## Anomalous Arterial Anatomy in the Calot Triangle ### Anatomical Variants of the Hepatic Artery | Variant | Frequency | Course | Clinical Significance | |---------|-----------|--------|----------------------| | Right hepatic artery via Calot triangle | 15–25% | Crosses through/near Calot triangle | High risk of iatrogenic injury | | Accessory right hepatic artery | 5–10% | May be small but supplies right lobe | Ligation causes ischemia | | Left hepatic from gastroduodenal | 2–5% | Anomalous origin | Rare but critical | **Key Point:** Any artery identified in the Calot triangle must be presumed to supply liver parenchyma. Ligation without confirmation causes hepatic ischemia and necrosis. ### Recognition and Management 1. **Identify the vessel:** Anomalous arteries in Calot triangle are typically pulsatile and bleed briskly if divided 2. **Preserve the vessel:** Carefully dissect the gallbladder away from the artery 3. **Complete cholecystectomy:** The artery can be left in situ; it does not impede safe dissection 4. **Document findings:** Intraoperative note should record the anomaly for future reference **High-Yield:** Hepatic artery injury is one of the most serious complications of cholecystectomy. Even small "accessory" arteries may be the sole blood supply to a hepatic segment. Ligation results in segmental infarction and potential abscess formation. **Clinical Pearl:** The key to avoiding hepatic artery injury is recognizing that ANY pulsatile structure in the Calot triangle is likely an artery. When in doubt, do not ligate—dissect carefully and preserve. ### Why Intraoperative Ultrasound Is Not Needed In the open setting with direct visualization, the pulsatile nature of the vessel and its course are diagnostic. USG adds no value once the vessel is identified under direct vision. 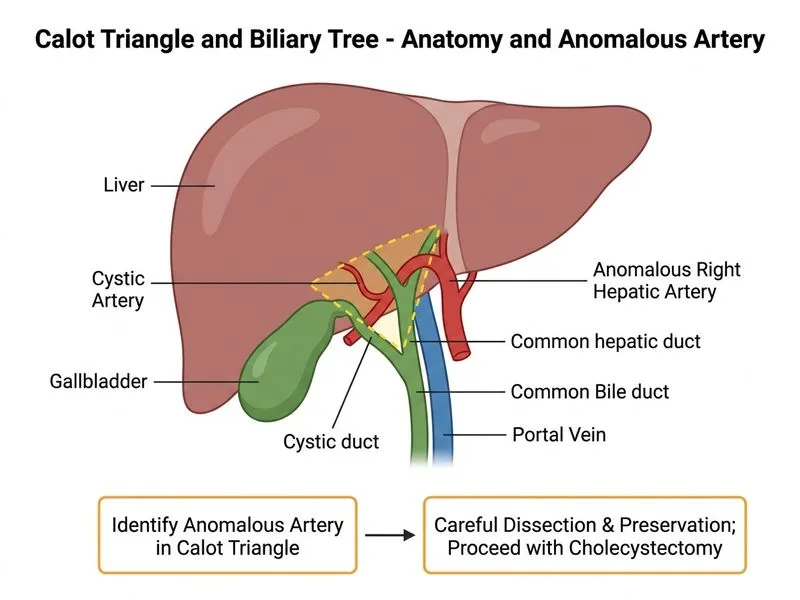
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.