## Clinical Context: Huntington Disease Diagnosis and Initial Management The patient presents with the classic triad of Huntington disease: chorea, cognitive decline, and psychiatric symptoms. Genetic confirmation (CAG repeat expansion in HTT gene) establishes the diagnosis definitively. ## Basal Ganglia Circuit Pathophysiology in Huntington Disease **Key Point:** Huntington disease involves selective degeneration of medium spiny neurons in the striatum, particularly those of the indirect pathway (which express enkephalin and GABA). This leads to: 1. **Loss of indirect pathway inhibition** → reduced thalamic inhibition → excessive thalamic output 2. **Relative dopaminergic excess** in the remaining direct pathway neurons 3. **Net result:** Hyperkinetic movement disorder (chorea) — the opposite of Parkinson disease **Mnemonic: "HD = Hyperkinetic, PD = Hypokinetic"** — Huntington disease causes excessive movement (chorea); Parkinson disease causes movement poverty (bradykinesia). ## Management Algorithm for Newly Diagnosed Huntington Disease ```mermaid flowchart TD A[Confirmed Huntington Disease]:::outcome --> B{Symptomatic chorea present?}:::decision B -->|Yes, functionally impairing| C[Initiate tetrabenazine or deutetrabenazine]:::action B -->|Mild or non-impairing| D[Observe, counsel, arrange follow-up]:::action C --> E[Suppress chorea via VMAT2 inhibition]:::outcome E --> F[Improves function and quality of life]:::outcome G[Genetic counselling for family]:::action H[Psychiatric & cognitive support]:::action I[Multidisciplinary team involvement]:::action C --> G C --> H C --> I ``` ## First-Line Pharmacotherapy: Tetrabenazine **High-Yield:** Tetrabenazine is the gold-standard first-line agent for chorea in Huntington disease because: 1. **Mechanism:** Inhibits vesicular monoamine transporter 2 (VMAT2), depleting presynaptic dopamine and serotonin stores 2. **Effect:** Reduces dopaminergic transmission in the basal ganglia, counteracting the relative dopaminergic excess 3. **Evidence:** FDA-approved for HD chorea; improves functional outcomes 4. **Alternative:** Deutetrabenazine (longer half-life, once-daily dosing) **Clinical Pearl:** Unlike Parkinson disease (where dopamine replacement is needed), Huntington disease requires dopamine reduction. This reflects the opposite pathophysiology of the basal ganglia circuit. ## Comprehensive Management Beyond Pharmacotherapy | Domain | Action | |--------|--------| | **Genetic counselling** | Inform family members of 50% inheritance risk; offer presymptomatic testing | | **Psychiatric support** | Address depression, anxiety, behavioral changes common in HD | | **Cognitive rehabilitation** | Speech therapy, occupational therapy, neuropsychology | | **Multidisciplinary care** | Neurology, psychiatry, genetics, social work, palliative care (later stages) | ## Why Not the Other Options? **Option 1 (Levodopa):** Contraindicated in Huntington disease. Levodopa would increase dopaminergic transmission, worsening chorea. It is used in Parkinson disease (dopamine deficiency), not Huntington disease (relative dopamine excess). **Option 2 (Cardiac MRI):** Cardiac involvement is not a primary feature of Huntington disease. While some studies suggest subtle cardiac autonomic dysfunction, cardiac screening is not part of standard HD management and would delay symptomatic treatment. **Option 3 (Palliative care/hospice):** Premature at this stage. The patient is newly diagnosed with manageable symptoms. Palliative care becomes relevant in advanced disease with severe disability, typically in later stages (10–20 years into illness). **Warning:** Do not confuse Huntington disease management with Parkinson disease. The basal ganglia circuits are disrupted in opposite ways — dopamine depletion in PD (treat with dopamine agonists/levodopa) versus dopamine excess in HD (treat with dopamine antagonists/VMAT2 inhibitors). 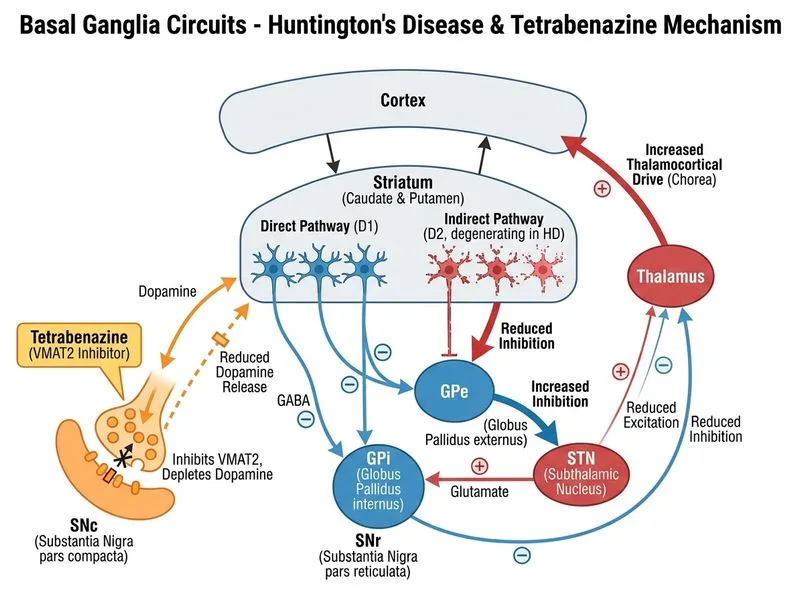
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.