## Clinical Presentation Analysis This patient has: - **Homonymous hemianopia** (loss of the same visual field in both eyes — right half in this case) - Sudden onset - Normal fundoscopy (no retinal pathology) - Normal neurologic examination otherwise - No headache or focal neurologic deficits **Key Point:** Homonymous hemianopia indicates a **post-chiasmal lesion** (optic tract, lateral geniculate nucleus, optic radiations, or occipital cortex). The sudden onset with no other neurologic signs raises concern for **acute ischemic or hemorrhagic stroke** affecting the visual cortex or optic radiations. ## Pathophysiology of Homonymous Hemianopia ```mermaid flowchart TD A[Homonymous hemianopia]:::outcome --> B[Post-chiasmal lesion]:::outcome B --> C{Acute onset?}:::decision C -->|Yes| D[Stroke - ischemic or hemorrhagic]:::urgent C -->|No| E[Chronic lesion - tumor, demyelination]:::outcome D --> F[MRI brain DWI is gold standard]:::action F --> G{DWI positive?}:::decision G -->|Yes| H[Acute ischemic stroke - thrombolysis/thrombectomy window?]:::action G -->|No| I[Hemorrhage or other pathology - CT may have missed]:::action ``` **High-Yield:** In acute homonymous hemianopia, **MRI with DWI is superior to CT** because: 1. DWI detects ischemic stroke within **minutes** of symptom onset (CT may be falsely negative in first 6–12 hours) 2. MRI also evaluates for hemorrhage, mass, and demyelination 3. Time-to-treatment is critical; DWI guides thrombolysis/thrombectomy eligibility ## Why MRI DWI is the Best Next Step **Clinical Pearl:** A patient with sudden homonymous hemianopia is a **stroke until proven otherwise**. Even without other focal neurologic signs, the visual cortex or optic radiations can be selectively affected by a small stroke in the territory of the posterior cerebral artery (PCA) or middle cerebral artery (MCA). **Mnemonic: STROKE WINDOW — DWI detects ischemia within minutes; CT detects only hemorrhage and large infarcts.** | Imaging Modality | Sensitivity in Acute Ischemia | Time to Diagnosis | Best For | |---|---|---|---| | CT (non-contrast) | <10% in first 6 hours | Minutes | Excluding hemorrhage | | MRI DWI | >95% within minutes | 20–30 minutes | Detecting acute ischemia; guiding thrombolysis | | CT perfusion | Moderate; shows mismatch | 10–15 minutes | Identifying salvageable tissue | **Tip:** In suspected acute stroke, **MRI DWI is the gold standard** for detecting ischemia. If MRI is contraindicated, CT perfusion or CT angiography may be used, but DWI is preferred. ## Why Other Options Are Incorrect | Option | Why It's Wrong | |--------|----------------| | Reassure and discharge | Homonymous hemianopia is a stroke symptom. Discharging without imaging risks missing acute ischemic stroke in the thrombolysis window (4.5 hours) or thrombectomy window (24 hours). | | Non-contrast CT head | CT is insensitive for acute ischemic stroke in the first 6–12 hours. It is useful for excluding hemorrhage but will miss most acute infarcts. MRI DWI is far superior. | | EEG and seizure prophylaxis | Seizures are not the primary concern here. The sudden homonymous hemianopia is a stroke symptom, not a seizure manifestation. EEG is not indicated as a first-line investigation. | **Warning:** Do not confuse **homonymous hemianopia** (post-chiasmal, suggests stroke) with **bitemporal hemianopia** (chiasmal compression, suggests pituitary tumor or optic chiasm lesion). [cite:Harrison 21e Ch 427, Neuro-Ophthalmology Illustrated 3e Ch 3] 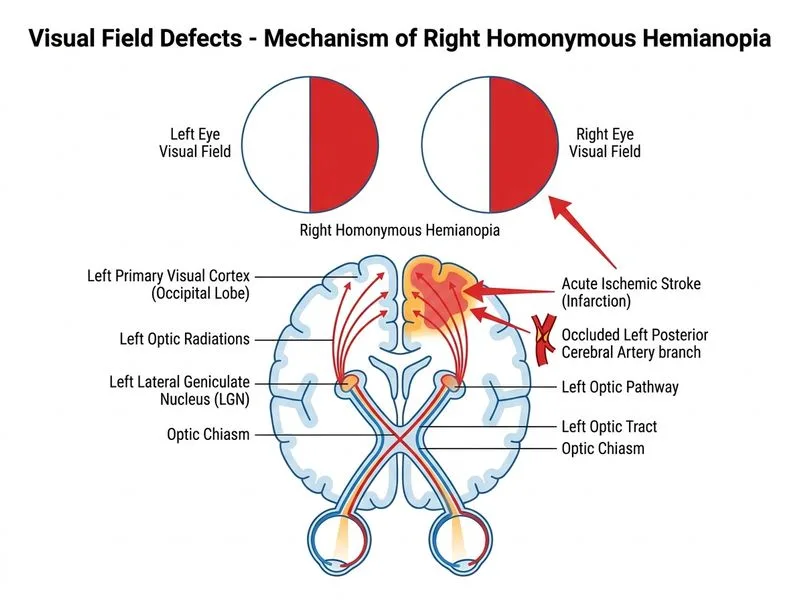
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.