## Anatomical Variants of Calot Triangle and Biliary Tree ### Clinical Scenario Analysis **Key Point:** The surgeon identifies a structure in the medial position of Calot triangle that appears to communicate directly with the common bile duct, but anatomy is obscured by inflammation. This is a **red flag** for an aberrant bile duct variant. ### Anatomical Variants of the Biliary Tree | Variant | Frequency | Location | Clinical Significance | Risk | |---------|-----------|----------|----------------------|------| | **Aberrant right hepatic duct** | 10–15% | Enters common hepatic duct or cystic duct directly | May be mistaken for cystic duct | **VERY HIGH** | | Short cystic duct | Common | Joins CBD directly | Usually identifiable | Low | | Accessory duct of Luschka | 5–10% | Gallbladder bed to bile ducts | Bile leak risk | Medium | | Low cystic duct insertion | Uncommon | Joins CBD at acute angle | Identifiable with care | Low | | Spiral valves (Heister) | Normal variant | Cystic duct | Aids identification | None | ### Why This Is an Aberrant Right Hepatic Duct **High-Yield:** When the medial structure of Calot triangle: 1. Appears to communicate directly with the common bile duct 2. Is obscured by inflammation (cannot use CVS technique) 3. Does NOT appear to be the typical cystic duct ...the most likely diagnosis is an **aberrant right hepatic duct** (anomalous entry of right hepatic duct into the cystic duct, common hepatic duct, or common bile duct). **Clinical Pearl:** Aberrant right hepatic ducts account for 10–15% of major bile duct injuries during cholecystectomy. They are the leading cause of iatrogenic bile duct injury because they mimic the cystic duct. ### Safest Management Strategy **Warning:** Proceeding with laparoscopic ligation without clear identification is contraindicated. The correct approach is: 1. **Convert to open surgery** — allows better visualization and control 2. **Perform intraoperative cholangiography (IOC)** — defines the biliary anatomy definitively 3. **Careful dissection under direct visualization** — identify all ducts before ligation 4. **If aberrant duct confirmed** — ligate only after confirming it does NOT drain the right lobe of liver **Mnemonic:** **CHOP** = Convert to open, Have IOC, Observe anatomy, Proceed cautiously ### Why Other Options Are Incorrect **Short cystic duct:** While common, a short duct should still be identifiable and should NOT appear to communicate directly with the CBD in an anomalous way. Proceeding without confirmation risks injury. **Accessory duct of Luschka:** This is a small duct from the gallbladder bed to the bile ducts (not from the liver parenchyma). It causes bile leak, not major duct injury, and would not be the medial boundary of Calot triangle. **Low insertion of cystic duct:** Even with low insertion, the cystic duct should be clearly identifiable with CVS. The obscured anatomy and apparent direct communication suggest a more complex variant. ### Intraoperative Cholangiography Technique ```mermaid flowchart TD A[Obscured anatomy in Calot triangle]:::outcome --> B{Can CVS be achieved?}:::decision B -->|Yes| C[Proceed with laparoscopic ligation]:::action B -->|No| D[Convert to open cholecystectomy]:::action D --> E[Perform intraoperative cholangiography]:::action E --> F{Aberrant duct identified?}:::decision F -->|Yes| G[Ligate only after confirming drainage pattern]:::action F -->|No| H[Standard cholecystectomy]:::action G --> I[Complete cholecystectomy]:::outcome H --> I ``` **High-Yield:** IOC is the gold standard for resolving ambiguous anatomy. It: - Defines the entire biliary tree - Identifies aberrant ducts - Confirms cystic duct anatomy - Detects stones in the CBD - Reduces bile duct injury rate from ~0.7% to ~0.1% [cite:Standring Anatomy 42e Ch 68, Sabiston Textbook of Surgery 21e Ch 51] 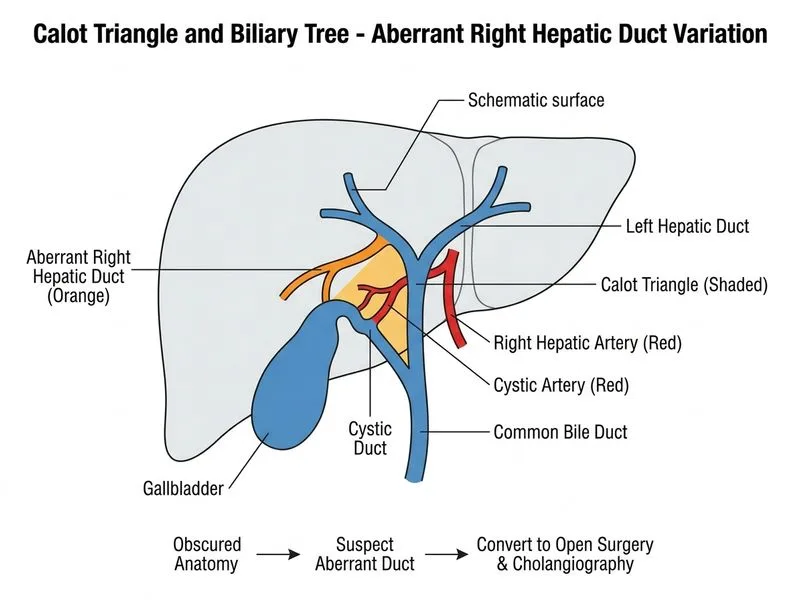
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.