## Clinical Diagnosis: Anemia of Chronic Disease (ACD) ### Understanding Anemia of Chronic Disease **Key Point:** Anemia of chronic disease is the second most common anemia globally and occurs in any chronic inflammatory, infectious, or malignant condition. It is characterized by **impaired erythropoietin response** and **iron sequestration** due to hepcidin dysregulation, NOT iron deficiency. ### Why This Patient Has ACD, Not Iron Deficiency **High-Yield:** The key discriminator is the **iron studies pattern**: | Parameter | Patient | Iron Deficiency | ACD | Chronic Kidney Disease | |-----------|---------|-----------------|-----|------------------------| | Hemoglobin | 9.8 g/dL | ↓ | ↓ | ↓ | | MCV | 78 fL | ↓↓ | Normal/↓ | Normal/↓ | | Serum Iron | 42 µg/dL | **↓↓** | **↓** | **↓** | | Ferritin | 156 ng/mL | **↓↓** | **↑ (normal/↑)** | **↑** | | TIBC | 280 µg/dL | **↑↑** | **↓** | **↓** | | Transferrin Sat. | 15% | **↓↓** | **↓** | **↓** | | EPO Level | — | Normal/↑ | **↓ (blunted)** | **↑↑** | **Clinical Pearl:** In this patient, **ferritin is elevated at 156 ng/mL despite low serum iron**. This paradox is diagnostic of ACD — iron is sequestered in macrophages (ferritin) but unavailable for erythropoiesis (low serum iron, low TIBC). ### Pathophysiology of ACD in Rheumatoid Arthritis ```mermaid flowchart TD A[Chronic Inflammation: RA]:::outcome --> B[IL-6 & TNF-α production]:::outcome B --> C[Hepcidin upregulation]:::outcome C --> D[Ferroportin degradation]:::outcome D --> E[Iron sequestration in macrophages]:::outcome E --> F[Low serum iron available]:::outcome B --> G[Blunted EPO response]:::outcome G --> H[Reduced RBC production]:::outcome F --> H H --> I[Mild-to-moderate anemia<br/>MCV normal or low]:::outcome ``` ### Why the MCV is Low (78 fL) **Key Point:** ACD can present as **normocytic or microcytic**. When microcytic, it is called "ACD with iron-restricted erythropoiesis." The low MCV here reflects: 1. Chronic inflammation → reduced iron availability → smaller RBCs 2. Blunted EPO response → fewer RBCs produced, but those made are smaller 3. **NOT true iron deficiency** — ferritin is elevated ### Clinical Context Supports ACD - **10-year RA** = established chronic inflammatory disease - **Elevated inflammatory markers** (CRP 8.2, ESR 62) = active inflammation - **Hepatosplenomegaly** = extramedullary hematopoiesis + chronic inflammation - **Normal WBC & platelets** = no bone marrow failure (rules out MDS, aplasia) - **Normal renal function** (Cr 1.1) = rules out CKD as primary cause ### Peripheral Blood Smear Findings **Clinical Pearl:** The smear shows **normocytic RBCs with mild anisopoikilocytosis** — consistent with ACD. There are NO target cells, pencil cells, or severe hypochromia as would be seen in iron deficiency. ### Why This Is NOT the Other Diagnoses **Mnemonic: FARM** - **F**erritin elevated → rules out iron deficiency - **A**ctive inflammation (CRP, ESR) → supports ACD - **R**A diagnosis → chronic inflammatory state - **M**ethotrexate toxicity → would cause macrocytic, not microcytic, anemia ### Management of ACD ```mermaid flowchart TD A[ACD Diagnosed]:::outcome --> B[Optimize Disease Control]:::action B --> C[Escalate RA therapy if needed]:::action A --> D[Iron supplementation?]:::decision D -->|Only if proven iron deficiency| E[Check ferritin & iron studies]:::action D -->|Ferritin elevated| F[Avoid iron supplementation]:::action A --> G[Consider ESA if Hb < 8 g/dL]:::action G --> H[Requires EPO level check first]:::action ``` **Key Point:** Iron supplementation is **NOT indicated** in ACD with elevated ferritin — it will worsen iron overload. The anemia will improve with better control of the underlying RA. 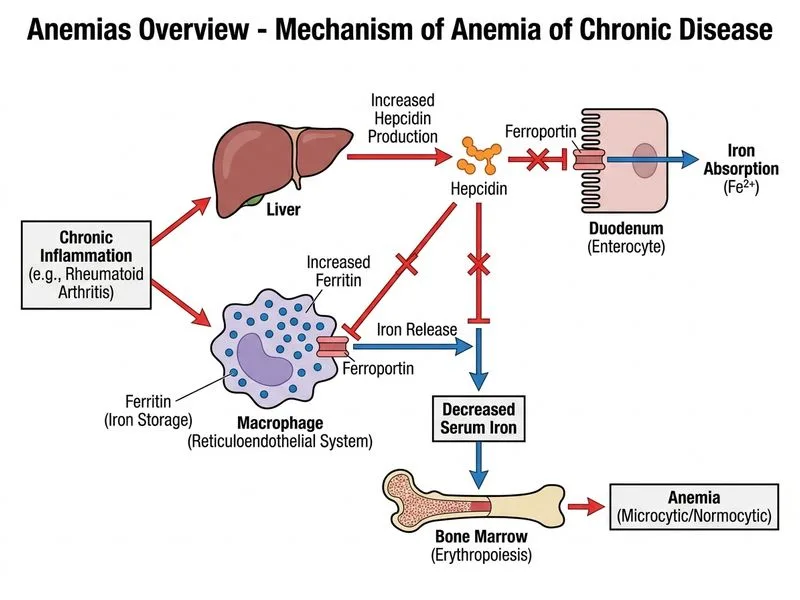
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.