## Management of Oesophageal Varices: Secondary Prophylaxis **Key Point:** After successful acute variceal haemorrhage control, secondary prophylaxis with non-selective beta-blockers is the first-line pharmacological intervention to prevent rebleeding. ### Rationale for Propranolol Propranolol reduces portal pressure by: 1. Decreasing cardiac output (β1-blockade) 2. Reducing splanchnic blood flow (β2-blockade of splanchnic vasodilators) 3. Achieving a target reduction of 25% in heart rate or a resting heart rate of 55–60 bpm **High-Yield:** Non-selective beta-blockers (propranolol, nadolol, carvedilol) reduce the risk of rebleeding by ~40% and mortality by ~10% in cirrhotic patients with varices [cite:Harrison 21e Ch 297]. ### When TIPS is Considered TIPS is reserved for: - Acute variceal rebleeding *despite* optimal medical therapy and endoscopic treatment - Refractory ascites - Hepatic encephalopathy (relative contraindication) - Not as first-line secondary prophylaxis **Clinical Pearl:** TIPS carries a 10–15% risk of hepatic encephalopathy and should not be deployed prematurely; it is a bridge to transplantation or a rescue intervention. ### Why Repeat Ligation Alone Is Insufficient Endoscopic variceal ligation (EVL) controls acute bleeding but does not prevent rebleeding without pharmacological support. The combination of EVL + beta-blockers is superior to either alone. ### Splenectomy Splenectomy is not standard therapy for portal hypertension in cirrhosis—it does not reliably reduce portal pressure and carries surgical morbidity in a decompensated patient. 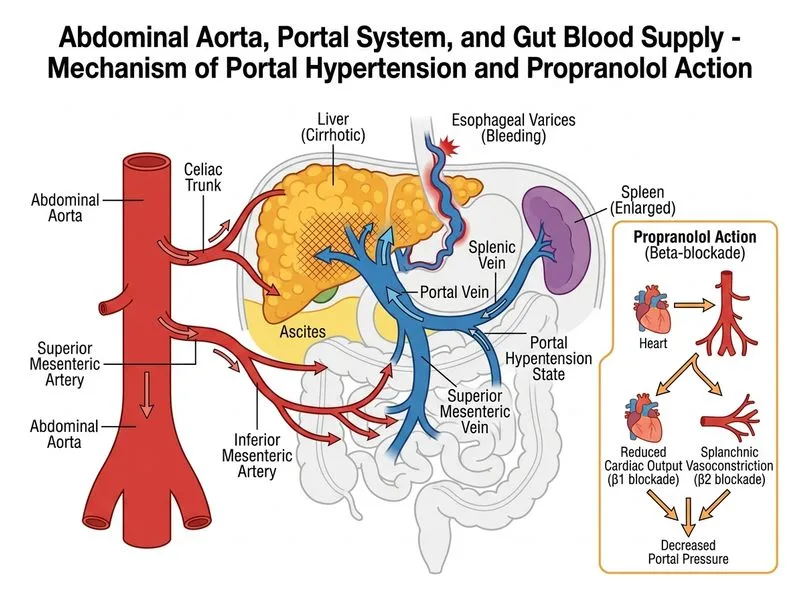
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.