Surgical Anatomy: Inguinal Canal, Hernias & Landmarks for NEET PG — Complete Guide 2026
Master inguinal canal anatomy and hernia repair for NEET PG 2026: boundaries, contents, Hesselbach triangle, direct vs indirect hernia, femoral hernia (highest strangulation), Lichtenstein vs Shouldice vs Bassini vs TEP/TAPP, and special hernias (Richter, Amyand, Littre, sliding).
Version 1.0 — Published April 2026
Quick Answer
Hernias and inguinal anatomy contribute 3–4 direct questions per NEET PG paper. Master these 10 high-yield areas:
- Inguinal canal — 4 cm oblique passage; deep ring at midpoint of inguinal ligament, 1–1.5 cm above femoral pulse; superficial ring above pubic tubercle
- Walls mnemonic (MALT) — Anterior: external oblique + internal oblique (lat 1/3). Posterior: transversalis fascia + conjoint tendon (medial 1/3). Floor: inguinal + lacunar ligaments. Roof: conjoint tendon arch
- Contents — spermatic cord (3 arteries, 3 nerves, 3 layers) in males; round ligament in females; ilioinguinal nerve outside the cord
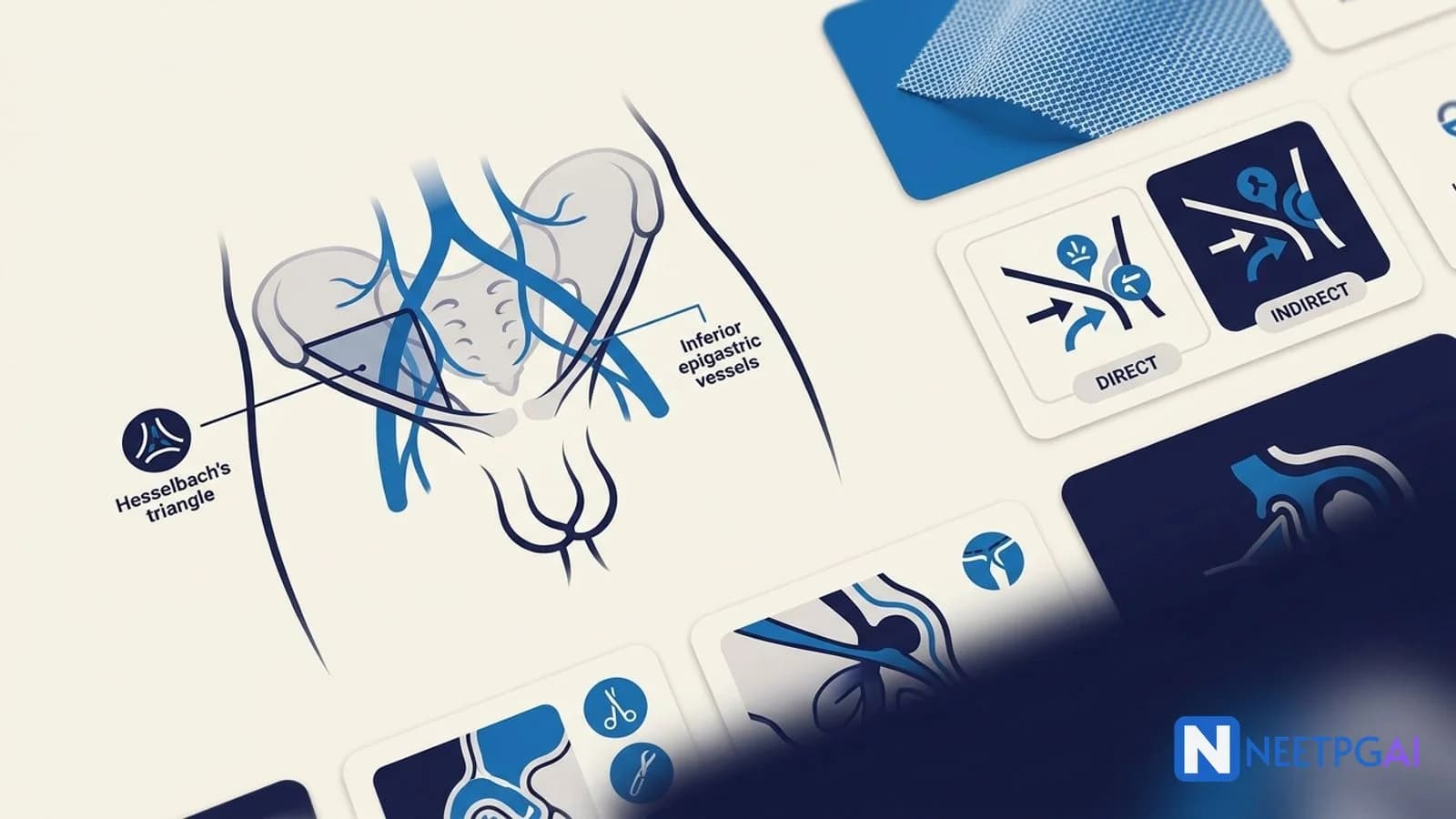
- Hesselbach triangle — medial: rectus lateral border. Lateral: inferior epigastric artery. Inferior: inguinal ligament. Direct hernia exits here (medial to inferior epigastric)
- Direct vs indirect — indirect: lateral to IE vessels, congenital, into scrotum. Direct: medial to IE vessels, acquired, rarely scrotal. Deep ring occlusion test
- Femoral hernia — through femoral canal below inguinal ligament; narrowest, rigid boundaries; highest strangulation risk (~40%); F>M
- Open repairs — Bassini (tissue, 3-layer, high recurrence), Shouldice (4-layer imbricated, best tissue), Lichtenstein (tension-free mesh, gold standard)
- Laparoscopic repairs — TEP (totally extraperitoneal) and TAPP (transabdominal preperitoneal); equal recurrence, less chronic pain
- Umbilical/paraumbilical — infants: most close by 5 yr (conservative); adults: Mayo operation or mesh; paraumbilical (acquired, obese, multiparous)
