## Diagnosis of Herpes Simplex Keratitis **Key Point:** PCR is the gold standard and most specific investigation for confirming HSV keratitis due to its high sensitivity and specificity. ### Investigation Comparison for Viral Keratitis | Investigation | Sensitivity | Specificity | Speed | Clinical Use | |---|---|---|---|---| | **PCR (corneal scrapings)** | 95–98% | 99–100% | 2–4 hours | Gold standard; confirmatory | | Giemsa staining | 50–60% | 70–80% | Rapid (15 min) | Screening; low sensitivity | | Viral culture | 70–80% | 100% | 3–7 days | Slow; rarely used now | | Confocal microscopy | 80–90% | Variable | Real-time | Morphological; not confirmatory | **High-Yield:** PCR detects viral DNA/RNA directly and is superior to culture and staining for rapid, definitive diagnosis. ### Clinical Pearl The **dendritic ulcer with terminal bulbs** is pathognomonic for HSV-1 keratitis. While clinical diagnosis is often sufficient to initiate topical antivirals (aciclovir, ganciclovir), PCR confirmation is essential for: - Atypical presentations - Recurrent keratitis (to rule out bacterial superinfection) - Research and epidemiological tracking - Medicolegal documentation **Warning:** Do not delay treatment while awaiting PCR results; begin topical antivirals immediately on clinical suspicion. PCR is confirmatory, not diagnostic in the acute setting. ### Why PCR is Superior 1. **Highest specificity:** Targets viral nucleic acid directly 2. **Rapid turnaround:** Results in hours, not days 3. **Detects latent/low-copy virus:** Positive even when culture is negative 4. **Multiplexing capability:** Can simultaneously test for HSV-1, HSV-2, VZV, CMV 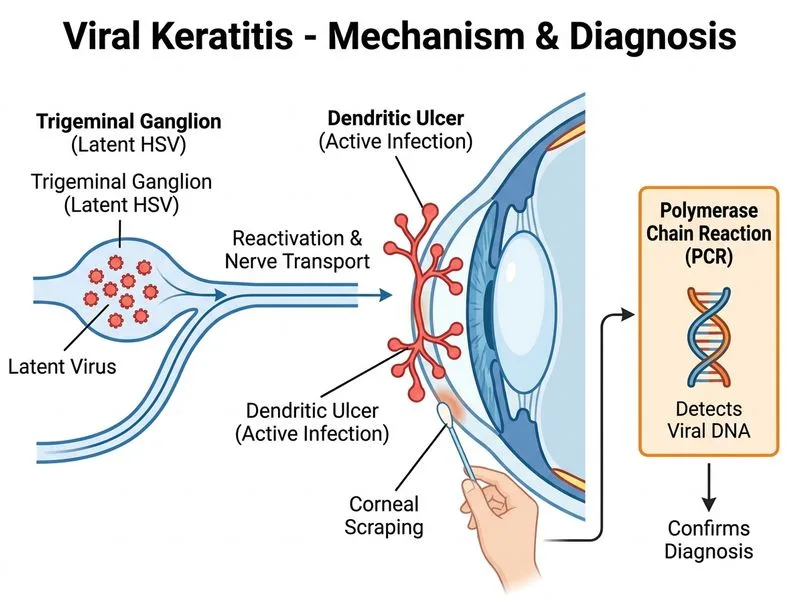
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.