## Distinguishing Autoimmune from TB-Induced Addison Disease ### Epidemiology and Pathogenesis **Key Point:** In developed countries, autoimmune destruction accounts for ~80% of primary adrenal insufficiency (Addison disease). In developing countries like India, tuberculosis remains a leading cause. Both present with identical clinical and biochemical findings, but their etiology differs fundamentally. ### Comparative Diagnostic Features | Feature | Autoimmune Addison | TB-Induced Addison | |---------|-------------------|-------------------| | **Anti-21-hydroxylase antibodies** | ✓ Present (90% of cases) | ✗ Absent | | **Anti-17α-hydroxylase antibodies** | ✓ Present (50% of cases) | ✗ Absent | | **Adrenal calcification** | ✗ Rare | ✓ Common (50–80% of cases) | | **Chest X-ray findings** | Normal | May show TB lesions | | **Adrenal imaging** | Normal size or atrophic | Enlarged, nodular | | **ESR/CRP** | Normal or mildly elevated | Often elevated | | **Associated autoimmune diseases** | ✓ Common (thyroiditis, vitiligo, pernicious anemia) | ✗ Rare | ### Why Anti-21-Hydroxylase Antibodies are the Best Answer **High-Yield:** Anti-21-hydroxylase (anti-21-OH) antibodies are: - Present in **~90% of autoimmune Addison disease** - **Virtually absent** in TB-induced adrenal insufficiency - Highly specific for autoimmune etiology - Diagnostic of the underlying mechanism (autoimmune destruction of steroid-producing enzymes) **Clinical Pearl:** Detection of anti-21-hydroxylase antibodies confirms autoimmune Addison disease and allows: - Screening for associated autoimmune conditions (thyroiditis, type 1 diabetes, pernicious anemia) - Genetic counseling (increased familial risk) - Exclusion of TB as the etiology ### Why Other Options Are Inferior **Adrenal calcification (Option 2):** While highly suggestive of TB-induced Addison, calcification is: - NOT present in all TB cases (~50–80% sensitivity) - NOT specific for TB (can rarely occur in other granulomatous diseases) - Does NOT confirm autoimmune disease; its absence does not exclude TB - A finding that suggests TB, not one that confirms autoimmune disease **Chest X-ray findings (Option 1):** Apical infiltrates suggest TB but: - Are not always present in TB-induced adrenal insufficiency - Do NOT confirm the adrenal disease is autoimmune - Are nonspecific (can occur in other lung conditions) **Elevated inflammatory markers (Option 3):** ESR and CRP: - Are nonspecific and can be elevated in both TB and autoimmune disease - Do NOT discriminate between the two etiologies - Are not diagnostic of autoimmune Addison disease ### Diagnostic Algorithm ```mermaid flowchart TD A[Primary Adrenal Insufficiency Confirmed]:::outcome --> B{Check anti-21-OH antibodies}:::decision B -->|Positive| C[Autoimmune Addison Disease]:::outcome B -->|Negative| D{Imaging findings?}:::decision D -->|Adrenal calcification| E[TB-Induced Addison]:::outcome D -->|Enlarged adrenals| F[Consider TB, fungal, or malignancy]:::outcome D -->|Normal imaging| G[Obtain TB culture/PCR]:::action C --> H[Screen for associated autoimmune conditions]:::action E --> I[Start anti-TB therapy + steroid replacement]:::action ``` **Mnemonic:** **AAA** — **Antibodies Against Adrenal** enzymes (21-OH, 17α-OH) are pathognomonic for **Autoimmune Addison**. 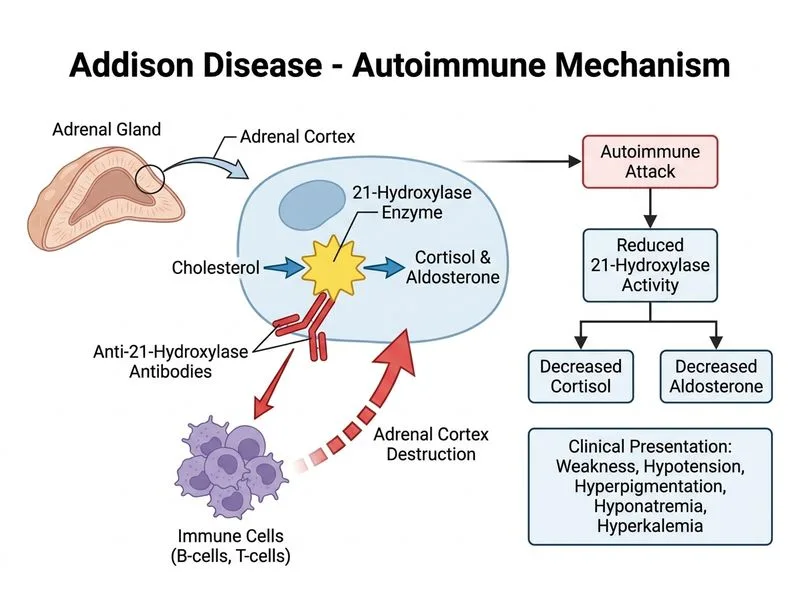
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.