- Special hernias — Richter (partial wall, strangulates without obstruction), Amyand (contains appendix), Littre (Meckel), Sliding (viscus forms part of sac wall), Obturator (elderly F, Howship-Romberg)
Surgical anatomy of the inguinal region is the application of detailed regional anatomy to the diagnosis and repair of groin hernias, and it is a perennial NEET PG goldmine across surgery and anatomy. The student who memorises canal boundaries, Hesselbach triangle, and the direct-vs-indirect distinction covers 3–4 marks per exam. Pair this guide with daily MCQ practice on the surgery subject hub, cross-reference the surgery high-yield topics overview, and revise the common mistakes in surgery guide for classic distractor traps.
Inguinal canal — boundaries and dimensions
The inguinal canal is a 4 cm oblique intermuscular passage in the lower anterior abdominal wall that transmits the spermatic cord in males and the round ligament in females.
Dimensions and orientation:
- Length: ~4 cm
- Direction: downward, medially, and forward from deep ring to superficial ring
- Position: parallel to and just above the medial half of the inguinal ligament
Openings:
| Ring | Location | Structure |
|---|---|---|
| Deep (internal) ring | Midpoint of inguinal ligament; 1–1.5 cm above the midpoint between ASIS and pubic symphysis (approximately over the femoral pulse plus 1.5 cm superior) | Opening in transversalis fascia |
| Superficial (external) ring | Triangular opening in external oblique aponeurosis; above and medial to pubic tubercle | Bounded by medial and lateral crura + intercrural fibres |
Note on surface anatomy: The classic landmark is "midpoint of inguinal ligament" (ASIS to pubic tubercle) for the deep ring. The "mid-inguinal point" (ASIS to pubic symphysis) is the landmark for the femoral artery — these are often confused and heavily tested.
