## Endovenous Laser Ablation (EVLA) — Mechanism, Technique, and Outcomes ### Understanding EVLA Mechanism **Key Point:** EVLA works through direct thermal injury to the venous endothelium, causing intimal damage, collagen denaturation, and subsequent fibrosis. This leads to permanent vein occlusion and sealing of the incompetent segment. The mechanism involves: 1. Laser energy absorption by intravascular blood (hemoglobin and water) 2. Rapid heating of blood and venous wall 3. Endothelial denudation and thermal necrosis 4. Inflammatory response and fibrosis 5. Permanent vein closure ### Wavelength Selection in EVLA **High-Yield:** The 1470 nm wavelength is the most commonly used in modern EVLA because: - It is preferentially absorbed by water (H₂O) in venous blood - Water absorption coefficient is high at this wavelength - Provides efficient energy transfer with minimal scattering - Results in better endothelial damage with lower power requirements - Reduces perivenous thermal injury compared to older 980 nm systems Alternative wavelengths (1320 nm, 1550 nm) are less commonly used in clinical practice. ### Tumescent Anesthesia — Critical Component **Key Point:** Tumescent anesthesia is **mandatory** in EVLA and serves multiple essential functions: - Provides perivenous padding/thermal buffer around the vein - Protects surrounding tissues (skin, nerves) from thermal injury - Reduces skin burns and nerve damage (especially saphenous nerve) - Compresses the vein, bringing walls into contact with the fiber - Provides local anesthesia, reducing procedural pain - Improves treatment efficacy by optimizing vein-fiber contact Without tumescent anesthesia, the risk of thermal injury to surrounding structures increases significantly. ### EVLA vs. Conventional Ligation — Recurrence Rates **Clinical Pearl:** This is the key discriminator. EVLA has **LOWER** recurrence rates compared to conventional saphenofemoral ligation (SFL), NOT higher. | Parameter | EVLA | Conventional SFL | |-----------|------|------------------| | 5-year recurrence rate | 5–15% | 15–30% | | Mechanism of recurrence | Recanalization, incomplete ablation | Neovascularization at SFJ | | Technical failure | Rare with modern systems | Occurs with inadequate ligation | | Cosmetic outcome | Superior (minimally invasive) | Good (but larger scar) | **High-Yield:** The statement that "EVLA has higher recurrence than ligation" is **INCORRECT**. EVLA actually has superior long-term outcomes with lower recurrence because: - Complete thermal ablation of the entire incompetent segment - No neovascularization at the ablation site (unlike SFJ ligation) - Endothelial damage is more extensive and uniform - Recanalization is rare (occurs in <10% at 5 years) Neovascularization is a problem with **ligation alone**, where small vessels around the ligated SFJ can recanalize and reconnect to distal saphenous branches, leading to recurrent varicosities. ### Summary of Correct vs. Incorrect Statements | Statement | Correct? | Reason | |-----------|----------|--------| | EVLA causes endothelial damage and fibrosis | ✓ Yes | This is the fundamental mechanism | | 1470 nm wavelength absorbed by water | ✓ Yes | Preferred wavelength in modern practice | | Tumescent anesthesia is mandatory | ✓ Yes | Essential for safety and efficacy | | EVLA has higher recurrence than ligation | ✗ **NO** | EVLA has LOWER recurrence rates | **Warning:** A common misconception is that minimally invasive techniques have higher recurrence. In reality, EVLA's complete ablation of the incompetent vein results in superior outcomes compared to ligation, which leaves the proximal stump and risks neovascularization. 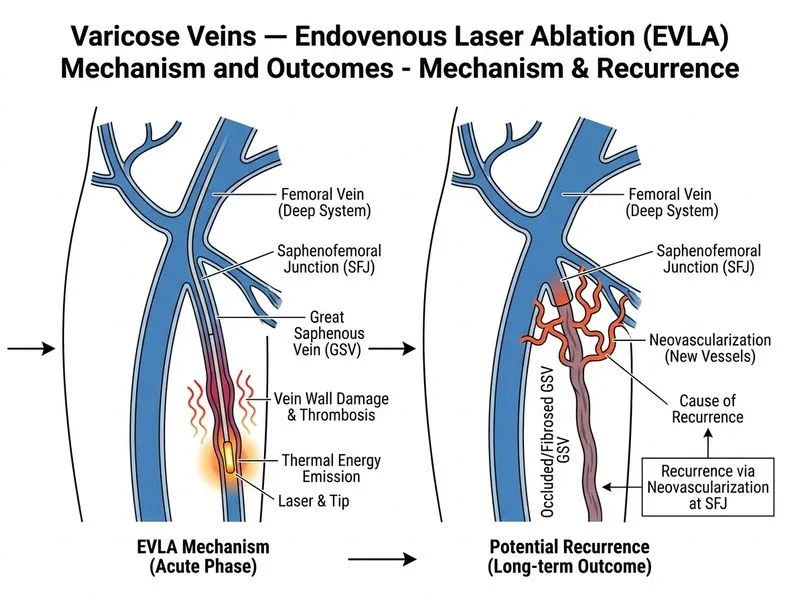
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.