## Clinical Context This patient presents with a **primary epigastric hernia** (midline defect in the linea alba above the pubis). The hernia is symptomatic (tender, irreducible), 4 cm in size, and the patient is a good surgical candidate with no comorbidities. ## Management Principles for Primary Ventral Hernias **Key Point:** Primary ventral/epigastric hernias >2 cm with symptoms warrant elective surgical repair to prevent incarceration and strangulation. Unlike inguinal hernias, ventral hernias carry a higher risk of incarceration (up to 10%) and have no natural history of resolution. ## Why Repair is Indicated Now 1. **Size:** 4 cm defect — larger defects have increased incarceration risk 2. **Symptoms:** Tenderness indicates local inflammation; irreducibility suggests tight fascial edges 3. **Location:** Epigastric hernias are prone to incarceration of omentum or bowel 4. **Healthy patient:** No contraindications to elective surgery ## Surgical Approach Selection | Approach | Indication | Advantage | Disadvantage | |----------|-----------|-----------|---------------| | **Open mesh (tension-free)** | Primary, uncomplicated, patient preference | Lower cost, familiar, good outcomes | Larger incision, longer recovery | | **Laparoscopic mesh** | Recurrent, multiple defects, cosmesis priority | Minimal access, faster recovery | Higher recurrence in primary (if not reinforced), cost | | **Robotic-assisted** | Recurrent, complex anatomy | Precision, minimal access | High cost, not first-line | **High-Yield:** For **primary ventral hernias** in healthy patients, **open tension-free mesh repair** is the gold standard and most cost-effective first-line approach. Laparoscopic repair is equally effective but reserved for recurrent hernias or patient preference for cosmesis. ## Why Each Distractor is Wrong ### Option 0: Observation with activity restriction - **Why wrong:** Symptomatic ventral hernias do NOT resolve spontaneously. Observation is appropriate only for **asymptomatic, small (<2 cm) hernias** in poor surgical candidates. This patient is symptomatic and a good candidate — delaying repair increases risk of incarceration and emergency surgery (which carries higher morbidity). ### Option 2: Laparoscopic repair - **Why wrong:** While laparoscopic repair is a valid option, it is NOT the "most appropriate" first-line for primary uncomplicated ventral hernias. Laparoscopic repair is preferentially used for **recurrent hernias** or when patient strongly desires minimal access. Open mesh is simpler, cheaper, and has equivalent long-term outcomes for primary repairs. Laparoscopic repair requires reinforcement with mesh on the visceral side (higher cost, longer operative time). ### Option 3: Watchful waiting with emergency repair only if incarceration develops - **Why wrong:** This is dangerous management. Incarcerated ventral hernias require **emergency surgery** with higher morbidity, mortality, and risk of bowel resection. Elective repair of a symptomatic hernia in a fit patient is always safer than gambling on emergency presentation. "Watchful waiting" is only appropriate for asymptomatic hernias in high-risk patients. ## Clinical Pearl **Incarceration risk in ventral hernias:** Up to 10% of ventral hernias incarcerate (vs. 0.3% for inguinal hernias). Emergency repair of incarcerated ventral hernia carries 5–10% mortality and 30–40% morbidity. Elective repair in a fit patient is strongly preferred. ## Mnemonic: REPAIR (When to operate on ventral hernia) - **R** — Recurrent (always repair) - **E** — Enlarging (>2 cm, repair electively) - **P** — Primary + symptomatic (repair electively) - **A** — Asymptomatic <2 cm (observe; repair if enlarges) - **I** — Incarceration risk high (repair urgently) - **R** — Recurrent + large (repair with mesh) ## Summary This patient requires **elective open tension-free mesh repair** — the gold standard for primary, uncomplicated ventral hernias in fit patients. 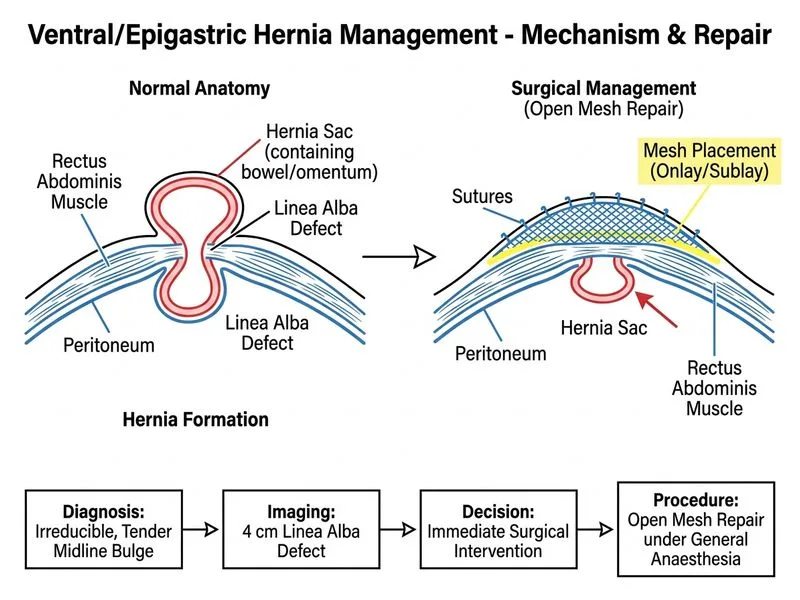
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.