## Clinical Diagnosis: Posterior Subcapsular Cataract ### Key Morphological Features **Key Point:** Posterior subcapsular cataracts (PSC) are characterized by **granular or plaque-like opacities at the posterior lens surface**, causing **disproportionate functional vision loss** relative to the extent of opacity. ### Distinguishing Characteristics of Posterior Subcapsular Cataract | Feature | Posterior Subcapsular | Cortical | Nuclear Sclerotic | Snowflake (True Diabetic) | |---------|----------------------|----------|-------------------|---------------------------| | **Location** | Posterior pole, subcapsular | Lens periphery | Central nucleus | Anterior and posterior cortex | | **Appearance** | Granular, bread-crumb, plaque | Radial striations, vacuoles | Uniform browning | Snowflake-like, needle-like opacities | | **Onset** | Rapid (weeks to months) | Gradual (years) | Gradual (years) | Very rapid (days to weeks) | | **Functional impact** | **Disproportionate** to opacity | Proportionate | Proportionate | Severe, rapid | | **Glare/haloes** | Marked | Mild to moderate | Mild | Moderate to severe | | **Reading difficulty** | Severe (near vision) | Mild | Mild | Severe | ### Clinical Pearl **Clinical Pearl:** The hallmark of PSC is **functional vision loss out of proportion to the clinical appearance of opacity**. A patient may have only 20% lens opacification but 6/18 vision due to the posterior location disrupting the visual axis. ### Pathophysiology 1. **Location-dependent impact:** Posterior lens fibers are in the direct path of light rays entering the eye 2. **Glare mechanism:** Posterior opacities scatter light rays, causing significant glare and haloes 3. **Near vision affected first:** Accommodation increases lens thickness, worsening PSC symptoms 4. **Rapid progression:** Metabolic stress on posterior epithelial cells leads to swift opacification ### High-Yield Associations **High-Yield:** Posterior subcapsular cataracts are strongly associated with: - **Chronic corticosteroid use** (most common iatrogenic cause) - **Diabetes mellitus** (especially with poor glycemic control, as in this case: HbA1c 9.2%) - **Myotonic dystrophy** - **Chronic uveitis** - **Radiation exposure** - **Retinitis pigmentosa** **Mnemonic: CURD-M** — **C**orticosteroids, **U**veitis, **R**adiation, **D**iabetes, **M**yotonic dystrophy ### Clinical Presentation Correlation This patient has: - **Rapid onset** (3 weeks) — typical of PSC - **Disproportionate symptoms** — 6/18 vision with mild external opacity - **Marked glare** — characteristic of posterior location - **Reading difficulty** — near vision affected first in PSC - **Bilateral symmetric presentation** — consistent with metabolic cause (diabetes) - **Risk factor present** — poorly controlled diabetes (HbA1c 9.2%) The **bread-crumb or rosette appearance** is the classic slit-lamp finding in PSC. ### Differential Consideration: Snowflake Cataract **Warning:** Do not confuse PSC with **snowflake (true diabetic) cataract**, which is a rare, rapidly progressive cataract occurring in young, poorly controlled diabetics. Snowflake cataracts present with needle-like opacities in both anterior and posterior cortex, occurring over **days to weeks**, and are reversible in early stages with glycemic control. This patient's presentation (granular posterior opacities, 52 years old, 3-week onset) is more consistent with PSC secondary to diabetes, not true snowflake cataract. 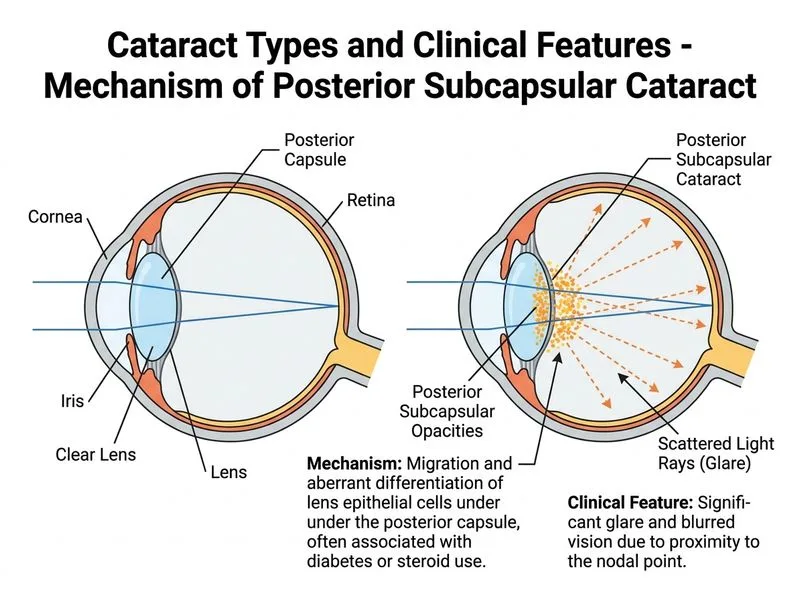
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.