## Classification and Management Rationale This patient meets criteria for **mild persistent asthma** based on symptom frequency (2–3 times per week) and nocturnal symptoms (once monthly), despite normal lung function. ### GINA Step Therapy for Asthma Control **Key Point:** GINA 2023 recommends that all patients with persistent asthma (symptoms ≥2 days per week or any nocturnal symptoms) require regular controller therapy, not reliever-only treatment. **High-Yield:** For mild persistent asthma, the preferred initial controller is **low-dose inhaled corticosteroid (ICS) monotherapy**. This is the most effective and safest first-line agent for step-up from intermittent reliever use. ### Why Low-Dose ICS? | Feature | Low-Dose ICS | LABA Monotherapy | ICS + LABA | |---------|--------------|------------------|------------| | First-line for mild persistent | ✓ Yes | ✗ No (contraindicated) | ✗ No (overkill) | | Anti-inflammatory efficacy | ✓ Excellent | ✗ None | ✓ Excellent | | Systemic side effects at low dose | ✓ Minimal | — | ✓ Minimal | | Risk of asthma mortality if used alone | — | ✗ Increased | — | **Clinical Pearl:** LABA monotherapy is **contraindicated** in asthma management due to increased risk of asthma-related mortality when used without concurrent ICS. LABAs mask inflammation and should never be prescribed as monotherapy. **Warning:** Do not defer controller therapy in persistent asthma. Continuing salbutamol alone exposes the patient to ongoing airway inflammation and risk of exacerbation. ### Recommended Dosing For mild persistent asthma, typical starting doses include: - Fluticasone propionate 100–250 μg twice daily, or - Budesonide 200–400 μg twice daily Reassess control after 2–4 weeks and step up if needed. 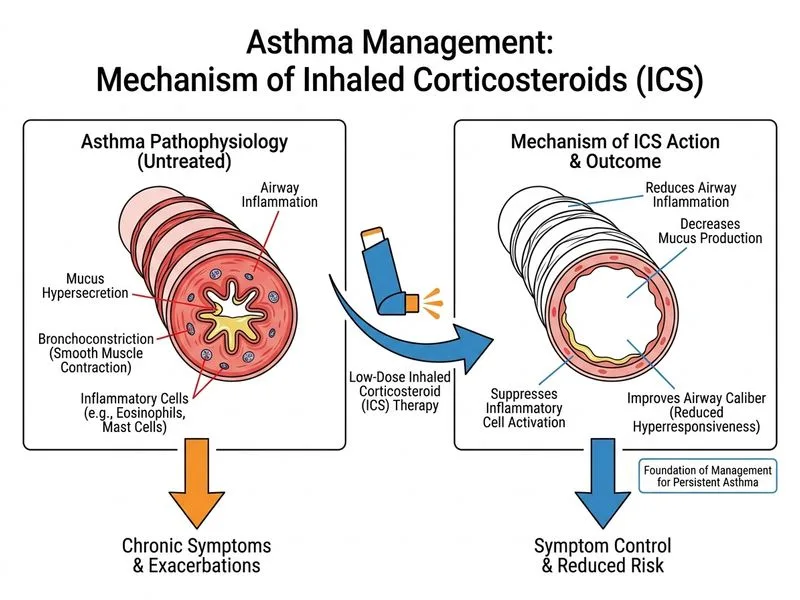
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.