Walls (MALT mnemonic for the student who likes acronyms):
| Wall | Lateral third | Medial third |
|---|---|---|
| Anterior | External oblique aponeurosis + internal oblique muscle | External oblique aponeurosis only |
| Posterior | Transversalis fascia | Transversalis fascia + conjoint tendon |
| Floor | Inguinal ligament (Poupart) | Inguinal ligament + lacunar ligament (Gimbernat) |
| Roof | Arching fibres of internal oblique and transversus abdominis (conjoint tendon) | Arching fibres |
Conjoint tendon = fusion of lower fibres of internal oblique and transversus abdominis, inserting on pubic tubercle and pectineal line. It is the key strengthening structure medially.
Contents of the inguinal canal
The inguinal canal contains the spermatic cord in males (round ligament in females) along with the ilioinguinal nerve running alongside but outside the internal spermatic fascia.
Spermatic cord (male) — the "3-3-3" rule:
| Category | Contents |
|---|---|
| 3 arteries | Testicular (from aorta), cremasteric (from inferior epigastric), artery to vas deferens (from superior/inferior vesical) |
| 3 nerves | Genital branch of genitofemoral, sympathetic plexus, ilioinguinal (OUTSIDE the cord, within the canal) |
| 3 fascial layers | Internal spermatic fascia (from transversalis fascia), cremasteric fascia (from internal oblique + transversus), external spermatic fascia (from external oblique) |
| 3 other | Vas deferens, pampiniform venous plexus, lymphatics, obliterated processus vaginalis |
Female inguinal canal contents:
- Round ligament of the uterus (from uterine horn to labium majus)
- Ilioinguinal nerve
- Genital branch of genitofemoral nerve
- Small artery accompanying round ligament (artery of Sampson)
Clinical relevance:
- Cremasteric reflex — stroking medial thigh → cremaster contracts → testis elevates (L1-L2; genitofemoral nerve efferent)
- Ilioinguinal nerve can be injured during hernia repair → neuralgia, numbness over medial thigh / scrotum / labium; genital branch of genitofemoral supplies cremaster and anterior scrotum
Hesselbach triangle and hernia anatomy
Hesselbach triangle (inguinal triangle) is the anatomical area on the posterior wall of the inguinal canal where direct hernias protrude — bounded by three well-tested landmarks.
Boundaries:
- Medial: lateral border of rectus abdominis (linea semilunaris)
- Lateral: inferior epigastric artery (key landmark)
- Inferior: inguinal ligament (Poupart)
Inferior epigastric artery is the single most important landmark for hernia classification:
- Direct hernia → medial to IE vessels (through Hesselbach triangle)
- Indirect hernia → lateral to IE vessels (through deep ring)
Floor of Hesselbach triangle:
- Transversalis fascia (only; no muscular support)
- This is the weakest part of the groin and the site of direct hernia
- Conjoint tendon overlies and strengthens it
Myopectineal orifice of Fruchaud:
- Single weak area through which all groin hernias pass (inguinal direct, indirect, femoral)
- Bounded above by internal oblique/transversus arch, below by pubic ramus and pectineal ligament, medially by rectus, laterally by iliopsoas
- Divided by the inguinal ligament into suprainguinal (inguinal hernias) and infrainguinal (femoral hernia)
- Underlies the logic of preperitoneal mesh repair (TEP / TAPP) covering all three potential defects with one mesh
Direct vs indirect inguinal hernia
Direct and indirect hernias are both inguinal but anatomically and clinically distinct — and the NEET PG single best answer almost always hinges on the inferior epigastric relationship.
