## Clinical Presentation Analysis **Key Point:** Bilateral temporal hemianopia is a classic sign of compression of the optic chiasm from below (e.g., pituitary adenoma, craniopharyngioma, meningioma). ## Why MRI Brain with Contrast is the Investigation of Choice ### Anatomical Rationale 1. Optic chiasm compression occurs at the sella turcica level 2. Sagittal and coronal views specifically visualize the suprasellar region and chiasmal anatomy 3. Contrast enhancement delineates the lesion and its relationship to surrounding structures (cavernous sinus, internal carotid artery) ### Diagnostic Advantages - **Sensitivity:** >95% for detecting sellar/suprasellar masses - **Specificity:** Characterizes lesion type (pituitary adenoma, craniopharyngioma, meningioma) based on signal intensity and enhancement pattern - **Surgical planning:** Provides precise anatomical detail for neurosurgical approach **High-Yield:** Bilateral temporal hemianopia = chiasmal compression until proven otherwise. MRI is the gold standard confirmatory test. ## Differential Diagnosis of Bitemporal Hemianopia | Lesion | Location | MRI Finding | Additional Feature | |--------|----------|-------------|--------------------| | Pituitary adenoma | Intrasellar | Hypointense on T1, enhancement post-contrast | Hormonal symptoms may occur | | Craniopharyngioma | Suprasellar | Cystic + solid, calcification on CT | Childhood presentation common | | Meningioma | Suprasellar | Dural tail sign, homogeneous enhancement | Broad dural base | | Aneurysm | Anterior communicating artery | Flow void on MRI, CTA better | Subarachnoid hemorrhage risk | **Clinical Pearl:** The patient's normal fundoscopy does not exclude chiasmal compression—optic atrophy develops only after chronic compression. Early detection via MRI prevents permanent vision loss. 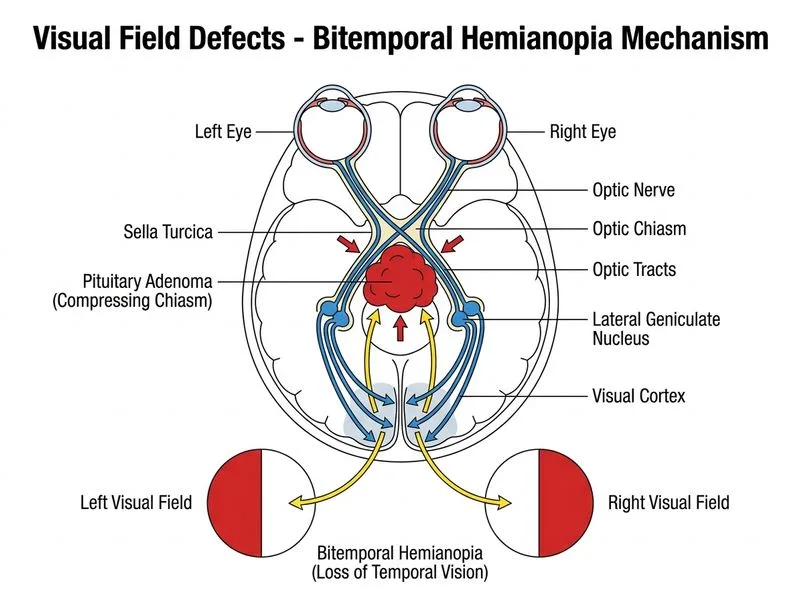
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.