## Clinical Diagnosis: Giant Cell (Temporal) Arteritis with Polymyalgia Rheumatica ### Key Clinical Features **Key Point:** Giant cell arteritis (GCA) is a large-vessel vasculitis affecting the aorta and its branches, particularly the temporal and ophthalmic arteries. It is the most common vasculitis in patients >50 years of age. This patient presents with the classic triad: 1. **Constitutional symptoms** — headache, malaise 2. **Cranial artery involvement** — temporal artery tenderness, jaw claudication, visual symptoms (amaurosis fugax or blindness) 3. **Systemic inflammation** — markedly elevated ESR (88 mm/h), elevated CRP 4. **Polymyalgia rheumatica** — morning stiffness in shoulders and hips (present in ~50% of GCA patients) ### Pathologic Hallmark **High-Yield:** Temporal artery biopsy showing **transmural inflammation with granulomatous infiltration and fragmentation of the internal elastic lamina** is the gold standard for diagnosis. This is a granulomatous vasculitis of large and medium vessels. ### Diagnostic Algorithm ```mermaid flowchart TD A[Age >50 + headache + jaw claudication]:::outcome --> B{Temporal artery tenderness?}:::decision B -->|Yes| C[Check ESR/CRP]:::action C --> D{Markedly elevated?}:::decision D -->|Yes| E[Temporal artery biopsy]:::action E --> F{Granulomatous transmural inflammation?}:::decision F -->|Yes| G[Giant Cell Arteritis]:::action F -->|No| H[Consider other diagnosis]:::outcome B -->|No| H D -->|No| H ``` ### Temporal vs. Takayasu Arteritis | Feature | Giant Cell Arteritis | Takayasu Arteritis | |---|---|---| | **Age of onset** | >50 years (typically 60–80) | <50 years (typically 10–40) | | **Ethnicity** | Caucasian predominance | Asian, Indian, Latin American | | **Vessels affected** | Temporal, ophthalmic, aortic arch | Aorta, subclavian, renal arteries | | **Presentation** | Headache, jaw claudication, vision loss | Arm claudication, absent pulses | | **Polymyalgia rheumatica** | Common (50%) | Rare | | **Biopsy finding** | Granulomatous transmural inflammation | Granulomatous aortitis | ### Clinical Pearl **Clinical Pearl:** **Jaw claudication** (pain in the jaw while chewing) is highly specific for temporal arteritis and should immediately raise suspicion. Visual symptoms (amaurosis fugax, diplopia, or permanent blindness) are ophthalmologic emergencies requiring urgent treatment with corticosteroids to prevent irreversible vision loss. ### Management Urgency **Warning:** Do not delay treatment while awaiting biopsy results if clinical suspicion is high. Corticosteroids should be initiated immediately to prevent vision loss, as the risk of blindness is ~15–20% if untreated. Biopsy can be performed within 1–2 weeks of starting steroids without significantly affecting diagnostic yield. 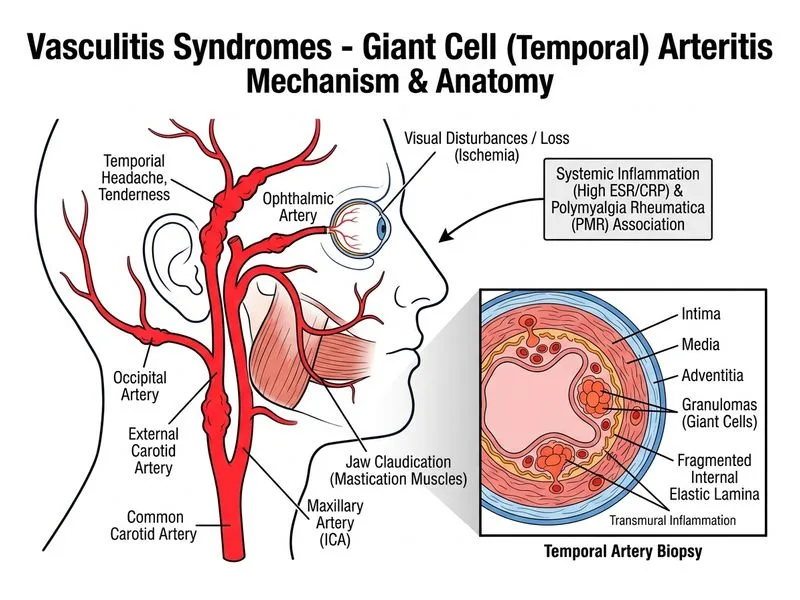
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.