| Feature | Indirect | Direct |
|---|---|---|
| Route | Through deep ring → canal → superficial ring | Through Hesselbach triangle directly |
| Relation to inferior epigastric artery | Lateral | Medial |
| Scrotal descent | Common (inguinoscrotal) | Uncommon |
| Coverings | Internal spermatic fascia + cremasteric + external | External spermatic only |
| Aetiology | Congenital — patent processus vaginalis | Acquired — weak transversalis fascia |
| Common age | Infants, young adults | Older adults (>50 years) |
| Sex | Male >> female | Male > female |
| Laterality | Right > left (late testicular descent) | Often bilateral |
| Strangulation risk | Higher than direct | Lower |
| Shape | Elongated (pear-shaped) | Globular (dome-shaped) |
| Deep ring occlusion test | Controlled by pressure on deep ring | Not controlled |
Deep ring occlusion test (Mackay's test):
- Reduce the hernia
- Press over deep ring (1.5 cm above midpoint of inguinal ligament)
- Ask patient to cough / strain
- Indirect hernia is controlled (does not appear)
- Direct hernia appears medially despite pressure
Pantaloon (saddlebag) hernia — a combined direct + indirect hernia straddling the inferior epigastric artery on both sides.
Incidence:
- Indirect : direct = 2 : 1 overall
- Right side dominant (70%)
- Male : female = 9 : 1
Femoral hernia — highest strangulation risk
Femoral hernia is a protrusion of abdominal contents through the femoral canal, beneath the inguinal ligament — and its rigid boundaries explain its notoriously high strangulation rate.
Femoral canal anatomy:
- Medial compartment of the femoral sheath (the sheath has 3 compartments: lateral — femoral artery; intermediate — femoral vein; medial — femoral canal)
- ~1.5 cm in length
- Contents normally: lymphatic vessels, deep inguinal lymph node (of Cloquet), fat
- Femoral ring (upper opening) is the weak point
Boundaries of femoral ring (the unyielding ring):
| Border | Structure |
|---|---|
| Anterior | Inguinal ligament (Poupart) |
| Posterior | Pectineal ligament of Cooper + superior ramus of pubis |
| Medial | Lacunar ligament of Gimbernat (sharp, crescentic) |
| Lateral | Femoral vein |
Clinical features:
- More common in females (wider pelvis, larger femoral canal) — F:M ~4:1
- Common in middle-aged and elderly
- Small globular swelling below and lateral to pubic tubercle (inguinal hernia lies above and medial to pubic tubercle)
- Often irreducible
- Strangulation rate ~40% — highest of all hernias
- Frequent first presentation: intestinal obstruction or strangulation
Richter hernia in the femoral ring is particularly dangerous — partial bowel wall strangulation without complete obstruction may cause delayed presentation.
Surgical approaches:
- Lockwood (low approach) — below inguinal ligament; simpler; ideal for elective repair of uncomplicated femoral hernia
- Lothiessen (trans-inguinal) — through the inguinal canal; opens transversalis fascia to reach femoral ring
- McEvedy (high preperitoneal) — above inguinal ligament; best for strangulated / complicated / emergency repair (allows bowel resection)
- Mesh repair with preperitoneal approach (TEP / TAPP) is increasingly preferred
Relieving incision in emergency — cutting lacunar ligament medially (with care for aberrant obturator artery, "artery of death") to relieve constriction.
Hernia repair techniques
Open and laparoscopic hernia repairs have evolved from pure tissue reconstruction to tension-free mesh — and the named repairs are NEET PG staples.
