## Clinical Diagnosis: Pancoast Tumor with RLN Invasion ### Presentation Analysis The patient presents with: - **Lung apex mass** (Pancoast tumor) invading RLN - **Left vocal cord fixed in paramedian position** - **Visible mass at vocal cord margin** (direct tumor involvement) - **Hoarseness, dysphagia, weight loss** (malignancy features) - **Smoking history** (lung cancer risk) ### Key Point: **The recurrent laryngeal nerve (RLN) innervates ALL intrinsic laryngeal muscles EXCEPT the cricothyroid (innervated by external branch of SLN).** RLN paralysis leaves the cord in a paramedian position because: 1. Loss of abductor function (posterior cricoarytenoid) → cord cannot abduct 2. Loss of adductor function (lateral cricoarytenoid, interarytenoid) → cord cannot fully adduct 3. **Net result: passive paramedian resting position** ### Anatomy of Laryngeal Innervation | Nerve | Muscles Innervated | Effect of Paralysis | | --- | --- | --- | | **RLN** | PCA, LCA, IA, TA | Paramedian position; weak voice; aspiration risk | | **SLN (ext. branch)** | Cricothyroid | Loss of pitch control; voice fatigue | | **SLN (int. branch)** | Sensory above vocal cords | Loss of cough reflex | **Mnemonic for RLN muscles: PLAIT** - **P**osterior cricoarytenoid (abductor) - **L**ateral cricoarytenoid (adductor) - **A**rytenoid (interarytenoid — adductor) - **I**nterarytenoid (transverse — adductor) - **T**hyroarytenoid (adductor + tensor) ### High-Yield: **Pancoast tumor (lung apex malignancy) is a classic cause of RLN paralysis via direct invasion or compression.** The RLN ascends from the thorax on the left side, looping under the aortic arch; left lung apex tumors can directly invade it. ### Clinical Pearl: **Horner syndrome (ptosis, miosis, anhidrosis) + VCP + arm pain = Pancoast tumor until proven otherwise.** This patient does not have Horner syndrome documented, but the combination of RLN paralysis + lung apex mass is pathognomonic for Pancoast. ### Why RLN Paralysis → Paramedian Position? ```mermaid flowchart TD A[RLN Paralysis]:::outcome --> B[Loss of PCA function]:::action A --> C[Loss of LCA/IA function]:::action B --> D[Cannot abduct cord]:::action C --> E[Cannot fully adduct cord]:::action D --> F[Cord rests in paramedian position]:::outcome E --> F F --> G[Incomplete glottic closure]:::outcome G --> H[Breathy voice + aspiration]:::outcome ``` ### Contrast: SLN Paralysis - **External branch SLN** → cricothyroid paralysis → loss of pitch control, voice fatigue, but **cord position normal** (cord lies in lateral position due to unopposed RLN abductors) - **Internal branch SLN** → sensory loss above cords → loss of cough reflex, aspiration risk ### Management of Pancoast with VCP 1. **Oncologic:** Concurrent chemoradiation ± surgery (Paulson procedure) 2. **Laryngeal:** Voice therapy; consider injection laryngoplasty if persistent VCP after cancer treatment 3. **Airway:** Monitor for aspiration; swallow evaluation [cite:Harrison 21e Ch 29; Robbins & Cotran 10e Ch 16] 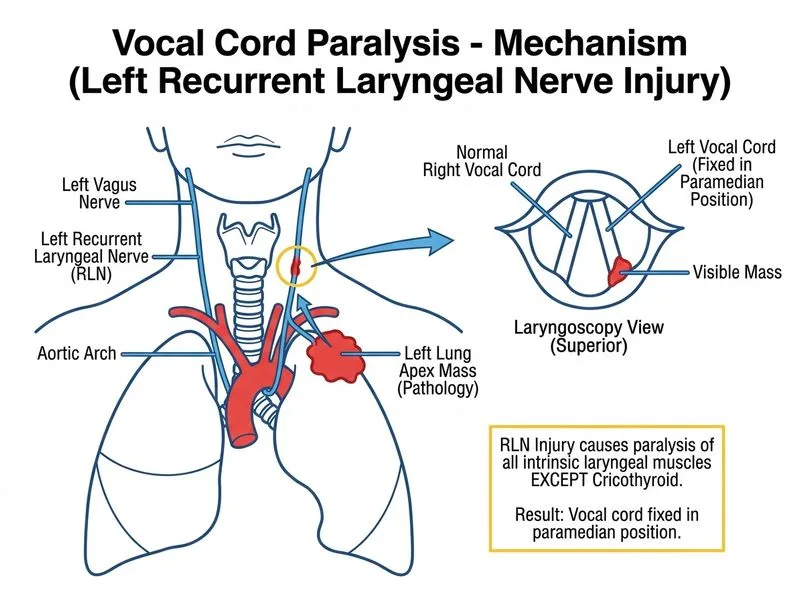
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.