## Clinical Scenario Analysis This patient presents with a classic triad of **infective endocarditis (IE)**: fever, new cardiac murmur, and vascular phenomena (splinter hemorrhages). The presence of vegetations on echocardiography and hematuria with RBC casts (suggesting immune complex glomerulonephritis) further support the diagnosis. ## Pathophysiology of IE-Related Vasculitis **Key Point:** Infective endocarditis causes secondary vasculitis through: 1. Septic emboli from vegetations → microinfarcts 2. Immune complex deposition → glomerulonephritis and vasculitis 3. Direct bacterial invasion of vessel walls The renal involvement (elevated creatinine, hematuria with casts) reflects immune complex-mediated glomerulonephritis, not primary vasculitis requiring immunosuppression. ## Management Algorithm ```mermaid flowchart TD A[Suspected Infective Endocarditis]:::outcome --> B{Blood cultures obtained?}:::decision B -->|No| C[Obtain 3 sets of blood cultures immediately]:::action B -->|Yes| D[Start empirical antibiotics without delay]:::action C --> D D --> E[Broad-spectrum coverage: Vancomycin + Ceftriaxone + Gentamicin]:::action E --> F[Echocardiography confirmation]:::action F --> G[De-escalate based on culture results]:::action ``` ## High-Yield Management Principles **High-Yield:** Empirical antibiotic therapy must **NOT be delayed** while awaiting culture results. IE has high mortality (15–20% even with treatment), and each hour of delay increases morbidity. **Clinical Pearl:** The modified Duke criteria require: - Major: Echocardiographic findings (vegetation, abscess) ✓ - Major: Blood culture positive for typical organism (pending) - Minor: Fever, vascular phenomena (splinter hemorrhages) ✓ - Minor: Immunological phenomena (hematuria) ✓ This patient meets ≥3 criteria and requires immediate antibiotic initiation. **Key Point:** Blood cultures should be obtained **before** antibiotics, but antibiotic administration must not be delayed waiting for results. Obtain cultures, then start therapy immediately. ## Why NOT the Other Options | Option | Why Incorrect | |--------|---------------| | Renal biopsy | Unnecessary and delays treatment; hematuria + casts in IE context is diagnostic of immune complex GN, not primary vasculitis | | Immunosuppression | IE is an **infectious** process, not primary vasculitis; steroids/cyclophosphamide worsen outcomes by impairing immune response | | Await cultures | Delays life-saving therapy; mortality increases with each hour of untreated IE | [cite:Harrison 21e Ch 124] 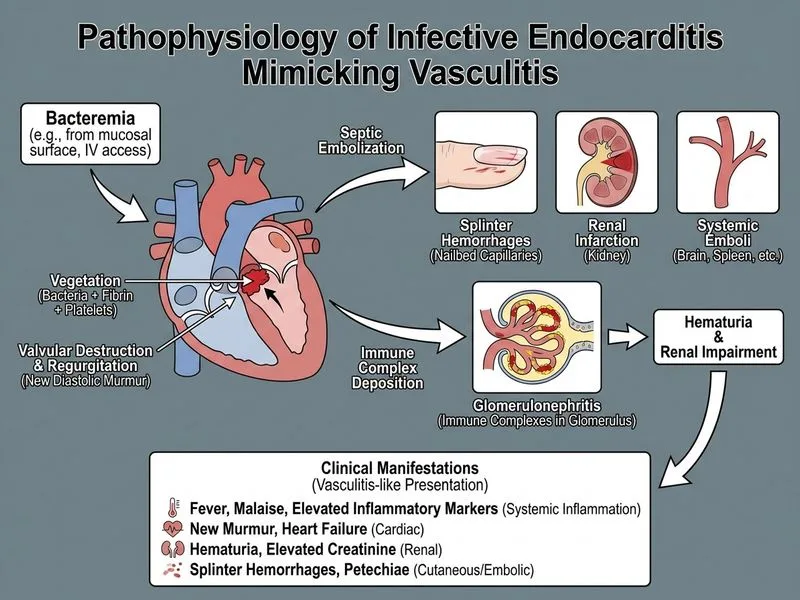
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.