Open tissue repairs (historic but still tested):
| Repair | Year | Principle | Recurrence |
|---|---|---|---|
| Bassini | 1887 | Approximation of conjoint tendon to inguinal ligament in 3 layers | 10–15% |
| Shouldice | 1945 | 4-layer imbricated repair of transversalis fascia | 1–2% (best tissue repair) |
| Halsted | 1893 | Similar to Bassini but also transposed cord | Historic |
| McVay (Cooper ligament) | 1942 | Approximation of conjoint tendon to Cooper ligament; good for femoral hernias | 2–5% |
Open tension-free mesh repair:
Lichtenstein repair (1984) — current gold standard for open inguinal hernia repair:
- Open approach via inguinal incision
- Onlay polypropylene mesh covering posterior wall and Hesselbach triangle
- Mesh sutured to pubic tubercle medially, inguinal ligament inferiorly, conjoint tendon superiorly
- Slit in mesh for spermatic cord; reconstructed around cord
- Recurrence < 1%
- Day care procedure under local / regional anaesthesia
Other open mesh techniques:
- Rutkow (plug and patch) — cone of mesh plug in defect + onlay patch
- Gilbert (sutureless, preperitoneal disc + onlay)
- Kugel (preperitoneal patch)
- TIPP (Trans-Inguinal Pre-Peritoneal)
Laparoscopic repairs:
| Feature | TEP (Totally Extraperitoneal) | TAPP (Transabdominal Preperitoneal) |
|---|---|---|
| Access | Preperitoneal space only; does NOT enter peritoneum | Enters peritoneum first, then dissects peritoneum to expose preperitoneal space |
| Pros | Lower visceral injury risk, no peritoneal closure needed | Easier anatomy, diagnostic laparoscopy, better for recurrent / bilateral / femoral |
| Cons | Steeper learning curve, limited space, CO2 subcutaneous emphysema | Peritoneal violation, bowel injury risk, adhesions |
| Mesh | Covers myopectineal orifice; 15 × 10 cm polypropylene | Same mesh; peritoneum sutured/stapled over mesh |
| Recurrence | 1–3% | 1–3% |
| Chronic pain | Lower than Lichtenstein | Lower than Lichtenstein |
| Ideal for | Bilateral, recurrent, athletes | Bilateral, recurrent, femoral, incarcerated |
Key triangles in laparoscopic repair (avoid injury):
| Triangle | Boundaries | Contents (to avoid) |
|---|---|---|
| Triangle of doom | Medial: vas deferens. Lateral: testicular vessels. Apex: deep ring | External iliac artery and vein |
| Triangle of pain | Medial: testicular vessels. Lateral: iliopubic tract | Lateral femoral cutaneous, femoral branch of genitofemoral, femoral nerves |
Mesh should be stapled/tacked ONLY above the iliopubic tract and medial to the vas deferens.
Complications of hernia repair (general):
- Haematoma, seroma
- Wound infection (higher with mesh)
- Chronic groin pain (ilioinguinal, iliohypogastric, genitofemoral neuralgia) — 5–15%
- Ischaemic orchitis → testicular atrophy
- Urinary retention
- Recurrence
- Mesh-related: infection, erosion into bladder / bowel, seroma, rejection
Umbilical, paraumbilical, and incisional hernias
Umbilical and incisional hernias are common ventral hernias with distinct demographics, and their management differs substantially from groin hernias.
Congenital umbilical hernia:
- Protrusion through umbilical ring (failure of closure of umbilical cicatrix)
- Common in neonates and infants; higher in Afro-Caribbean children
- 80–90% close spontaneously by 5 years with fascial defect <1.5 cm
- Strangulation is rare
- Conservative observation until 5 years; surgery if defect >=2 cm, persistent beyond 5 years, or symptomatic
Paraumbilical hernia (adult, acquired):
- Through the linea alba just above or below the umbilical ring (not through the umbilicus itself)
- Common in multiparous, obese, middle-aged women
- Contents: preperitoneal fat, omentum, small bowel
- Often painful, irreducible
- Risk of strangulation (~20%)
- Repair: Mayo operation (overlapping vest-over-pants suture) or mesh repair (preferred now)
Epigastric hernia — through linea alba between xiphoid and umbilicus; usually small, painful, often contains just preperitoneal fat.
