## Clinical Diagnosis This patient presents with **optic neuritis** or **demyelinating optic neuropathy** with features suggesting possible **intracranial pathology**: - Unilateral optic disc swelling (pale, elevated, blurred margins) - Progressive peripheral scotoma with nasal step (non-glaucomatous pattern) - Normal IOP (excludes glaucoma) - Expanding visual field defect over 2 months - Age and demographics suggest demyelinating disease or structural lesion ## Differential Diagnosis of Optic Disc Swelling with Visual Field Loss | Feature | Optic Neuritis | Papilledema | Anterior Ischemic Optic Neuropathy | Compressive Lesion | |---------|---|---|---|---| | IOP | Normal | Normal | Normal | Normal | | Disc appearance | Pale, blurred | Hyperemic, blurred | Sectoral pallor | May be normal initially | | VF defect | Central scotoma, peripheral | Peripheral constriction | Altitudinal | Depends on location | | Progression | Acute to subacute | Gradual | Acute | Gradual | | MRI finding | Optic nerve enhancement | Raised ICP | Ischemia | Mass lesion | ## Pathophysiology of Visual Field Defect The **nasal step pattern with peripheral scotoma** suggests: 1. Demyelination affecting the optic nerve (optic neuritis) 2. Compression from intracranial mass (pituitary, meningioma, glioma) 3. Inflammation extending from the optic nerve sheath Unlike glaucomatous arcuate defects, this pattern is non-glaucomatous and requires neuroimaging to exclude structural or inflammatory causes. ## Management Algorithm ```mermaid flowchart TD A[Unilateral optic disc swelling + VF loss]:::outcome --> B{IOP elevated?}:::decision B -->|Yes| C[Glaucoma]:::outcome B -->|No| D[Non-glaucomatous optic neuropathy]:::outcome D --> E{Acute or progressive?}:::decision E -->|Acute + young| F[Optic neuritis]:::outcome E -->|Progressive + older| G[Consider demyelination or compression]:::outcome F --> H[MRI brain and orbits with gadolinium]:::action G --> H H --> I[Assess for demyelinating disease or mass]:::action I --> J[Treat underlying cause]:::action ``` ## Key Point: **Unilateral optic disc swelling with normal IOP and non-glaucomatous visual field defect requires urgent MRI to exclude demyelinating disease (optic neuritis, MS) or intracranial compression.** Gadolinium contrast is essential to demonstrate optic nerve enhancement (optic neuritis) or mass lesions. ## High-Yield: - **Nasal step + peripheral scotoma** = non-glaucomatous pattern - **Pale disc + blurred margins + normal IOP** = demyelinating optic neuropathy or compression - **Progressive over 2 months** = suggests inflammation or slow-growing lesion, not acute ischemia - **MRI with gadolinium** = gold standard for optic neuritis and structural lesions ## Clinical Pearl: Optic neuritis is the presenting symptom of multiple sclerosis in 15–20% of MS patients. Early MRI with gadolinium not only confirms the diagnosis but also provides prognostic information (presence of brain lesions predicts higher risk of MS conversion). In older patients, progressive optic neuropathy with disc swelling should raise suspicion for compressive lesions (pituitary adenoma, meningioma). ## Warning: **Do NOT assume normal IOP excludes serious pathology.** Glaucoma is ruled out, but demyelinating disease and intracranial lesions can present with identical optic disc findings and normal IOP. MRI is mandatory. ## Tip: The **nasal step pattern** is a red flag for non-glaucomatous pathology. Remember: glaucomatous defects are arcuate/altitudinal; non-glaucomatous defects (optic neuritis, compression, ischemia) often have different patterns (central scotoma, nasal step, peripheral constriction). [cite:Harrison 21e Ch 376; Neuro-Ophthalmology Review Manual Ch 3] 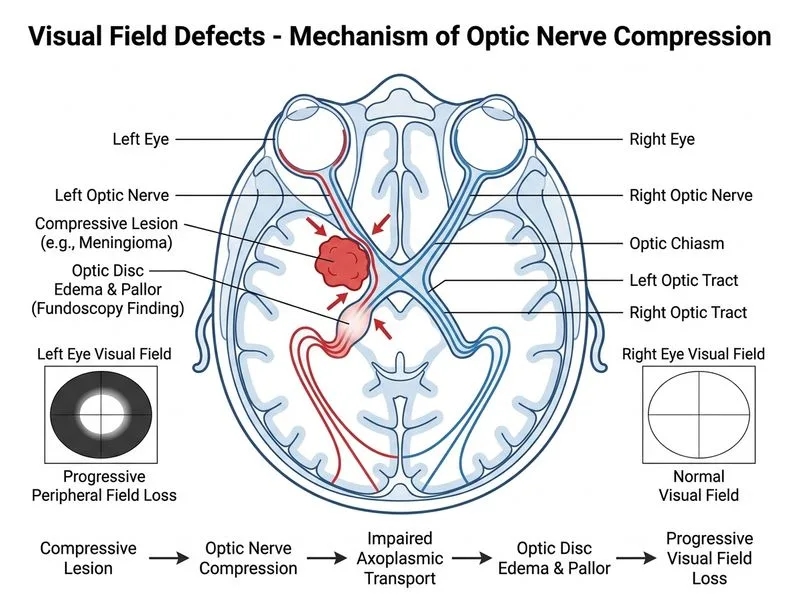
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.