## Acute Complication: Right Ventricular Failure Secondary to Pulmonary Hypertension ### Pathophysiology of RV Failure in Mitral Stenosis **Key Point:** Chronic mitral stenosis leads to progressive pulmonary hypertension, which ultimately causes right ventricular failure. This is a natural evolution of untreated MS and represents a critical hemodynamic decompensation. ### Mechanism of Pulmonary Hypertension in MS 1. **Passive pulmonary hypertension (early):** Elevated left atrial pressure is transmitted retrograde to the pulmonary circulation, increasing pulmonary venous and capillary pressures. 2. **Reactive pulmonary hypertension (progressive):** Chronic pulmonary venous hypertension triggers pulmonary arteriolar vasoconstriction and medial hypertrophy of pulmonary arteries (muscularization). 3. **Fixed pulmonary hypertension (late):** Structural remodeling of pulmonary vessels becomes irreversible; pulmonary vascular resistance remains elevated even after mitral valve surgery. 4. **RV pressure overload:** The right ventricle must generate increasingly higher pressures to eject blood against the elevated pulmonary vascular resistance. 5. **RV dilatation and failure:** Chronic RV pressure overload leads to RV hypertrophy, then dilatation, and eventually systolic dysfunction. ### Clinical Features of Acute RV Failure in This Case | Finding | Mechanism | |---------|----------| | **Acute dyspnea & hemoptysis** | Pulmonary edema from elevated LA pressure; hemoptysis from rupture of dilated bronchial veins or pulmonary infarction | | **Syncope on exertion** | Inability of RV to increase cardiac output; fixed or falling systemic BP during increased demand | | **Hypotension (95/60)** | RV failure → reduced LV preload → decreased cardiac output and systemic hypotension | | **Cyanosis** | Right-to-left shunting through patent foramen ovale (PFO) or decreased cardiac output with increased peripheral oxygen extraction | | **Loud S2** | Increased pulmonary artery pressure raises the intensity of the pulmonary component of S2 | | **RV heave** | RV hypertrophy and dilatation; palpable at left lower sternal border | | **Pulsatile hepatomegaly** | RV failure → elevated right atrial pressure → hepatic venous congestion | | **Acute pulmonary edema on CXR** | Acute decompensation with Kerley B lines (interlobular septal edema) and prominent pulmonary artery | | **Right axis deviation & RV strain on ECG** | RV hypertrophy and acute RV pressure overload | ### Natural History of Untreated Mitral Stenosis **High-Yield:** The progression from MS → pulmonary hypertension → RV failure is a classic hemodynamic cascade. Exertion (which increases cardiac output and LA pressure) can precipitate acute decompensation. ```mermaid flowchart TD A[Mitral Stenosis]:::outcome --> B[Elevated LA Pressure]:::outcome B --> C[Passive Pulmonary Hypertension]:::outcome C --> D[Chronic Pulmonary Venous Congestion]:::outcome D --> E[Pulmonary Arteriolar Vasoconstriction & Medial Hypertrophy]:::outcome E --> F[Reactive Pulmonary Hypertension]:::outcome F --> G[RV Pressure Overload]:::outcome G --> H[RV Hypertrophy]:::outcome H --> I[RV Dilatation]:::outcome I --> J[RV Systolic Dysfunction]:::outcome J --> K[Acute RV Failure]:::urgent K --> L[Hypotension, Syncope, Shock]:::urgent A --> M[Exertion Increases Cardiac Output]:::decision M --> N[Further Elevation of LA Pressure]:::outcome N --> K ``` ### Why Syncope Occurs **Clinical Pearl:** Syncope in MS with pulmonary hypertension indicates severe RV dysfunction. The RV cannot increase cardiac output during exertion, leading to a paradoxical fall in systemic blood pressure and cerebral hypoperfusion. This is a sign of advanced disease and carries a poor prognosis without urgent intervention. ### Diagnostic Confirmation - **Echocardiography:** Reduced mitral valve area (<1 cm²), severely elevated LA pressure, RV dilatation, reduced RV systolic function, elevated tricuspid regurgitation velocity (indicating pulmonary hypertension). - **Right heart catheterization:** Elevated pulmonary artery pressure (>60 mmHg systolic), elevated pulmonary capillary wedge pressure (PCWP), elevated right atrial pressure, reduced cardiac output. - **Chest X-ray:** Prominent pulmonary artery ("pulmonary artery knob"), Kerley B lines, acute pulmonary edema. ### Management 1. **Immediate:** Oxygen, diuretics, vasodilators (nitrates, hydralazine) to reduce LA pressure. 2. **Pulmonary vasodilators:** Inhaled nitric oxide or sildenafil may provide temporary relief but do not reverse fixed pulmonary hypertension. 3. **Definitive:** Urgent mitral valve replacement (PMBC is contraindicated in severe pulmonary hypertension with RV failure due to risk of acute decompensation). **Mnemonic: ARDS vs. Pulmonary Edema in MS** — Acute Respiratory Distress Syndrome (ARDS) requires bilateral infiltrates and PEEP; pulmonary edema in MS shows Kerley B lines, cardiomegaly, and responds to diuretics. 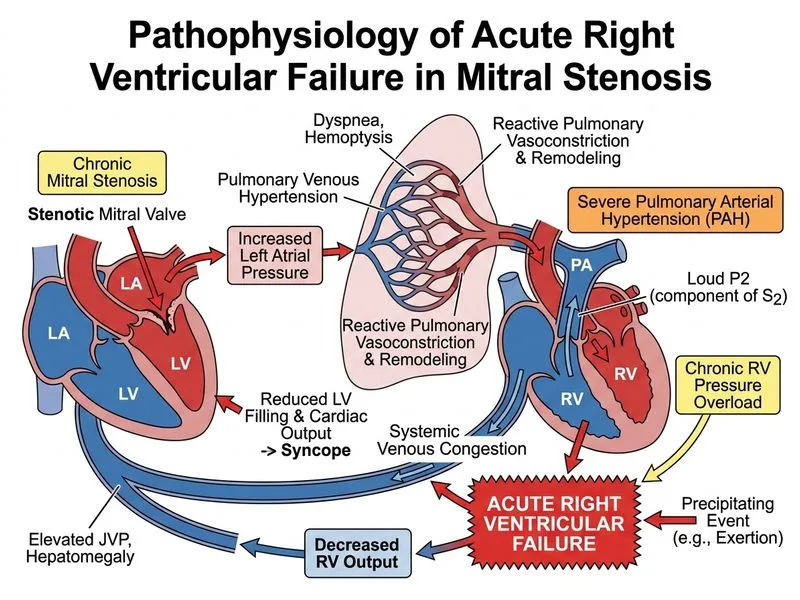
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.