## Investigation of Choice for TOLAC Candidacy Assessment ### Clinical Context Trial of labor after cesarean (TOLAC) is an attempt at vaginal delivery in women with a prior cesarean section. Success rates are ~60–80% in appropriately selected candidates. **Uterine scar integrity** is critical to assess before TOLAC; scar dehiscence (asymptomatic separation) or rupture (symptomatic with fetal distress) is a rare but serious complication (~0.3–0.5% risk). ### Why Transvaginal Ultrasound is Correct **Key Point:** Transvaginal ultrasound measurement of lower uterine segment (LUS) thickness is the **non-invasive imaging modality of choice** to assess scar integrity and predict risk of dehiscence in TOLAC candidates. #### Mechanism of Assessment 1. **Lower uterine segment thickness** measured at the site of prior cesarean scar - Measured in the **sagittal plane** during transvaginal scan - Thickness **≥2.5 mm** associated with lower dehiscence risk - Thickness **<2.5 mm** (especially <1.5 mm) suggests thin scar; increased dehiscence risk 2. **Scar defects** visualized as: - Discontinuity in the myometrium - Hypoechoic or anechoic areas within scar - Loss of normal layering 3. **Predictive value:** - Sensitivity ~70–80% for identifying thin/defective scars - Specificity ~60–70% - Negative predictive value high (reassuring if normal) **High-Yield:** Normal LUS thickness **≥2.5 mm** on transvaginal ultrasound is reassuring and **supports TOLAC candidacy**. Thin scar (<1.5 mm) warrants counseling about increased dehiscence risk but does not absolutely contraindicate TOLAC if patient is counseled and monitored closely. ### Role of Other Investigations | Investigation | Role in TOLAC Assessment | Why Not First-Line | |---|---|---| | **MRI of pelvis** | Excellent soft-tissue resolution; can visualize scar defects and pelvic anatomy | Expensive, time-consuming, not routinely available; reserved for specific indications (e.g., suspected uterine anomaly). | | **Pelvimetry (X-ray/CT)** | Assesses pelvic bony dimensions; useful if cephalopelvic disproportion suspected | Radiation exposure; this patient already has CPD as indication for prior cesarean. Pelvimetry does NOT assess scar integrity. | | **Diagnostic laparoscopy** | Direct visualization of scar; gold standard for scar assessment | Invasive; carries risk of bowel/bladder injury; not indicated in asymptomatic patient. Reserved for specific concerns (e.g., suspected rupture). | **Clinical Pearl:** TOLAC is **contraindicated** in: - Prior classical (vertical) cesarean (scar in contractile segment; high rupture risk ~5–12%) - Recurrent indication (e.g., CPD) unless pelvimetry improved or fetal weight expected to be lower - Multiple prior cesareans (relative contraindication; individualize) - Maternal age >35 or BMI >30 (relative; not absolute) In this case, the patient has **one prior low-transverse cesarean** for CPD — TOLAC is reasonable if: 1. Transvaginal ultrasound shows adequate LUS thickness (≥2.5 mm) 2. Pelvimetry or clinical assessment suggests adequate pelvis for current pregnancy 3. Patient counseled on 0.3–0.5% uterine rupture risk **Mnemonic — TOLAC Criteria:** **T**ransverse prior scar (not classical), **O**ne prior cesarean (or carefully selected two), **L**ower uterine segment intact (≥2.5 mm on US), **A**dequate pelvis (no recurrent CPD), **C**ontinuous fetal monitoring available. --- ## Why Each Distractor is Wrong | Option | Reason | |---|---| | **MRI of the pelvis** | While MRI provides excellent soft-tissue detail, it is expensive, time-consuming, and not routinely available for routine TOLAC assessment. Transvaginal ultrasound is more practical, faster, and equally sensitive for scar assessment. MRI is reserved for specific indications (e.g., suspected uterine anomaly or complex anatomy). | | **Pelvimetry by X-ray or CT** | Pelvimetry assesses bony pelvic dimensions but does **not assess scar integrity**. Additionally, this patient already has CPD as the indication for her prior cesarean; pelvimetry would not change management unless pelvic dimensions are expected to improve (unlikely). Radiation exposure is an additional concern. | | **Diagnostic laparoscopy** | Laparoscopy is invasive, carries risk of bowel/bladder injury, and is not indicated in an asymptomatic patient. It is reserved for acute situations (e.g., suspected uterine rupture with fetal distress) or specific clinical concerns, not for routine TOLAC candidacy assessment. | 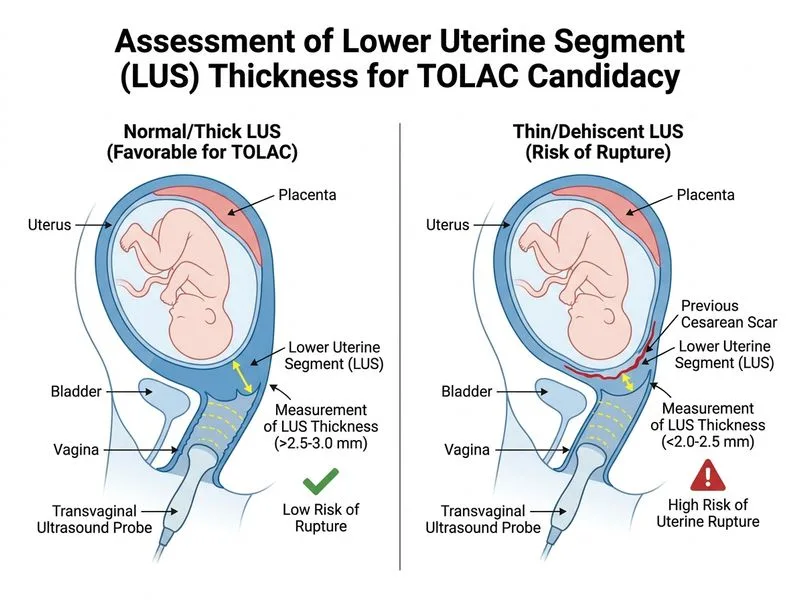
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.