Incisional (ventral) hernia:
- Herniation through a previous abdominal surgical scar
- Incidence: 5–20% of laparotomies (higher with midline incisions, emergency surgery, obesity, wound infection)
- Risk factors: obesity, diabetes, malnutrition, chronic cough / constipation (raised IAP), smoking, steroids, wound infection, poor suturing technique, ascites
- Jenkins rule — suture length to wound length ratio of 4:1 reduces incisional hernia
- Small defect (<4 cm): primary suture repair (high recurrence ~50%)
- Large defect: mesh repair (onlay, sublay, intraperitoneal onlay mesh — IPOM) — recurrence <10%
- Component separation technique for large midline defects (Ramirez procedure)
- Laparoscopic IPOM with composite mesh
Sliding, Richter, Amyand, Littre, and obturator hernias
Several hernia eponyms describe specific contents or wall composition — and they are high-value NEET PG MCQ material.
Sliding hernia:
- A viscus forms part of the wall of the hernia sac (not merely a content)
- Most common viscus: sigmoid colon on the left, caecum/appendix on the right, bladder medially
- Retroperitoneal organs (caecum, sigmoid, bladder) slide down with peritoneum
- Risk: organ injury during sac opening
- Recognise: thick-walled sac, mesentery visible on one side
- Repair: reduce contents, plicate bowel, standard hernia repair (do NOT excise sac wall containing bowel)
Richter hernia:
- Only part of the antimesenteric circumference of bowel herniates (not full lumen)
- Bowel lumen not obstructed → no classic colicky pain / vomiting initially
- Strangulation and gangrene without obstruction → delayed diagnosis, high mortality
- Common sites: femoral ring (classic), laparoscopic trocar site (5–12 mm), obturator canal, umbilical
Amyand hernia:
- Hernia sac contains the vermiform appendix (normal, inflamed, or perforated)
- Usually right-sided inguinal hernia
- Named after Claudius Amyand (1735) — first successful appendectomy, through an inguinal hernia of an 11-year-old boy
- Classification (Losanoff & Basson):
- Type 1 — normal appendix
- Type 2 — acute appendicitis within sac
- Type 3 — appendicitis with abdominal sepsis
- Type 4 — concurrent pathology
- Management: appendectomy + hernia repair (mesh avoided if inflamed)
Littre hernia:
- Contains a Meckel diverticulum (ileal remnant of vitellointestinal duct)
- Sites: inguinal, femoral, umbilical
- Rule of 2s — Meckel is 2 feet from ileocaecal valve, 2% population, 2% symptomatic, 2 inches long, 2 types of mucosa (ileal + ectopic gastric/pancreatic), age <2 years symptomatic
Maydl hernia (hernia-en-W):
- Two loops of bowel in the sac, with the middle intervening loop lying in the abdomen and potentially strangulated
- Strangulated portion is in the abdomen, not in the sac
- Easy to miss at surgery — inspect both afferent and efferent limbs
Obturator hernia:
- Through the obturator canal (below obturator membrane)
- Elderly, emaciated women (hence "little old lady's hernia")
- Howship-Romberg sign — pain along medial thigh radiating to knee (compression of obturator nerve), worsened by thigh abduction / extension / internal rotation
- Often presents as bowel obstruction without palpable swelling
- Diagnosis: CT abdomen
- Management: laparoscopic or open repair
Spigelian hernia:
- Through the linea semilunaris (lateral edge of rectus sheath) at the arcuate line
- Below the umbilicus, lateral to rectus
- Small defect but high strangulation risk
Petit (inferior lumbar) and Grynfeltt (superior lumbar) triangle hernias — posterior abdominal wall hernias; rare; diagnosed by CT.
Sources and references
- Bailey & Love's Short Practice of Surgery, 28th Edition (Williams, Bulstrode, O'Connell, Eds., 2023) — Chapter on Hernias.
- Sabiston Textbook of Surgery, 21st Edition (Townsend, Beauchamp, Evers, Mattox, Eds., 2021) — Chapter on Inguinal Hernias.
- Schwartz's Principles of Surgery, 11th Edition (Brunicardi et al., 2019) — Chapter on Inguinal Hernias and Anterior Abdominal Wall Hernias.
