## Two-Hit Hypothesis in BRCA1-Associated Breast Cancer **Key Point:** The two-hit hypothesis (Knudson hypothesis) states that both copies of a tumor suppressor gene must be inactivated for cancer to develop. In this case, the patient inherited one mutant BRCA1 allele (germline hit), and the tumor acquired loss of the second (wild-type) allele (somatic hit). ### Molecular Basis of BRCA1 Inactivation **High-Yield:** BRCA1 is a tumor suppressor gene that encodes a protein essential for homologous recombination (HR) DNA repair. Loss of both alleles results in: 1. **Impaired homologous recombination repair** → inability to fix double-strand breaks (DSBs) 2. **Accumulation of unrepaired DNA damage** → genomic instability 3. **Increased mutation rate** → acquisition of additional oncogenic mutations 4. **Loss of cell cycle checkpoint control** → uncontrolled proliferation ### Why This Patient Developed Cancer ```mermaid flowchart TD A[Inherited BRCA1 mutation<br/>Germline hit]:::outcome --> B[All cells carry one mutant allele] B --> C[Somatic event in breast epithelial cell<br/>Loss of wild-type allele<br/>LOH at BRCA1 locus]:::action C --> D[Complete loss of BRCA1 protein<br/>Both alleles non-functional]:::urgent D --> E[Severe HR DNA repair deficiency] E --> F[Accumulation of DSBs and mutations] F --> G[Malignant transformation]:::outcome ``` **Clinical Pearl:** The presence of LOH (loss of heterozygosity) at the BRCA1 locus in the tumor is the smoking gun for the two-hit mechanism. The tumor has lost the entire wild-type allele, proving that both copies were inactivated. ### BRCA1 Function and Cancer Risk | Function | Normal BRCA1 | Absent BRCA1 | |----------|-------------|---------------| | Homologous recombination | Intact | Severely impaired | | Double-strand break repair | Efficient | Inefficient | | Cell cycle checkpoint | Functional | Compromised | | Genomic stability | Maintained | Unstable | | Cancer risk | Baseline | 45–87% lifetime risk | **Mnemonic:** **BRCA-2-HITS** — Both alleles must be inactivated: one germline (inherited), one somatic (acquired in tumor). **Warning:** Do NOT confuse BRCA1 inactivation with haploinsufficiency. BRCA1 is a classic recessive tumor suppressor — one functional copy is usually sufficient for normal DNA repair. Cancer develops only when BOTH copies are lost. [cite:Robbins 10e Ch 7] 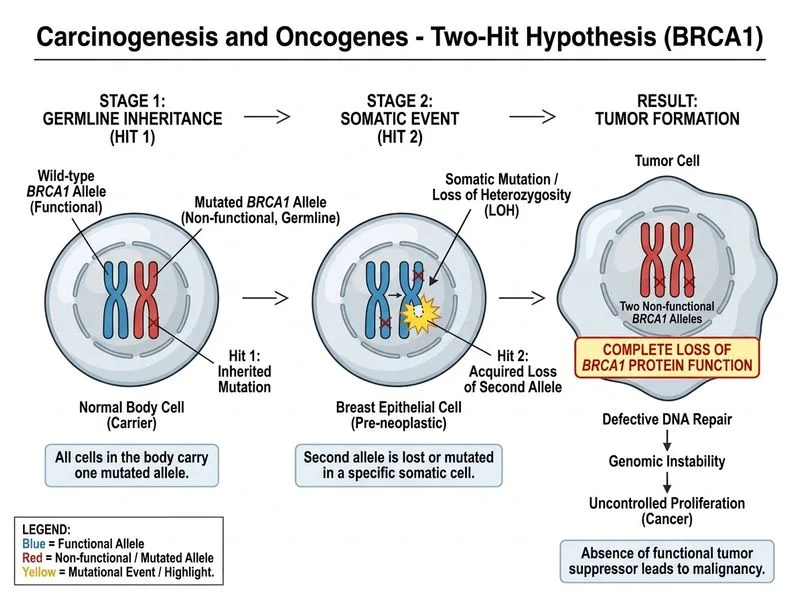
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.