## Post-Treatment Follow-Up for CIN 3 ### Clinical Scenario Summary The patient has been treated for CIN 3 with LEEP, achieving clear margins and negative endocervical curettage — indicators of complete excision. The question addresses the optimal surveillance strategy to detect recurrence or persistent disease. ### Post-Treatment Surveillance Algorithm ```mermaid flowchart TD A[CIN 3 treated with LEEP]:::outcome --> B{Margins clear & ECC negative?}:::decision B -->|Yes| C[HPV testing at 6 & 12 months]:::action C --> D{Both HPV tests negative?}:::decision D -->|Yes| E[Return to routine screening]:::outcome D -->|No| F[Colposcopy + biopsy]:::action F --> G{Recurrent/persistent disease?}:::decision G -->|Yes| H[Repeat excision or ablation]:::action G -->|No| I[Continue surveillance]:::action B -->|No| J[Repeat excision/conization]:::action ``` ### High-Yield Follow-Up Strategy **Key Point:** After successful treatment of CIN 3 with clear margins and negative endocervical curettage, HPV-based follow-up (HPV testing at 6 and 12 months) is superior to cytology-based follow-up because: - HPV persistence/recurrence is the strongest predictor of treatment failure - Negative HPV at both 6 and 12 months indicates <5% risk of recurrent CIN 2/3 - HPV testing has higher sensitivity than repeat cytology for detecting residual disease **High-Yield:** If both HPV tests are negative at 6 and 12 months, the patient can return to routine cervical cancer screening (standard 3-year or 5-year intervals depending on screening protocol). ### Comparison of Follow-Up Modalities | Modality | Sensitivity | Specificity | Timing | Preferred? | |----------|-------------|-------------|--------|------------| | **HPV testing (6 & 12 mo)** | High (~95%) | High (~90%) | 6 mo, 12 mo | **YES** | | **Cytology (annual Pap)** | Lower (~70%) | High | Annual | No — less sensitive | | **Colposcopy (3 mo)** | Very high | Moderate | 3 mo | Only if HPV+ | | **Hysterectomy** | N/A | N/A | N/A | Not indicated | ### Why Other Options Are Incorrect **Annual Pap smear (Option A):** Cytology-based follow-up is less sensitive than HPV testing for detecting recurrent/persistent CIN. After treatment of CIN 3, HPV-based surveillance is the standard of care. **Repeat colposcopy at 3 months (Option C):** Colposcopy is reserved for HPV-positive results or abnormal cytology, not routine surveillance. Performing colposcopy on all treated CIN 3 patients is not evidence-based and increases unnecessary procedures. **Hysterectomy (Option D):** Hysterectomy is not indicated after successful treatment of CIN 3 with clear margins. The patient is young (28 years), and hysterectomy carries surgical morbidity. Hysterectomy may be considered only if recurrent CIN 3 develops despite surveillance. ### Clinical Pearl **Clinical Pearl:** The negative endocervical curettage is particularly important — it indicates that dysplasia does not extend into the endocervical canal, reducing the risk of residual disease and justifying conservative follow-up rather than repeat excision. ### Management Summary **Mnemonic: HPV-SAFE** — **H**PV testing at **P**ost-treatment intervals (6 and 12 months), **S**urvey for **A**bsence of **F**ailure, then **E**xit to routine screening if both negative. 1. HPV test at 6 months 2. HPV test at 12 months 3. If both negative → routine screening 4. If either positive → colposcopy with biopsy 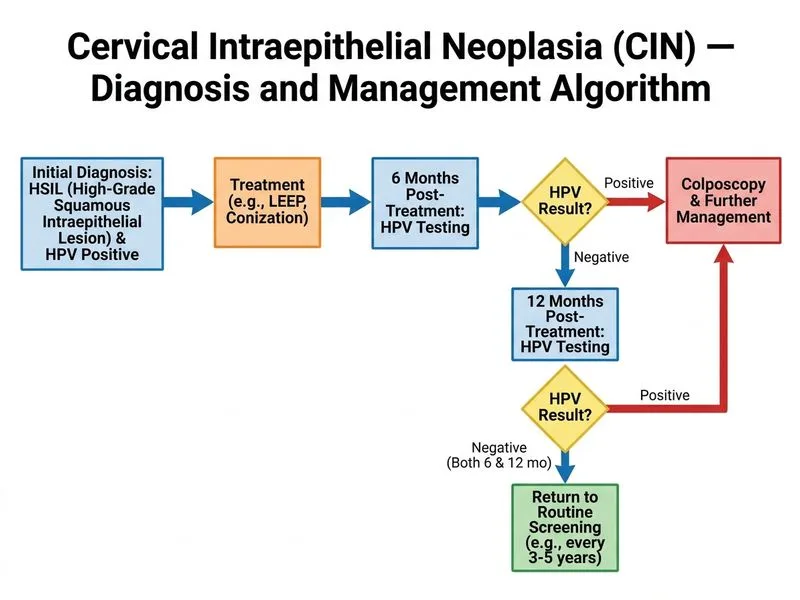
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.