- SRB's Manual of Surgery, 6th Edition (Bhat SM, 2019) — Hernia chapter with Indian examination perspective.
- HerniaSurge Group. International guidelines for groin hernia management. Hernia 2018; 22(1):1-165.
- Snell RS. Clinical Anatomy by Regions, 10th Edition (2018) — Chapter on Abdominal Wall and Inguinal Canal.
Frequently asked questions
How many hernia and inguinal anatomy questions appear in NEET PG?
Hernias and inguinal canal anatomy contribute 3-4 direct questions per NEET PG paper across surgery, anatomy, and clinical surgery. Boundaries of the inguinal canal, Hesselbach triangle, direct vs indirect hernia differentiation, femoral hernia strangulation, and mesh repair types (Lichtenstein, TEP, TAPP) are the most tested subtopics based on 2019-2025 pattern analysis.
What are the boundaries of the inguinal canal?
The inguinal canal is a 4 cm oblique passage in the lower anterior abdominal wall. Anterior wall: external oblique aponeurosis throughout, internal oblique in the lateral third. Posterior wall: transversalis fascia throughout, conjoint tendon (internal oblique plus transversus abdominis) in the medial third. Floor: inguinal ligament and lacunar ligament medially. Roof: arching fibres of internal oblique and transversus abdominis (conjoint tendon). Deep ring at midpoint of inguinal ligament, 1 to 1.5 cm above the femoral pulse; superficial ring in external oblique aponeurosis above pubic tubercle.
What are the contents of the inguinal canal?
The inguinal canal contains the spermatic cord in males and the round ligament of the uterus in females, along with the ilioinguinal nerve (runs with the cord but outside the internal spermatic fascia). The spermatic cord contains 3 arteries (testicular, cremasteric, artery to vas), 3 nerves (genital branch of genitofemoral, sympathetic, ilioinguinal which lies outside), 3 fascial layers (external spermatic, cremasteric, internal spermatic), the vas deferens, the pampiniform plexus, lymphatics, and the obliterated processus vaginalis.
What is the Hesselbach triangle?
Hesselbach triangle (inguinal triangle) is the anatomical area on the posterior inguinal wall where direct inguinal hernias protrude. Boundaries: medially the lateral border of rectus abdominis (linea semilunaris), laterally the inferior epigastric artery, and inferiorly the inguinal ligament. Direct hernias push through the transversalis fascia within this triangle, medial to the inferior epigastric vessels. Indirect hernias enter through the deep ring lateral to the inferior epigastric vessels.
How do direct and indirect inguinal hernias differ?
Indirect hernia passes through the deep ring lateral to the inferior epigastric vessels, traverses the full inguinal canal, and can descend into the scrotum — it is congenital (patent processus vaginalis), more common in males, and common in young patients; covered by internal spermatic fascia. Direct hernia pushes medially through Hesselbach triangle medial to the inferior epigastric vessels, usually does not enter scrotum, is acquired from weak transversalis fascia, and common in older males. The deep ring occlusion test differentiates: pressure over the deep ring controls indirect but not direct hernia.
Why does femoral hernia have the highest risk of strangulation?
Femoral hernia passes through the femoral canal, which is the narrowest medial compartment of the femoral sheath and is bounded by rigid structures — the inguinal ligament anteriorly, the pectineal (Cooper) ligament posteriorly, the lacunar (Gimbernat) ligament medially, and the femoral vein laterally. These unyielding boundaries compress the hernia sac quickly, cutting off venous drainage and arterial supply. Strangulation rate is approximately 40 percent (highest of all hernias). More common in females (wider pelvis, larger femoral canal), especially middle-aged and elderly women.
What is the difference between Lichtenstein, Shouldice, and Bassini repairs?
