## Clinical Diagnosis: Granulomatosis with Polyangiitis (GPA) ### Classic Presentation Triad **Key Point:** This patient has the pathognomonic triad of GPA: 1. **Upper respiratory tract involvement** (implied by hemoptysis source) 2. **Lower respiratory tract involvement** (bilateral infiltrates) 3. **Glomerulonephritis** (elevated creatinine, RBC casts, proteinuria) ### Serological Confirmation **High-Yield:** c-ANCA with anti-PR3 antibodies is **highly specific (>95%)** for GPA. In the presence of: - Clinical features consistent with systemic vasculitis - Positive c-ANCA/PR3 - Glomerulonephritis with RBC casts - Pulmonary involvement **Clinical Pearl:** Serology + clinical presentation is sufficient for diagnosis in GPA. Biopsy is NOT required before initiating treatment when serology and clinical features are diagnostic. ## Management Algorithm for GPA ```mermaid flowchart TD A[Suspected GPA with c-ANCA/PR3 positive]:::outcome --> B{Organ-threatening disease?}:::decision B -->|Yes: Pulmonary hemorrhage, renal failure| C[Induction therapy: High-dose corticosteroids + Cyclophosphamide]:::action B -->|No: Limited disease| D[Corticosteroids + Rituximab or Azathioprine]:::action C --> E[Pulse methylprednisolone 1g IV daily x 3 days]:::action E --> F[Oral prednisolone 1 mg/kg/day]:::action F --> G[Cyclophosphamide 0.5-1 g/m² IV monthly or daily oral]:::action G --> H[Plasmapheresis if pulmonary hemorrhage severe]:::action D --> I[Maintenance therapy at 3-6 months]:::action ``` ## Why Induction Therapy is Urgent **Key Point:** This patient has **organ-threatening disease**: - Serum creatinine 3.2 mg/dL = significant renal involvement - Hemoptysis + bilateral infiltrates = pulmonary involvement - Active urinary sediment = active glomerulonephritis **Warning:** Untreated GPA progresses rapidly to end-stage renal disease (ESRD) and respiratory failure. Delays in immunosuppression increase risk of irreversible organ damage. ### Induction Regimen for Organ-Threatening GPA | Component | Dosing | Duration | |-----------|--------|----------| | Methylprednisolone | 1 g IV daily | 3 days (pulse) | | Prednisolone | 1 mg/kg/day (max 80 mg) | Taper over 3–6 months | | Cyclophosphamide | 0.5–1 g/m² IV monthly OR 1.5–2 mg/kg/day oral | Until remission + 3 months | | Plasmapheresis | 7 sessions over 2 weeks | If pulmonary hemorrhage or Cr >5.8 mg/dL | [cite:Harrison 21e Ch 319] ## Why NOT the Other Options **Option 1 (Renal/pulmonary biopsy before treatment):** - Biopsy delays critical therapy in an organ-threatening disease - c-ANCA/PR3 serology + clinical features are diagnostic - Biopsy is reserved for seronegative cases or diagnostic uncertainty - Renal biopsy in active GN carries risk of worsening hematuria **Option 2 (Azathioprine monotherapy):** - Azathioprine is a **maintenance** agent, not induction therapy - Insufficient for organ-threatening disease requiring rapid immunosuppression - Cyclophosphamide is superior for induction (higher remission rates) - Azathioprine is used after remission is achieved with cyclophosphamide **Option 3 (Observation with repeat serology):** - Observation in organ-threatening vasculitis is contraindicated - GPA progresses rapidly to ESRD and pulmonary failure - Serology will not change management; clinical features mandate immediate treatment - Delay increases irreversible organ damage ## Mnemonic for GPA Diagnosis **Mnemonic: "GPA = c-ANCA + Granulomas + Glomerulonephritis"** - **c-ANCA/PR3** = cytoplasmic ANCA pattern - **Granulomas** = necrotizing granulomas on biopsy (if done) - **Glomerulonephritis** = necrotizing, crescentic GN [cite:Robbins 10e Ch 12; Park 26e Ch 7] 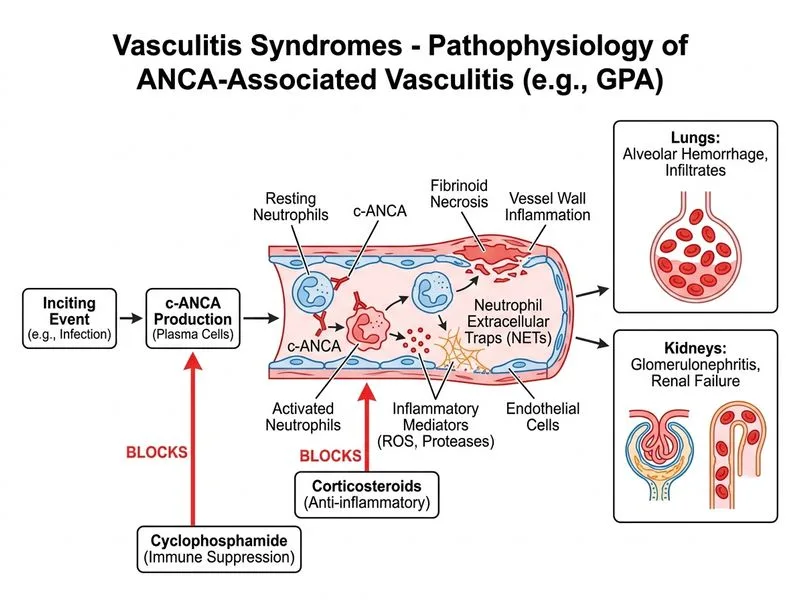
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.