## Distinguishing Acute from Chronic Mitral Regurgitation ### Key Pathophysiologic Difference **Key Point:** In acute mitral regurgitation, the left atrium has not had time to dilate and remodel; therefore, regurgitant flow causes a sudden rise in left atrial pressure, leading to acute pulmonary edema despite a normal-sized left ventricle. In chronic mitral regurgitation, the left atrium and left ventricle gradually dilate over years, accommodating the regurgitant volume with less acute hemodynamic decompensation. ### Comparison Table | Feature | Acute MR | Chronic MR | | --- | --- | --- | | **LV size** | Normal or mildly enlarged | Markedly dilated | | **LA size** | Normal or mildly enlarged | Markedly dilated | | **Pulmonary edema** | Acute, severe (early) | Develops late, if at all | | **Atrial fibrillation** | Uncommon (early) | Common (late) | | **Murmur character** | Often soft, brief | Holosystolic, loud | | **CXR findings** | Pulmonary edema + normal heart size | Cardiomegaly ± pulmonary edema | ### Clinical Pearl **Clinical Pearl:** The **normal LV size with acute pulmonary edema** is the hallmark discriminator. The unprepared left atrium cannot accommodate sudden regurgitant volume, so pressure backs up acutely into the pulmonary circulation. This is why acute severe MR (e.g., from papillary muscle rupture post-MI or endocarditis) presents as fulminant pulmonary edema despite preserved LV systolic function. ### High-Yield Mechanism **High-Yield:** Acute MR → ↑ LA pressure acutely → pulmonary edema; Chronic MR → LA/LV remodeling → accommodation of regurgitant volume → AF, cardiomegaly, late decompensation. [cite:Robbins 10e Ch 12] 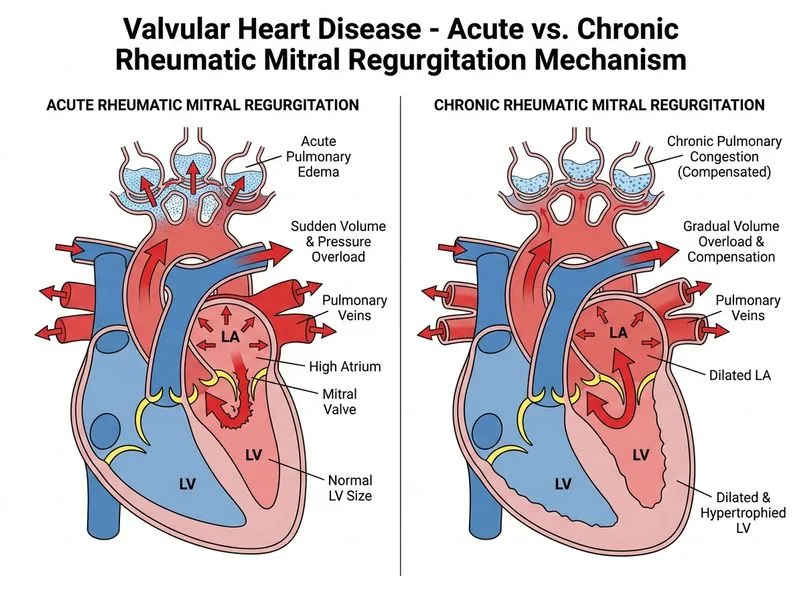
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.