## Diagnosis: Iron Deficiency Anemia (IDA) ### Clinical and Laboratory Correlation **Key Point:** The constellation of microcytic hypochromic anemia (MCV 62 fL, MCH 18 pg), elevated TIBC, low serum iron, and low ferritin (8 ng/mL) is pathognomonic for iron deficiency anemia. **High-Yield:** The peripheral blood smear showing microcytic hypochromic RBCs with target cells confirms chronic iron deficiency. The RBC count is paradoxically elevated (5.8 × 10¹²/L) because the body produces more RBCs to compensate for reduced hemoglobin per cell. ### Iron Metabolism Parameters | Parameter | Normal Range | This Patient | Interpretation | |-----------|--------------|--------------|----------------| | Serum Iron | 60–170 µg/dL | 32 µg/dL | Depleted | | TIBC | 250–425 µg/dL | 420 µg/dL | Elevated (iron-binding capacity increased) | | Ferritin | 15–200 ng/mL | 8 ng/mL | Severely depleted iron stores | | Transferrin Saturation | 20–50% | ~7.6% | Severely reduced | **Clinical Pearl:** Ferritin <15 ng/mL is virtually diagnostic of absent iron stores. Combined with the clinical history of menorrhagia (the most common cause of IDA in women of reproductive age in India), this is uncomplicated iron deficiency anemia. ### Management Algorithm ```mermaid flowchart TD A[Iron Deficiency Anemia confirmed]:::outcome --> B{Hb < 7 g/dL or symptomatic?}:::decision B -->|No| C[Oral iron therapy]:::action B -->|Yes| D[Consider transfusion + IV iron]:::action C --> E[Ferrous sulfate 200 mg daily]:::action E --> F[Reassess Hb after 4 weeks]:::action F --> G{Hb rise ≥ 1-2 g/dL?}:::decision G -->|Yes| H[Continue therapy for 3-6 months]:::action G -->|No| I[Investigate for malabsorption or ongoing loss]:::action B -->|Hb < 5 or hemodynamic compromise| J[Transfuse PRBCs + IV iron]:::urgent ``` ### Why Oral Iron is First-Line Here 1. **Hb 7.2 g/dL is adequate** for oral therapy initiation (not <7 g/dL). 2. **No acute symptoms** of cardiac compromise or severe dyspnea at rest. 3. **Oral iron is preferred** because: - Better long-term compliance and safety profile - Ferrous sulfate 200 mg daily provides ~60 mg elemental iron - Expected Hb rise: 1–2 g/dL per week in uncomplicated IDA - Cost-effective and suitable for outpatient management 4. **Reassessment at 4 weeks** is standard to confirm response and guide further therapy. **Mnemonic: ORAL FIRST — O (Oral iron preferred), R (Response expected in 4 weeks), A (Adequate Hb for oral route), L (Long-term therapy needed), F (Ferrous sulfate 200 mg).** ### Why Endoscopy is NOT the Next Step **High-Yield:** In a premenopausal woman with heavy menstrual bleeding, the source of iron loss is already identified. Endoscopy is indicated only if: - The patient is postmenopausal or male (occult GI bleeding suspected). - Oral iron fails (no Hb rise after 4 weeks despite compliance). - There are GI symptoms (melena, hematemesis). This patient does not meet these criteria yet. 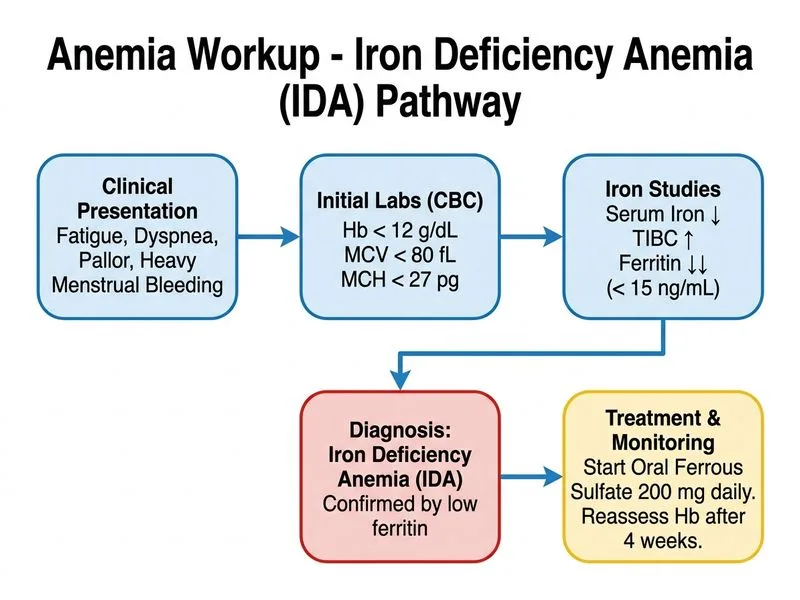
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.