## Clinical Context & Pathophysiology This patient presents with **recurrent superficial thrombophlebitis (ST)** complicating primary varicose veins — a key clinical escalation point that changes management strategy from conservative to interventional. ### Why Recurrent ST Mandates Intervention **Key Point:** Recurrent superficial thrombophlebitis in the presence of GSV incompetence is an **absolute indication for definitive venous intervention** (not merely compression or anticoagulation alone). Each episode carries a small but real risk of thrombus propagation into the deep venous system or PE, particularly if the thrombus extends near the SFJ. **High-Yield:** The presence of: - SFJ diameter >6 mm (this patient: 8 mm) — indicates significant haemodynamic dysfunction - Reflux time >0.5 seconds (this patient: 1.2 seconds) — confirms pathological reflux - Recurrent ST — clinical evidence of repeated thrombotic events These three features together form the **triad mandating intervention** [cite:Rutherford's Vascular Surgery 8e Ch 32]. ### Why EVLA Is Optimal Here **Clinical Pearl:** Endovenous laser ablation (EVLA) is now the **gold-standard first-line intervention** for symptomatic GSV incompetence with complications (including recurrent ST), replacing open saphenofemoral ligation and stripping as the preferred approach in modern practice [cite:NICE CG168, ESVS Guidelines 2015]. **Advantages of EVLA over open surgery:** 1. **Minimally invasive** — local anaesthesia, day-case procedure 2. **Lower morbidity** — avoids groin dissection, saphenous nerve injury (1–3% with EVLA vs. 10–15% with open ligation) 3. **Superior efficacy** — 90–95% technical success; lower recurrence than ligation alone 4. **Faster recovery** — return to normal activity within 1–2 weeks vs. 4–6 weeks post-open surgery 5. **Compression therapy post-EVLA** — 2 weeks of Class II compression is standard and sufficient **Mnemonic: EVLA Superiority — SAFE** - **S**uperiority in outcomes (90–95% success) - **A**void saphenous nerve injury - **F**aster recovery (days vs. weeks) - **E**ndovenous (minimally invasive) ### Why Other Options Are Suboptimal **Option 0 (Compression alone):** Compression therapy is appropriate for **asymptomatic or mildly symptomatic varicose veins without complications**. However, recurrent ST is a **complication** that demands intervention — compression will not prevent further thrombotic episodes and leaves the underlying incompetence untreated. This is passive management of an active problem. **Option 1 (Open ligation + stripping + anticoagulation):** While open saphenofemoral ligation combined with stripping was the historical gold standard (Trendelenburg procedure), it is now considered **second-line** due to: - Higher morbidity (saphenous nerve injury, groin complications, bleeding) - Longer recovery period - No superior efficacy vs. EVLA - Perioperative anticoagulation in this patient (no DVT/PE history) is **not indicated** and adds unnecessary thrombotic risk; anticoagulation is reserved for patients with concurrent DVT or high thrombotic risk. **Option 3 (Warfarin anticoagulation):** Anticoagulation is **not indicated** for superficial thrombophlebitis in the absence of DVT or PE. Warfarin does not address the underlying venous incompetence and will not prevent recurrent ST. This represents a fundamental misunderstanding of ST management — the goal is to eliminate the source of thrombosis (the incompetent vein), not to anticoagulate indefinitely. Anticoagulation is considered only if there is concurrent DVT or if thrombus extends to within 3 cm of the SFJ (risk of propagation). ## Summary: Decision Algorithm ```mermaid flowchart TD A[Varicose veins with GSV incompetence]:::outcome --> B{Symptomatic or complicated?}:::decision B -->|Asymptomatic or mild symptoms| C[Compression therapy + observation]:::action B -->|Symptomatic without complications| D[EVLA or open surgery]:::action B -->|Recurrent superficial thrombophlebitis| E[EVLA first-line]:::action B -->|Concurrent DVT or SFJ thrombus| F[EVLA + anticoagulation]:::action E --> G[Local anaesthesia, day-case]:::action G --> H[2 weeks compression post-EVLA]:::action H --> I[Follow-up ultrasound at 1 month]:::outcome ``` **High-Yield:** The shift from open surgery to EVLA as first-line is a **major paradigm change** in modern vascular surgery (post-2010) and is heavily tested in NEET PG. Know the **indications, advantages, and success rates** of EVLA. 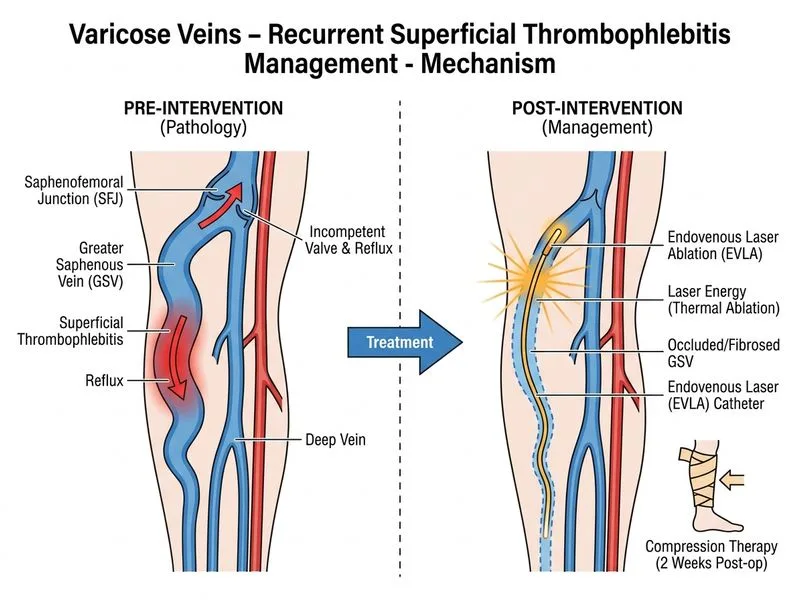
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.