## Arteritic vs. Non-Arteritic AION: Inflammatory Markers as Discriminator ### Clinical Context **Key Point:** Systemic inflammatory markers (ESR and CRP) are the best discriminating feature between arteritic AION (A-AION, due to giant cell arteritis) and non-arteritic AION (NA-AION, due to atherosclerotic vascular disease). ### Comparison Table | Feature | Arteritic AION (A-AION) | Non-Arteritic AION (NA-AION) | |---------|------------------------|------------------------------| | **Cause** | Giant cell arteritis (GCA) | Atherosclerosis, hypertension, diabetes | | **ESR** | Markedly elevated (>50 mm/h) | Normal or mildly elevated (<30 mm/h) | | **CRP** | Elevated (>2.4 mg/dL) | Normal or mildly elevated | | **Age** | >60 years (typically >70) | >50 years (mean ~65) | | **Systemic symptoms** | Temporal headache, jaw claudication, PMR, fever | Absent | | **Visual field defect** | Altitudinal | Altitudinal | | **Optic disc appearance** | Pale, atrophic | Pale, atrophic | | **APD** | Present | Present | | **Prognosis without treatment** | Risk of fellow eye involvement (50% in 2 weeks) | Stable, low risk of fellow eye | | **Temporal artery biopsy** | Positive (granulomatous inflammation) | Negative | ### Why Inflammatory Markers Discriminate 1. **A-AION is a systemic vasculitis:** Giant cell arteritis causes inflammation of medium and large arteries, including the posterior ciliary arteries supplying the optic nerve head. 2. **Marked elevation of ESR/CRP:** Reflects active systemic inflammation; ESR typically >50 mm/h and CRP >2.4 mg/dL. 3. **NA-AION is vascular insufficiency:** Results from atherosclerotic narrowing or thrombosis of the posterior ciliary arteries without systemic inflammation. 4. **Normal or mildly elevated markers in NA-AION:** ESR and CRP remain normal or only minimally elevated. **High-Yield:** ESR >50 mm/h in a patient >60 years with sudden vision loss and optic disc ischemia strongly suggests A-AION and mandates urgent temporal artery biopsy and corticosteroid therapy to prevent fellow-eye involvement. **Mnemonic:** **GCA = Giant Cell Arteritis** — think **G**reat **C**RP, **A**lways elevated ESR. **Clinical Pearl:** A-AION is a medical emergency because ~50% of untreated patients develop vision loss in the fellow eye within 2 weeks. Immediate corticosteroid therapy (often without waiting for biopsy confirmation) is indicated if clinical suspicion is high and inflammatory markers are elevated. ### Why Other Features Are Not Discriminating - **Altitudinal visual field defect:** Occurs in both A-AION and NA-AION; not discriminating. - **Afferent pupillary defect:** Present in both; reflects optic nerve damage, not etiology. - **Age >60 years:** Both conditions occur in this age group; A-AION typically >70, but NA-AION also common >60. Overlap is substantial. ### Temporal Artery Biopsy: Gold Standard While temporal artery biopsy is the gold standard for confirming GCA, inflammatory markers (ESR/CRP) are the practical discriminator at the bedside and guide urgent treatment decisions. [cite:Harrison 21e Ch 427; Neuro-Ophthalmology, Ischemic Optic Neuropathy] 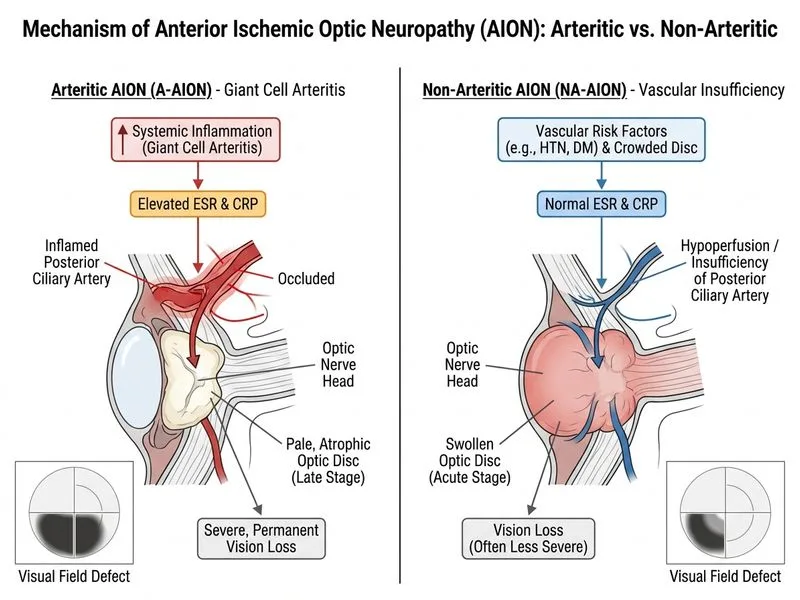
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.