## Clinical Diagnosis This patient has **iron deficiency anemia (IDA)** confirmed by: - Microcytic hypochromic indices (MCV 62, MCH 18) - Low serum iron, low ferritin, elevated TIBC (classic iron-deficient pattern) - Glossitis and splenomegaly (systemic features) ## Why GI Endoscopy is the Next Step **Key Point:** In any adult with iron deficiency anemia, the underlying cause must be identified before empiric iron replacement. In women of reproductive age, menorrhagia is the most common cause; however, GI blood loss (peptic ulcer, gastritis, celiac disease, colorectal polyps/malignancy) must be excluded. **High-Yield:** The presence of glossitis (not seen in simple dietary iron deficiency) and the severity of anemia (Hb 7.2) suggest chronic blood loss rather than dietary insufficiency alone. This patient requires endoscopic evaluation. **Clinical Pearl:** While iron supplementation will eventually correct the anemia, starting iron without investigating the source risks masking a serious underlying pathology (e.g., gastric ulcer, colorectal cancer) and delaying definitive treatment. ## Management Algorithm ```mermaid flowchart TD A[Iron Deficiency Anemia confirmed]:::outcome --> B{Patient age & sex?}:::decision B -->|Premenopausal woman| C[Assess menstrual history]:::action B -->|Postmenopausal woman or any man| D[GI source likely]:::outcome C -->|Heavy menstrual bleeding only| E[Start iron + gynecology referral]:::action C -->|Symptoms suggest GI loss| D D --> F[Upper + Lower GI endoscopy]:::action F --> G{Source identified?}:::decision G -->|Yes| H[Treat underlying cause + iron]:::action G -->|No| I[Consider celiac serology, H. pylori]:::action ``` **Tip:** In NEET PG, always ask: "Why is the patient anemic?" before "How do I treat it?" This question tests that principle. [cite:Harrison 21e Ch 96] 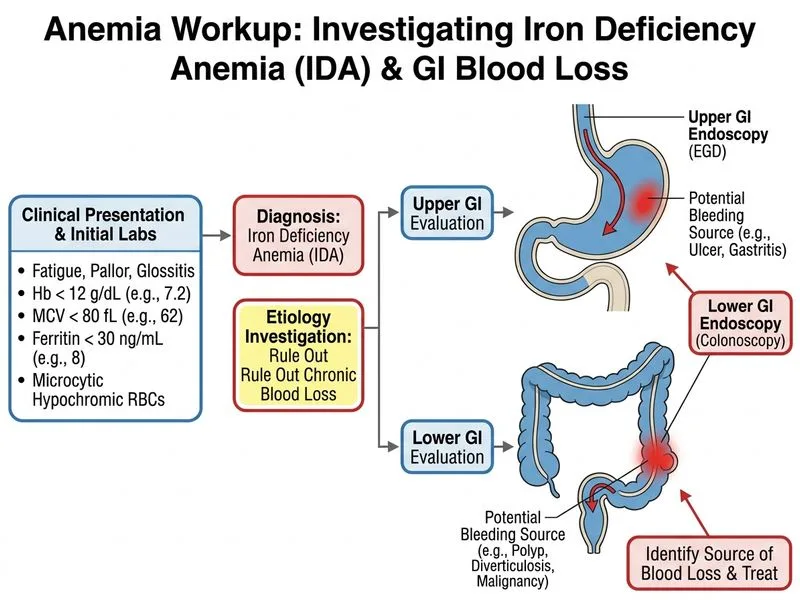
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.