## Distinguishing GPA from MPA ### Key Histopathological Differences **Key Point:** The hallmark discriminator between GPA and MPA is the presence of **granulomatous inflammation** in GPA, which is **absent in MPA**. ### Comparative Table | Feature | GPA | MPA | | --- | --- | --- | | **Granulomatous inflammation** | Present (necrotizing granulomas) | Absent | | **Necrotizing vasculitis** | Present (small & medium vessels) | Present (small vessels only) | | **Organ involvement** | Upper respiratory tract, lungs, kidneys | Kidneys, lungs (rarely upper RT) | | **ANCA type** | c-ANCA/PR3 (70–90%) | p-ANCA/MPO (70–80%) | | **Glomerulonephritis** | Necrotizing with crescents | Necrotizing with crescents | ### Pathological Mechanism **High-Yield:** GPA is characterized by the **triad**: 1. Necrotizing vasculitis of small and medium vessels 2. **Granulomatous inflammation** (the distinguishing feature) 3. Necrotizing glomerulonephritis MPA presents only necrotizing vasculitis of small vessels **without granulomas**. ### Clinical Pearl The presence of **necrotizing granulomas** in lung or upper respiratory tract biopsy in a patient with ANCA-positive vasculitis and glomerulonephritis is pathognomonic for GPA. MPA, by definition, lacks granulomatous inflammation. **Tip:** When comparing ANCA vasculitides on histology, always ask: "Are there granulomas?" If yes → GPA. If no → MPA or GPA-seronegative variant. [cite:Robbins 10e Ch 11] 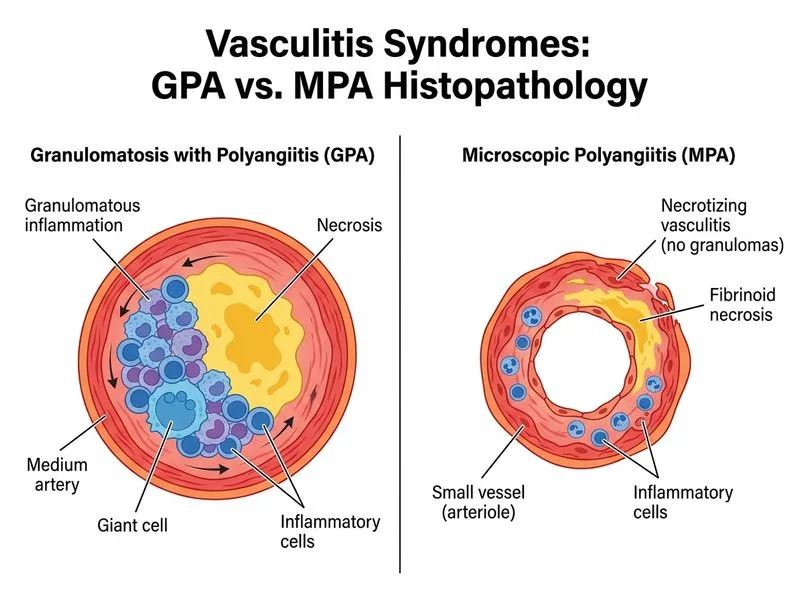
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.