## Diagnosis: Secondary Osteosarcoma (Radiation-Induced) ### Clinical Context: Radiation-Induced Malignancy **High-Yield:** Patients with a history of childhood malignancy treated with radiation therapy have a significantly increased risk of developing secondary osteosarcoma, typically 10–30 years after radiation exposure but can occur earlier in aggressive cases. ### Risk Factors for Secondary Osteosarcoma | Risk Factor | Details | Relevance to This Case | |-------------|---------|------------------------| | **Prior radiation** | External beam therapy to bone | Patient received radiation for retinoblastoma at age 3 | | **Latency period** | 5–30 years post-radiation | 11 years since treatment (within typical range) | | **High-dose chemotherapy** | Doxorubicin, cisplatin increase risk | Patient received chemotherapy | | **Young age at treatment** | Rapidly dividing cells more susceptible | Age 3 at initial treatment | | **Location in radiation field** | Proximal tibia in radiation port | Tumor arises in previously irradiated bone | ### Pathological Features of This Case **Key Point:** Secondary osteosarcomas arising in irradiated bone have the same histological features as primary osteosarcomas but occur in a different age group and clinical context. ### Radiographic & Laboratory Findings 1. **Mixed lytic/sclerotic lesion** — indicates both bone destruction and new bone formation 2. **Cortical breakthrough with soft tissue extension** — aggressive, malignant behavior 3. **Elevated alkaline phosphatase (320 U/L)** — reflects osteoblastic activity 4. **Elevated LDH (580 U/L)** — marker of tumor burden and cell turnover; prognostically significant 5. **MRI findings** — intramedullary location with marrow and soft tissue involvement; essential for surgical planning **Clinical Pearl:** In secondary osteosarcomas, LDH elevation is particularly important as it correlates with prognosis and is used to monitor treatment response alongside alkaline phosphatase. ### Distinguishing Secondary from Primary Osteosarcoma **Mnemonic: SECONDARY OS** - **S**ite: often in radiation field - **E**lder age: typically 20s–40s (vs. primary in adolescents) - **C**hemotherapy history: prior treatment - **O**lder skeletal maturity: may be skeletally mature - **N**eoplasia history: prior malignancy - **D**ifferent prognosis: generally worse than primary OS - **A**ggressive: rapid growth - **R**adiation-related: documented exposure - **Y**ears post-treatment: 5–30 year latency ### Diagnostic Confirmation 1. **Biopsy** — histological confirmation (core needle or open) 2. **CT chest/abdomen** — staging for metastases (lung most common) 3. **Alkaline phosphatase & LDH** — baseline prognostic markers 4. **PET-CT** — may assess metabolic activity and detect occult metastases ### Treatment & Prognosis **Warning:** Secondary osteosarcomas generally have a worse prognosis than primary osteosarcomas due to: - Often larger at diagnosis - More aggressive behavior - Potential chemotherapy resistance (prior exposure) - Higher metastatic potential Management still involves neoadjuvant chemotherapy, wide surgical resection, and adjuvant chemotherapy, but 5-year survival is lower (~40–50%) compared to primary OS (~70%). **Clinical Pearl:** The presence of both elevated alkaline phosphatase AND elevated LDH in the setting of prior radiation therapy is a red flag for secondary malignancy, particularly osteosarcoma. [cite:Robbins 10e Ch 26] 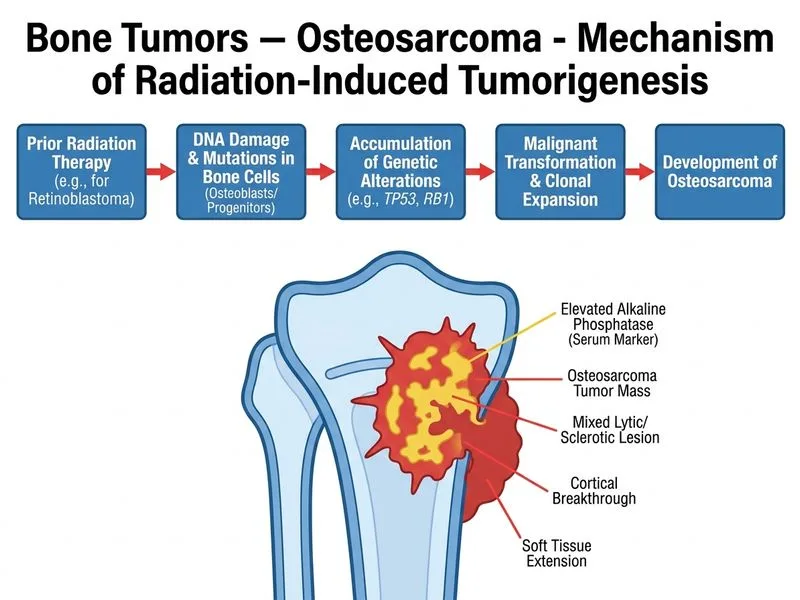
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.