## Diagnosis: Vitamin A Deficiency — Stage XN (Night Blindness) **Key Point:** Night blindness is the **earliest clinical manifestation** of vitamin A deficiency and occurs before any visible conjunctival or corneal changes. It reflects impaired synthesis of rhodopsin (visual purple), the rod photopigment essential for low-light vision. **High-Yield:** In population-based screening for vitamin A deficiency in endemic areas, night blindness is the most sensitive early indicator. A history of difficulty seeing at dusk or inability to navigate in dim light should immediately raise suspicion for VAD, even when the anterior segment appears normal under bright light. ### Biochemistry: Why Night Blindness Occurs First **Vitamin A (Retinol) → Retinal (Retinaldehyde) → Rhodopsin Formation** 1. Vitamin A is converted to retinal in the retinal pigment epithelium (RPE) 2. Retinal combines with opsin to form **rhodopsin**, the visual pigment in rod photoreceptors 3. Rhodopsin is exquisitely sensitive to light and enables vision in low-illumination conditions 4. With depleted vitamin A stores, rhodopsin synthesis declines → rods become non-functional → night blindness 5. Rod dysfunction precedes cone dysfunction because cones require less vitamin A and are more resistant to deficiency **Clinical Pearl:** Dark adaptation testing (measuring time for visual threshold to improve in darkness) is prolonged in VAD because rod regeneration of rhodopsin is impaired. This is a sensitive functional test before structural changes appear. ### Timeline of Xerophthalmia Progression ```mermaid flowchart LR A["Stage XN<br/>Night Blindness<br/>(Earliest)"]:::outcome --> B["Stage X1A<br/>Conjunctival Xerosis"]:::outcome B --> C["Stage X1B<br/>Bitot's Spots"]:::outcome C --> D["Stage X2<br/>Corneal Xerosis/Haze"]:::outcome D --> E["Stage X3A<br/>Corneal Ulceration"]:::urgent E --> F["Stage XS<br/>Corneal Scar<br/>(Permanent Blindness)"]:::urgent G["Vitamin A Supplementation"]:::action -.->|Reverses if given early| B G -.->|Reverses if given early| C G -.->|Reverses if given early| D G -.->|May prevent progression| E G -.->|Cannot reverse| F ``` **Warning:** Parents often attribute night blindness to "normal childhood behavior" or dismiss it as the child being "timid in the dark." A careful history of specific inability to navigate or recognize people in dim light is the key diagnostic clue. ### WHO Diagnostic Criteria for Night Blindness (XN) - History of difficulty seeing in dim light or inability to navigate in darkness - Normal anterior segment on bright illumination - Prolonged dark adaptation time (>5 minutes to reach threshold) - **Reversible with vitamin A supplementation within days** **Mnemonic: ABCDE of Xerophthalmia** — **A** (night blindness/Adaptation defect), **B** (Bitot's spots), **C** (Corneal xerosis), **D** (corneal Defect), **E** (End-stage scar). ### Management of Stage XN - **Vitamin A 200,000 IU orally** on day 1, day 2, and day 15 (same as other stages) - Night blindness typically resolves within **3–7 days** of starting supplementation - Dietary counselling: increase vitamin A-rich foods (eggs, liver, dark leafy greens, orange vegetables) - No topical therapy needed at this stage - Prognosis: **100% reversible** if treated early 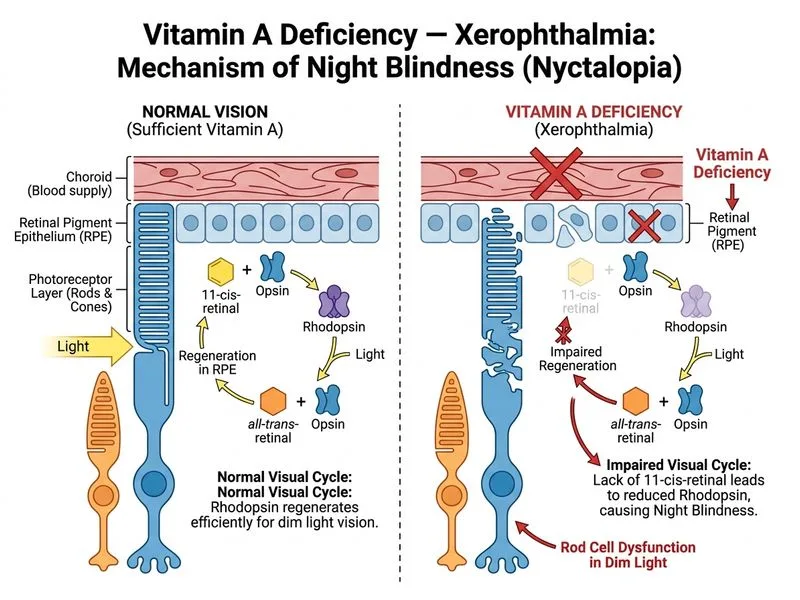
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.