## Clinical Diagnosis: HSV Stromal Keratitis The progression from epithelial disease to stromal opacity, neovascularization, and anterior uveitis 3 weeks into illness indicates **HSV stromal keratitis (HSK)**. This is an immune-mediated complication, not active viral replication. **Key Point:** Stromal keratitis is a delayed hypersensitivity reaction to viral antigen, NOT active epithelial infection. Treatment shifts from antivirals alone to combination antiviral + topical steroid. ## Pathophysiology of HSV Stromal Keratitis ```mermaid flowchart TD A[HSV epithelial infection]:::outcome --> B[Viral antigen in stroma]:::outcome B --> C[Immune complex deposition<br/>Type III hypersensitivity]:::outcome C --> D[Stromal inflammation<br/>neovascularization<br/>opacity]:::outcome D --> E{Treatment approach}:::decision E -->|Epithelial disease| F[Acyclovir alone]:::action E -->|Stromal disease| G[Acyclovir + topical steroid]:::action G --> H[Reduces inflammation<br/>Prevents scarring]:::outcome ``` ## Management of HSV Stromal Keratitis **High-Yield:** Topical steroids are ESSENTIAL in stromal HSK to suppress immune-mediated inflammation. They are contraindicated in epithelial disease but therapeutic in stromal disease. | Stage | Pathology | Treatment | Rationale | |-------|-----------|-----------|----------| | **Epithelial** | Active viral replication | Topical acyclovir ± oral acyclovir | Kill virus; steroids worsen | | **Stromal** | Immune complex inflammation | Topical acyclovir + prednisolone | Suppress inflammation; prevent scarring | | **Endothelial** | Immune keratouveitis | Acyclovir + high-dose prednisolone + systemic therapy | Preserve vision; prevent graft failure | ## Treatment Protocol for Stromal HSK 1. **Confirm epithelial healing:** Fluorescein staining should show no epithelial defect before initiating steroids. 2. **Topical prednisolone acetate 1%:** Start 4 times daily; taper over 4–12 weeks based on response. 3. **Continue topical acyclovir:** 5% ointment 3–4 times daily to suppress viral replication during immunosuppression. 4. **Oral acyclovir:** 400 mg 4–5 times daily for systemic suppression (reduces recurrence). **Clinical Pearl:** Steroid-induced IOP elevation is common in HSK; monitor intraocular pressure at each visit. Use lowest effective steroid dose and taper gradually. **Warning:** Abrupt steroid withdrawal can trigger rebound inflammation and scarring. Taper over weeks, not days. ## Why Combination Therapy Works - **Acyclovir:** Prevents epithelial reactivation and further viral antigen generation. - **Prednisolone:** Suppresses Type III hypersensitivity reaction, reduces neovascularization, and prevents stromal scarring. - Together: Synergistic effect; monotherapy (either agent alone) is suboptimal. [cite:Khurana Comprehensive Ophthalmology Ch 3; Yanoff & Duker Ophthalmology 5e Ch 4] 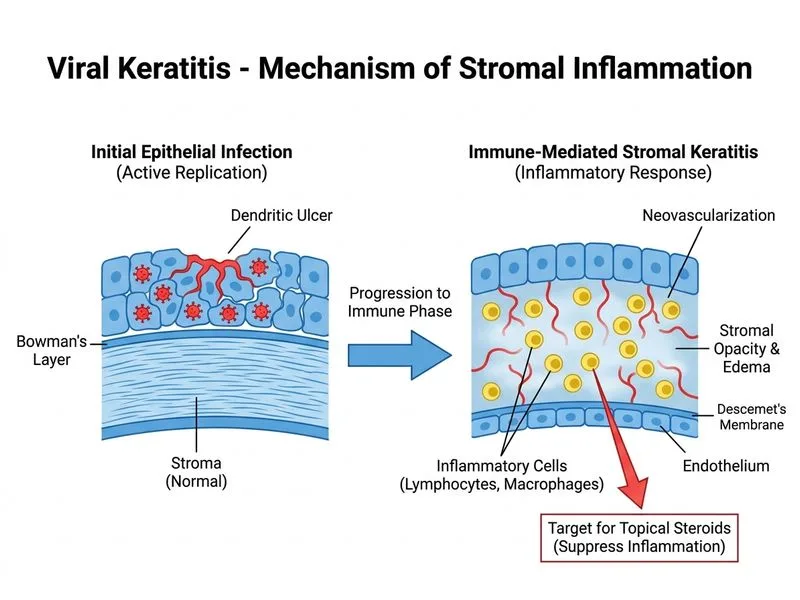
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.