## Clinical Diagnosis: Wallenberg Syndrome (Lateral Medullary Syndrome) — Acute Ischemic Stroke Management The clinical presentation — ipsilateral facial sensory loss, contralateral body pain/temperature loss, nystagmus, vertigo — is pathognomonic for **lateral medullary infarction (Wallenberg syndrome)**, caused by occlusion of the posterior inferior cerebellar artery (PICA) or vertebral artery. ### Anatomical Basis **Key Point:** The lateral medullary lesion damages: - **Trigeminal nucleus/tract (CN V)** → ipsilateral facial pain/temperature loss - **Spinothalamic tract** → contralateral body pain/temperature loss - **Vestibular nuclei** → vertigo, nausea, vomiting, nystagmus - **Nucleus ambiguus (CN IX, X)** → potential dysphagia/dysarthria - **Inferior cerebellar peduncle** → ipsilateral limb ataxia ### Management Algorithm ``` Acute ischemic stroke confirmed on MRI ↓ Time window assessment < 4.5 hours + no contraindications → Thrombolysis with IV alteplase (FIRST-LINE) > 4.5 hours or contraindications → Antiplatelet therapy + neurology consultation ``` ### Why Thrombolysis with Alteplase Is Correct **High-Yield (Harrison 21e, Ch 379):** For **acute ischemic stroke**, IV alteplase (0.9 mg/kg, max 90 mg) within **4.5 hours of symptom onset** is the standard of care and the most appropriate next step when the patient presents within the eligible time window. The stem states "acute onset" and explicitly offers thrombolysis within 4.5 hours as an option — this implies the patient is within the window. Thrombolysis is indicated for posterior circulation strokes including lateral medullary infarction, provided there are no contraindications. **Clinical Pearl:** The question stem does NOT state the patient is outside the 4.5-hour window. When a patient with confirmed acute ischemic stroke presents within 4.5 hours and has no stated contraindications, **thrombolysis takes priority over antiplatelet therapy**. Giving aspirin before thrombolysis is actually contraindicated within 24 hours of alteplase administration. ### Why NOT Aspirin Stat (Option D) Aspirin 300 mg stat is appropriate **only if thrombolysis is not indicated** (i.e., outside the 4.5-hour window or contraindications exist). Administering aspirin before or instead of alteplase when the patient is within the thrombolytic window is suboptimal and potentially harmful (increased bleeding risk post-thrombolysis). ### Why NOT Intubation (Option A) No indication: patient is alert, breathing spontaneously, no mention of airway compromise or altered consciousness. ### Why NOT High-Dose Steroids (Option B) No evidence for benefit in acute ischemic stroke; steroids are reserved for vasogenic edema in hemorrhagic stroke or mass effect. **Mnemonic:** **PICA** = Posterior Inferior Cerebellar Artery → **Wallenberg** (lateral medulla) → **Ipsilateral face, Contralateral body** sensory loss. In acute window → **Thrombolyse first**. [cite:Harrison 21e Ch 379; AHA/ASA Stroke Guidelines 2019] 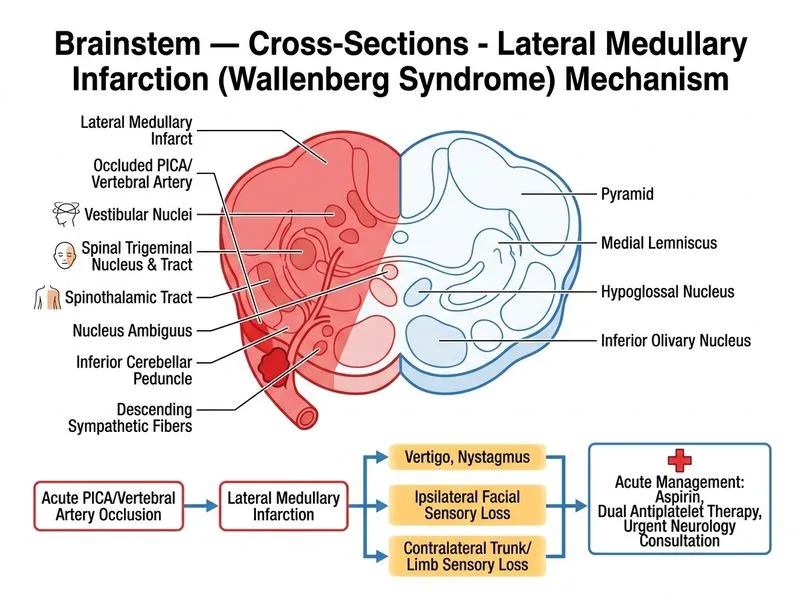
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.