## Clinical Diagnosis: Giant Cell Arteritis (Temporal Arteritis) The clinical presentation is classic for GCA: elderly patient with temporal artery tenderness, jaw claudication, elevated inflammatory markers (ESR >90), and ultrasound halo sign (hallmark finding). ## Management Priority **Key Point:** In suspected GCA with clinical and imaging evidence of active disease, corticosteroid therapy must be initiated immediately to prevent irreversible vision loss from arteritic anterior ischemic optic neuropathy (AAION). **High-Yield:** The risk of permanent blindness in untreated GCA is 40–50% within weeks. Delay in treatment for biopsy confirmation is NOT acceptable when clinical suspicion is high and imaging is supportive. ### Rationale for Immediate Steroid Therapy 1. **Clinical criteria met:** Temporal artery tenderness + jaw claudication + age >50 + elevated ESR 2. **Imaging confirmation:** Halo sign on ultrasound is highly specific (95%) for GCA 3. **Threat to vision:** Ophthalmic artery involvement can cause sudden, irreversible blindness 4. **Biopsy timing:** Temporal artery biopsy can be performed *after* steroid initiation (within 1–2 weeks) without loss of diagnostic sensitivity if steroids have been given for <2 weeks **Clinical Pearl:** The halo sign (hypoechoic ring around the temporal artery lumen on ultrasound) has replaced the need for immediate biopsy in many centers when clinical suspicion is high. Biopsy becomes confirmatory rather than gatekeeping. ### Steroid Dosing - **Induction:** Prednisolone 1 mg/kg/day (typically 40–60 mg/day) for 2–4 weeks - **Monitoring:** ESR/CRP at 1–2 weeks; taper based on clinical response and inflammatory markers - **Concurrent:** PPI, calcium + vitamin D, and bisphosphonate for osteoporosis prophylaxis [cite:Harrison 21e Ch 319] 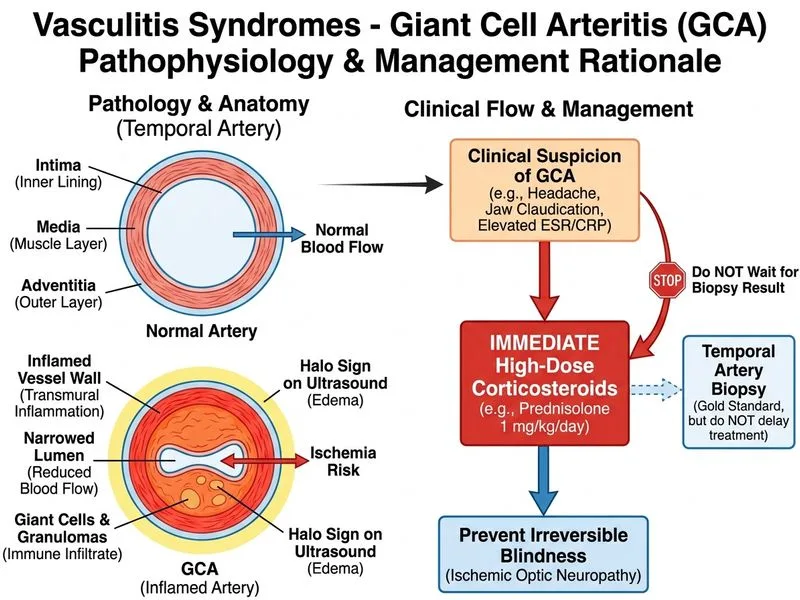
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.