Concurrent systemic corticosteroids]:::action F --> G[Topical corticosteroids as adjunct]:::action G --> H[Monitor for immune recovery uveitis]:::action H --> I[Taper corticosteroids over 8-12 weeks]:::action ``` **Key Point:** Do NOT delay ATT initiation waiting for culture results. Culture confirmation is a "nice-to-have" but not a prerequisite for starting treatment in presumed TB uveitis. ## Why Each Step Matters 1. **Confirm TB etiology first** — ATT has significant side effects (hepatotoxicity, peripheral neuropathy); confirmation reduces risk of unnecessary treatment in non-TB cases. 2. **Systemic corticosteroids are mandatory** — They prevent IRU and improve visual prognosis. 3. **Topical therapy is adjunctive** — Insufficient alone for posterior uveitis; systemic therapy is required. --- ## Vitreous Biopsy: When Is It Indicated? **Tip:** Vitreous biopsy is reserved for: - Atypical presentations (no TB history, unusual lesion pattern) - Diagnostic uncertainty after initial workup - Suspected infectious uveitis (fungal, viral) with negative serology - Lymphoma or malignancy suspected In this case, with a clear TB history and classic granulomatous lesions, biopsy is NOT the next step. 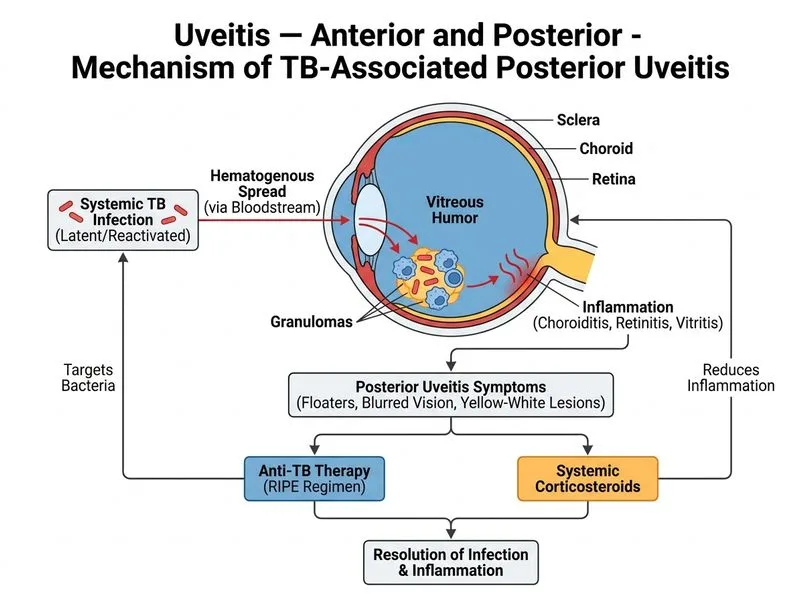
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.