## Clinical Context This patient has **Stage 3b CKD** (eGFR 35 mL/min/1.73m²) with: - Hypertensive nephrosclerosis (primary etiology) - Mild albuminuria (UACR 85 mg/g, microalbuminuria range) - Stable renal function over 6 months - **Prediabetes** (HbA1c 5.9%, fasting glucose 105 mg/dL) - Adequate BP control (132/78 mmHg) - Normal potassium (4.9 mEq/L) ## Evidence for SGLT2 Inhibitors in CKD **Key Point:** SGLT2 inhibitors (e.g., empagliflozin, dapagliflozin) have emerged as **cornerstone agents** for CKD protection across the spectrum—from early CKD to advanced stages—regardless of diabetes status [cite:KDIGO 2021, EMPA-KIDNEY trial]. ### Mechanism of Renal Protection 1. **Natriuresis and hemodynamic effects** — Reduce intraglomerular pressure 2. **Metabolic benefits** — Improve insulin sensitivity, reduce inflammation 3. **Anti-fibrotic effects** — Decrease TGF-β and myofibroblast activation 4. **Cardiovascular protection** — Reduce heart failure hospitalization and cardiovascular death **High-Yield:** The **EMPA-KIDNEY trial (2023)** demonstrated that empagliflozin reduced CKD progression and cardiovascular events in patients with CKD eGFR 20–90 mL/min/1.73m², **independent of diabetes status**. This is a paradigm shift — SGLT2-I are now recommended for all CKD patients, not just those with diabetes. ### Why SGLT2-I in This Patient? - Already on optimal ACE-I therapy (lisinopril 10 mg) - BP is at goal (132/78 mmHg) - **Prediabetic state** — SGLT2-I improve glucose metabolism and reduce progression to diabetes - **No contraindications** — eGFR 35 is well above the threshold for use; potassium is normal - **Dual benefit** — Slows CKD progression AND reduces cardiovascular risk ## Why Other Options Are Inferior | Option | Rationale for Rejection | |--------|-------------------------| | **Add amlodipine (CCB)** | BP is already at goal (132/78). Adding another CCB does not provide additional renal protection beyond what ACE-I offers. CCBs do not slow proteinuria or CKD progression as effectively as SGLT2-I or ACE-I. | | **Increase lisinopril to 20 mg** | Lisinopril 10 mg is a standard dose; doubling it offers marginal additional benefit and increases hyperkalemia risk (K already 4.9). No evidence supports higher ACE-I doses beyond standard therapy in stable CKD. | | **Add spironolactone 25 mg** | Spironolactone is a mineralocorticoid receptor antagonist (MRA) with some CKD benefit, but at eGFR 35 with K 4.9, adding an MRA carries significant **hyperkalemia risk**. MRA is typically reserved for advanced CKD with resistant proteinuria and careful K monitoring. SGLT2-I is safer and more effective. | **Warning:** Combining ACE-I + spironolactone at eGFR 35 risks dangerous hyperkalemia; this is a common trap. ## Clinical Pearl SGLT2 inhibitors are now **first-line add-on agents** for CKD, even in non-diabetic patients. They complement ACE-I/ARB therapy and provide synergistic renal and cardiovascular protection. The KDIGO 2021 guideline recommends SGLT2-I for all CKD patients with eGFR ≥20 mL/min/1.73m² (or albuminuria) to slow progression and reduce cardiovascular events. 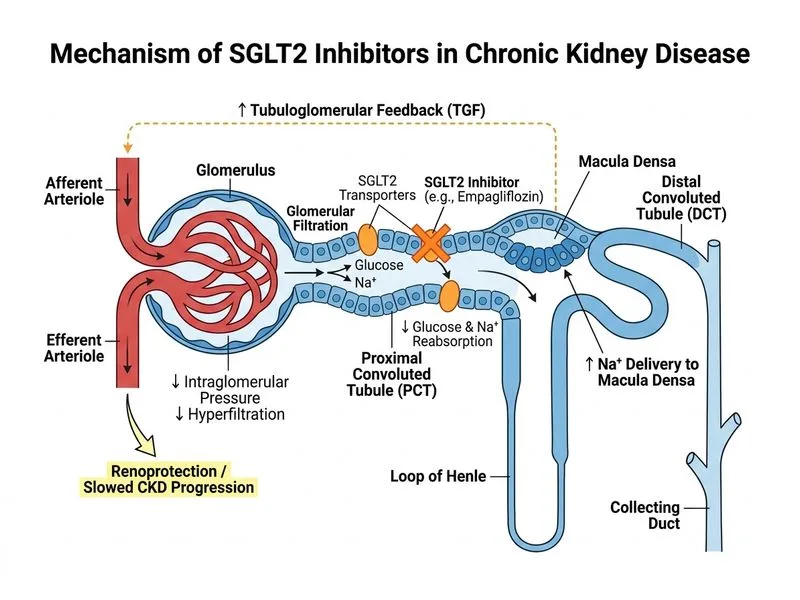
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.