## Clinical Presentation This patient has advanced CKD (stage 4) with symptomatic anemia (Hb 8.2 g/dL), secondary hyperparathyroidism (PTH 285 pg/mL), hyperphosphatemia (5.8 mg/dL), and hypocalcemia (7.9 mg/dL)—the classic triad of CKD mineral-bone disorder (MBD). Fatigue and dyspnea are consistent with moderate anemia. ## Pathophysiology of CKD-MBD ```mermaid flowchart TD A[Declining GFR]:::outcome --> B[Phosphate retention]:::outcome B --> C[↓ FGF23 initially]:::outcome C --> D[↓ 1,25-dihydroxyvitamin D]:::outcome D --> E[Hypocalcemia]:::outcome E --> F[↑ PTH secretion]:::outcome B --> F F --> G[Secondary hyperparathyroidism]:::outcome G --> H[Bone resorption + vascular calcification]:::urgent A --> I[Uremia + reduced EPO]:::outcome I --> J[Anemia]:::outcome ``` ## Management Strategy **Key Point:** In CKD stage 4 with symptomatic anemia and MBD, the priority is: 1. **Anemia correction** with ESA (target Hb 10–12 g/dL) to improve symptoms and reduce cardiovascular risk 2. **Phosphate control** with binders (calcium-free or non-calcium) to prevent hyperphosphatemia-driven PTH elevation 3. **Specialist nephrology referral** for comprehensive MBD management, including consideration of vitamin D analogs and calcimimetics if indicated **High-Yield:** ESA initiation is appropriate at Hb <10 g/dL in CKD stage 4. Iron status should be assessed (ferritin, TSAT) before ESA; iron supplementation (oral or IV) is often needed concurrently. Phosphate binders (e.g., sevelamer, lanthanum) should be started early to prevent further PTH escalation. **Clinical Pearl:** Hypocalcemia in CKD-MBD is typically NOT corrected acutely with IV calcium—this risks metastatic calcification and worsening hyperphosphatemia. Instead, phosphate control (via binders) allows PTH-driven calcium reabsorption and vitamin D metabolism to normalize over weeks. **Mnemonic:** **CKD-MBD Management = PEAS** - **P**hosphate binders (sevelamer, lanthanum) - **E**rythropoiesis-stimulating agents (ESA) - **A**ssess iron status and supplement - **S**pecialist referral for vitamin D analogs and calcimimetics ## Why NOT Acute IV Calcium? | Intervention | Why NOT in CKD-MBD | |--------------|-------------------| | IV calcium gluconate acutely | Risk of metastatic calcification, worsens hyperphosphatemia-driven PTH | | Calcitriol without phosphate control | Increases serum calcium × phosphate product, accelerates vascular calcification | | Protein restriction alone | Does not address phosphate retention or anemia; requires binders | [cite:KDIGO 2017 CKD-MBD Guidelines; Harrison 21e Ch 297] 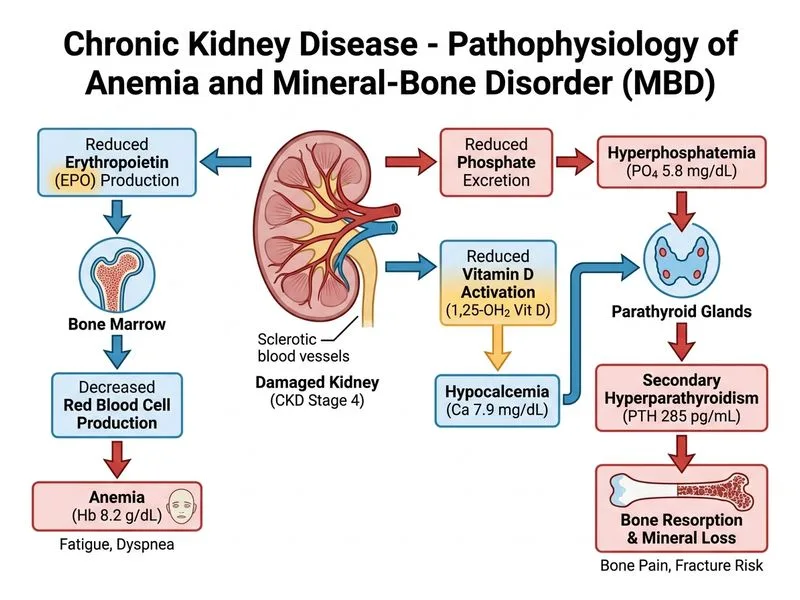
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.