## Clinical Scenario Analysis This patient presents with two concurrent vascular pathologies: 1. **Infrarenal AAA (4.5 cm)** — below the 5.5 cm threshold for elective repair; no rupture, no dissection, asymptomatic from the AAA itself 2. **Critical limb ischemia (CLI)** — ABI 0.4 with rest pain; this is a **limb-threatening emergency** requiring urgent intervention ## Management Rationale ### Why Option A (Defer AAA Repair, Proceed with Limb Revascularization) is Correct **Key Point:** A 4.5 cm infrarenal AAA is **below the threshold for elective repair** (5.5 cm per ACC/AHA and SVS guidelines). The rest pain described is attributable to critical limb ischemia from peripheral arterial disease, **not** from the AAA itself (no dissection, no rupture, infrarenal location). Standard vascular surgery principles (Rutherford's Vascular Surgery; Cronenwett & Johnston): - **AAA repair threshold:** Elective repair is indicated at ≥5.5 cm in men (or rapid expansion >0.5 cm/6 months, or symptomatic AAA). A 4.5 cm AAA does not meet criteria for repair. - **CLI is the immediate priority:** Rest pain (Rutherford category 4) indicates critical ischemia with imminent risk of tissue loss, gangrene, and major amputation within weeks if untreated. - **Correct sequence:** Address the limb-threatening emergency first (femoropopliteal bypass or endovascular revascularization), and continue surveillance of the AAA with imaging every 6–12 months. **Clinical Pearl:** The presence of a sub-threshold AAA does not change the urgency of CLI management. Performing unnecessary AAA repair (open or EVAR) in a patient with CKD (eGFR 35) and a 4.5 cm AAA would expose the patient to unjustified procedural risk. ### Why Each Distractor is Wrong #### Option B: EVAR + Revascularization **Reason:** EVAR is not indicated for a 4.5 cm AAA that does not meet size or symptomatic criteria for repair. Performing EVAR unnecessarily in a CKD patient adds contrast nephropathy risk and procedural morbidity without benefit. The AAA is not the cause of the CLI. #### Option C: Conservative Management Only **Reason:** Conservative management is contraindicated for CLI with rest pain. Without revascularization, the patient will progress to tissue loss and amputation within weeks. Antiplatelet therapy alone cannot restore perfusion to a critically ischemic limb. *(Harrison's Principles of Internal Medicine, 21st ed.)* #### Option D: Immediate Open Repair of AAA + Revascularization **Reason:** Open AAA repair is not indicated for a 4.5 cm aneurysm. Additionally, open repair in a 72-year-old with CKD (eGFR 35) carries high perioperative risk of acute kidney injury, prolonged recovery, and mortality. This option is doubly inappropriate — wrong indication and wrong technique for this patient's risk profile. ## Summary Algorithm | AAA Size | CLI Present | Action | |---|---|---| | < 5.5 cm, asymptomatic AAA | Yes | Treat CLI first; surveil AAA | | ≥ 5.5 cm or symptomatic AAA | Yes | Staged: AAA repair → then CLI | | Ruptured AAA | Any | Emergency AAA repair | ## Key Takeaway **High-Yield:** A 4.5 cm infrarenal AAA does NOT meet criteria for repair. When CLI coexists with a sub-threshold AAA, the limb-threatening emergency (CLI with rest pain) takes priority. Defer AAA repair and proceed with revascularization of the ischemic limb. Surveillance imaging of the AAA every 6–12 months is appropriate. *(Reference: Rutherford's Vascular Surgery and Endovascular Therapy, 9th ed.; SVS Practice Guidelines for AAA Management)* 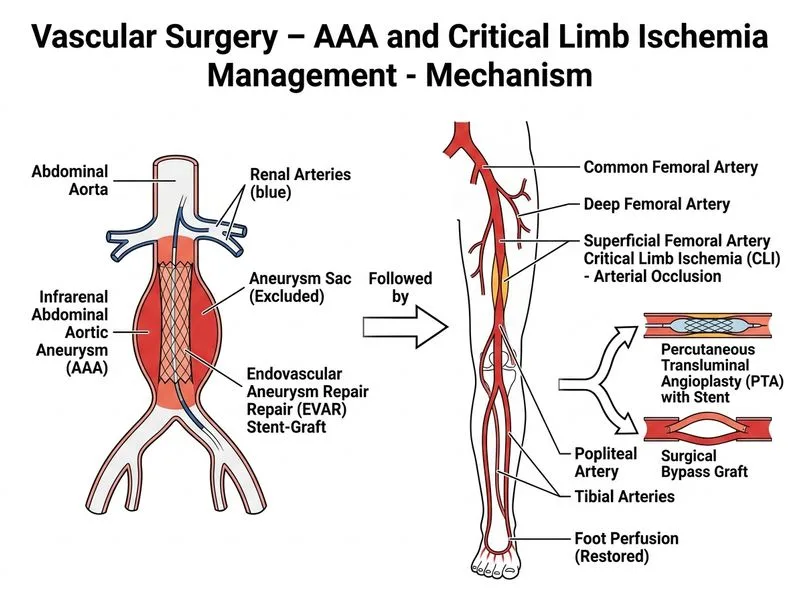
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.