## Diagnosis: Anemia of Chronic Kidney Disease (ACD) — Erythropoietin Deficiency ### Clinical and Laboratory Synthesis **Key Point:** The combination of normocytic normochromic anemia, low reticulocyte count (0.8%), normal iron metabolism, and Stage 3b CKD (eGFR 38) is diagnostic of anemia of chronic kidney disease due to erythropoietin (EPO) deficiency. ### Differential Diagnosis: Iron Deficiency vs. EPO Deficiency in CKD | Feature | Iron Deficiency | EPO Deficiency (ACD) | This Patient | |---------|-----------------|----------------------|---------------| | MCV | Low (microcytic) | Normal | 84 fL (normal) | | MCH | Low | Normal | 28 pg (normal) | | Serum Iron | Low (<60 µg/dL) | Normal | 95 µg/dL (normal) | | Ferritin | Low (<15 ng/mL) | Normal/High | 180 ng/mL (normal) | | TIBC | High (>425 µg/dL) | Normal | 280 µg/dL (normal) | | Reticulocyte Count | High (compensatory) | Low (inadequate response) | 0.8% (LOW) | | RBC Count | High (microcytic index) | Low/Normal | 3.2 × 10¹²/L (low) | **High-Yield:** The **inappropriately low reticulocyte count (0.8%) in the presence of anemia** is the hallmark of EPO deficiency. In iron deficiency, the reticulocyte count would be elevated (>2–3%) as the bone marrow attempts to compensate. **Clinical Pearl:** A reticulocyte count <1.5% in an anemic patient with CKD indicates impaired erythropoiesis and EPO deficiency, not iron deficiency. ### Pathophysiology of Anemia in CKD ```mermaid flowchart TD A[Chronic Kidney Disease]:::outcome --> B[Loss of renal mass and function]:::outcome B --> C[Decreased EPO production by peritubular fibroblasts]:::outcome C --> D[Reduced erythropoiesis in bone marrow]:::outcome D --> E[Normocytic normochromic anemia]:::outcome E --> F{Reticulocyte response adequate?}:::decision F -->|Yes| G[Mild anemia, good compensation]:::outcome F -->|No| H[Moderate-severe anemia, EPO deficiency]:::urgent B --> I[Uremia: shortened RBC survival]:::outcome B --> J[Chronic inflammation: hepcidin ↑]:::outcome J --> K[Functional iron deficiency]:::outcome ``` ### Why This Patient Has Pure EPO Deficiency (Not Iron Deficiency) 1. **Iron studies are completely normal:** - Serum iron 95 µg/dL (normal range) - Ferritin 180 ng/mL (normal; >15 ng/mL rules out iron deficiency) - TIBC 280 µg/dL (normal; would be elevated in iron deficiency) - Transferrin saturation ~34% (adequate iron availability) 2. **RBC indices are normocytic normochromic:** - MCV 84 fL (normal; would be <80 in iron deficiency) - MCH 28 pg (normal; would be <27 in iron deficiency) 3. **Reticulocyte count is inappropriately low:** - 0.8% is at the lower end of normal; in an anemic patient, it should be >2–3% if bone marrow were responding appropriately. - This indicates **inadequate erythropoietic response**, which is the hallmark of EPO deficiency. 4. **CKD Stage 3b (eGFR 38):** - EPO production declines significantly when eGFR falls below 45 mL/min/1.73 m². - This patient is at the threshold where EPO deficiency becomes clinically significant. **Mnemonic: NREP — N (Normocytic), R (Reticulocyte count low), E (EPO deficiency), P (Pure ACD in this case).** ### Why Not Iron Deficiency? ~~Iron deficiency~~ would present with: - Microcytic indices (MCV <80, MCH <27) - Low ferritin (<15 ng/mL) - Elevated TIBC (>425 µg/dL) - **Elevated reticulocyte count** (compensatory response) This patient has none of these features. ### Why Not Hemolytic Anemia? **High-Yield:** Hemolytic anemia would show: - **Elevated reticulocyte count** (>5–10%) - Elevated indirect bilirubin - Elevated LDH - Low haptoglobin - Schistocytes or spherocytes on blood smear This patient's reticulocyte count is LOW, and there are no schistocytes. Hemolysis is ruled out. ### Management Implications **Key Point:** This patient requires **erythropoiesis-stimulating agents (ESAs)**, not iron supplementation. - ESAs (epoetin alfa, darbepoetin alfa) are indicated when Hb <10 g/dL in CKD. - Target Hb: 10–11.5 g/dL (avoid over-correction due to cardiovascular risk). - Iron supplementation is adjunctive only if iron stores are depleted (ferritin <100 ng/mL or TSAT <20%). In this case, iron stores are adequate, so iron therapy is not the primary intervention. 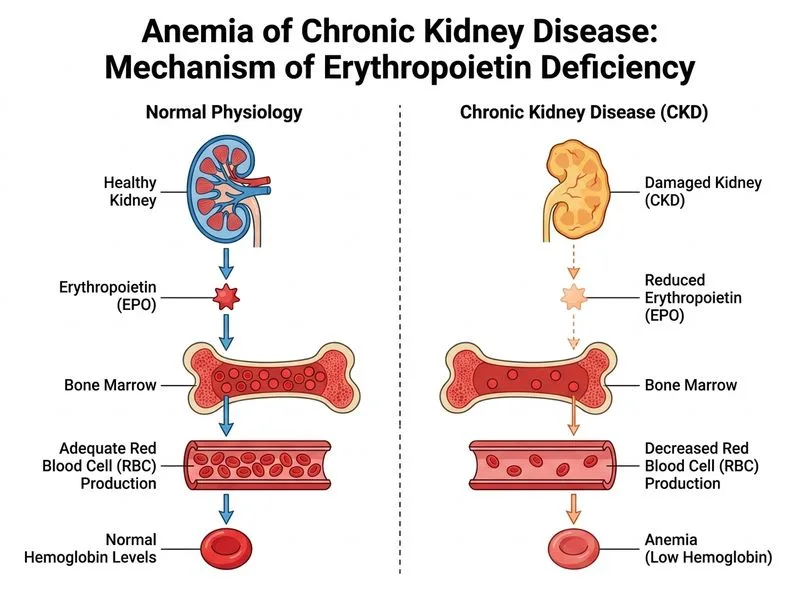
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.