Bassini repair (1887) is the original open tissue repair — approximates conjoint tendon to inguinal ligament in three layers; high recurrence (10-15 percent). Shouldice repair (1945) is a four-layer imbricated open tissue repair of the transversalis fascia; lowest recurrence (1-2 percent) among pure tissue repairs but technically demanding. Lichtenstein repair (1984) is a tension-free open mesh repair — polypropylene mesh onlay over posterior wall and around the cord; current gold standard for open repair with recurrence less than 1 percent.
What is TEP vs TAPP repair?
TEP (Totally Extraperitoneal) and TAPP (Transabdominal Preperitoneal) are the two laparoscopic hernia repair techniques. TEP accesses the preperitoneal space without entering the peritoneal cavity — lower visceral injury risk but steeper learning curve and limited space. TAPP enters the peritoneal cavity, dissects peritoneum to expose hernia defect, places mesh preperitoneally, then closes peritoneum — easier diagnostic, useful for bilateral and femoral hernias, but higher risk of bowel injury and adhesions. Both have similar recurrence (1-3 percent) and reduced chronic pain vs Lichtenstein.
What is a Richter hernia?
Richter hernia is an atypical hernia where only part of the antimesenteric circumference of the bowel wall herniates through the defect, WITHOUT producing complete obstruction. The patient may have strangulation and gangrene of the protruding bowel segment without classic intestinal obstruction features (absent colicky pain, absent vomiting initially). Common sites: femoral ring, laparoscopic trocar sites (5-12 mm), obturator canal. High delay-to-diagnosis risk and high mortality if missed.
What are Amyand and Littre hernias?
Amyand hernia is a hernia (usually right inguinal) containing the vermiform appendix, which may be normal, inflamed, or perforated. Named after Claudius Amyand who performed the first successful appendectomy through an inguinal hernia in 1735. Littre hernia is a hernia containing a Meckel diverticulum (ileal remnant of the vitellointestinal duct), most commonly found in inguinal, femoral, or umbilical sites. Both are diagnosed intraoperatively and managed by excision of the abnormal content plus standard hernia repair.
Ready to convert this guide into exam marks? Revise with the surgery high-yield topics overview, avoid classic distractor traps with the common mistakes in surgery guide, and use the AI tutor to drill the inferior-epigastric relationship on demand.
Start practicing surgery MCQs free →
Explore our pricing plans for unlimited practice across all 19 subjects, AI-powered doubt resolution, and personalized study plans.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Written by: NEETPGAI Editorial Team Reviewed by: Pending SME Review Last reviewed: April 2026
This article is reviewed by qualified medical professionals for clinical accuracy and exam relevance. For corrections or updates, contact the editorial team.
This content is for educational purposes for NEET PG exam preparation. It is not a substitute for professional medical advice, diagnosis, or treatment. Clinical information has been reviewed by qualified medical professionals.
Ready to put this into practice?
Start practicing NEET PG MCQs with AI-powered explanations.
Start Free PracticeYour Next Step
Related Study Guides
How to Revise Mistakes With AI Flashcards for NEET PG — A 10-Step Personal Mistake-Bank Protocol
Build a personal NEET PG mistake-bank with AI flashcards: error taxonomy, mock-test extraction, Anki vs RemNote vs NEETPGAI, spaced repetition cadence, leech card management, last-week protocol.
Clinical Case: 65-Year-Old Obese Woman With RUQ Pain and Fever — Acute Cholecystitis for NEET PG
NEET PG clinical case on acute cholecystitis: 65-yo obese female, RUQ pain after fatty meal, Murphy's sign, TG18 criteria, severity grading, early laparoscopic cholecystectomy, complications.
Thoracic Mediastinum Anatomy for NEET PG 2026
Master mediastinal compartments, the 4 T's of anterior masses, hilar relations, IASLC nodal stations and thoracic outlet anatomy for NEET PG 2026.
Join our NEET PG community
Daily MCQs, study tips, and topper strategies on Telegram.
Join on Telegram →