## Clinical Diagnosis: HSV Stromal Keratitis **Key Point:** The history of prior dendritic ulcer, recurrent HSV infection, and **stromal infiltration with intact epithelium** indicates **HSV stromal keratitis (HSK)** — a delayed hypersensitivity immune response to viral antigen in the stroma, not active viral replication. ## Pathophysiology of HSV Stromal Keratitis ```mermaid flowchart TD A[Primary HSV Epithelial Infection]:::outcome --> B[Viral Antigen in Corneal Stroma]:::outcome B --> C{Immune Response Type}:::decision C -->|Acute: 2-4 weeks| D[Type III/IV Hypersensitivity]:::action C -->|Chronic: Months-Years| E[Immune Complex Deposition]:::action D --> F[Stromal Inflammation + Neovascularization]:::action E --> F F --> G[Dense Stromal Infiltrates + Scarring]:::outcome G --> H[Vision Loss + Potential Perforation]:::urgent ``` ## Differential Diagnosis: Epithelial vs. Stromal HSV Keratitis | Feature | Epithelial HSV | Stromal HSV (HSK) | |---------|---|---| | **Onset** | Acute (days) | Subacute to chronic (weeks–months) | | **Ulcer Pattern** | Dendritic or geographic | Intact epithelium | | **Stromal Involvement** | Minimal | Dense infiltrates, neovascularization | | **Corneal Sensation** | Reduced | Normal or near-normal | | **AC Reaction** | Mild (0–1+) | Moderate to severe (2–4+) | | **Pathology** | Active viral replication | Immune-mediated (Type III/IV hypersensitivity) | | **Treatment** | Antivirals alone (acyclovir) | **Antivirals + Topical Steroids** | | **Prognosis** | Good; heals in 7–10 days | Variable; risk of scarring & vision loss | **High-Yield:** HSV stromal keratitis is an **immune-mediated disease**, not active viral infection. Therefore, steroids are NOT contraindicated — they are ESSENTIAL to suppress the inflammatory response. However, steroids MUST be combined with systemic antivirals to prevent epithelial reactivation. ## Management of HSV Stromal Keratitis ### Step 1: Confirm Diagnosis - History of prior HSV epithelial disease - Stromal infiltration with intact epithelium - Normal or near-normal corneal sensation (rules out active epithelial disease) - Anterior chamber reaction (immune response) ### Step 2: Initiate Dual Therapy **Topical Prednisolone 1%:** - Frequency: 4–6 times daily initially, taper over 4–6 weeks - Mechanism: Suppresses Type III/IV hypersensitivity and inflammatory cytokines - Efficacy: Reduces stromal edema and neovascularization **Oral Acyclovir 400 mg:** - Frequency: 5 times daily for 10–14 days, then consider long-term prophylaxis (400 mg 2–3 times daily) - Mechanism: Prevents epithelial reactivation and viral shedding - Rationale: Steroids alone risk epithelial breakdown and geographic ulceration **Clinical Pearl:** The combination of topical steroid + systemic antiviral is the cornerstone of HSK management. Steroids without antivirals lead to epithelial disease; antivirals without steroids fail to resolve stromal inflammation. ### Step 3: Monitoring - Slit-lamp examination every 1–2 weeks - Monitor for epithelial breakdown (indicates need to reduce steroid dose) - Assess for stromal clearing and reduction in AC reaction - Long-term: Watch for corneal scarring and neovascularization ## Why This Is NOT the Other Diagnoses **Bacterial Keratitis:** - Bacterial keratitis presents with **epithelial defect** and **suppurative infiltrate** (not granular) - Rapid onset (24–48 hours) with severe pain - Corneal scraping would show bacteria on Gram stain - This patient has intact epithelium and prior HSV history — bacterial infection is unlikely **Fungal Keratitis:** - Fungal keratitis is rare in immunocompetent hosts without risk factors (contact lens trauma, topical steroid abuse) - Presents with **feathery infiltrate** and **satellite lesions** - Slow progression over weeks to months - KOH mount would be negative in HSK - No mention of risk factors in this case **Acyclovir-Resistant HSV:** - Rare in immunocompetent patients (<1% incidence) - Typically presents with **recurrent epithelial disease**, not stromal infiltration - Stromal disease in HSV is immune-mediated, not due to viral resistance - Switching to ganciclovir without steroids would fail to address the underlying immune pathology ## Long-Term Management **Key Point:** HSV stromal keratitis has a chronic course with risk of recurrence (up to 50% over 5 years). Long-term prophylaxis with oral acyclovir 400 mg 2–3 times daily reduces recurrence risk by ~50%. **Mnemonic: STEROID-ANTIVIRAL (S-A) Rule for HSK** - **S** = Steroids (topical, tapered over weeks) - **A** = Antivirals (systemic, long-term prophylaxis) - Together they prevent both immune-mediated stromal damage and viral reactivation **Warning:** Do NOT use steroids without antivirals in HSV disease — risk of epithelial breakdown and geographic ulceration. Do NOT use antivirals alone in HSK — stromal inflammation will persist. 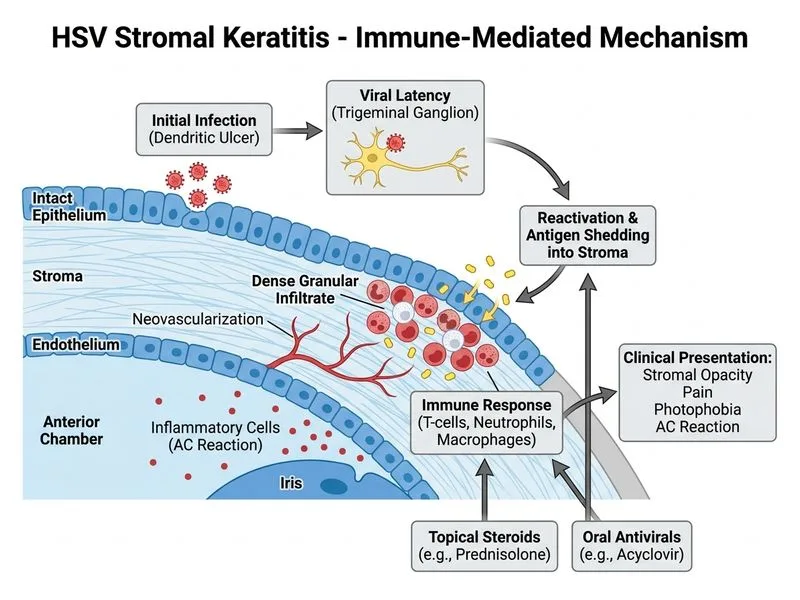
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.