## Diagnosis: Secondary Hyperparathyroidism with High-Turnover Bone Disease ### Clinical Presentation This patient presents with: - Symptomatic bone pain (hips, lower back) - Stage 3b CKD (eGFR 32) - Biochemical hallmarks: **elevated PTH (485 pg/mL), low calcium (7.2), elevated phosphate (4.8)** - Elevated bone-specific alkaline phosphatase - **Bone biopsy: increased osteoblast and osteoclast activity** — high bone turnover ### Pathophysiology of Secondary Hyperparathyroidism ```mermaid flowchart TD A[CKD eGFR ↓]:::outcome --> B[Phosphate retention]:::outcome A --> C[1,25-OH vitamin D ↓]:::outcome B --> D[Serum phosphate ↑]:::action C --> E[Serum calcium ↓]:::action D --> F[PTH secretion ↑]:::action E --> F F --> G[Parathyroid gland hyperplasia]:::outcome G --> H[Increased bone turnover]:::outcome H --> I[High-turnover bone disease]:::outcome ``` **Key Point:** Secondary hyperparathyroidism develops through a vicious cycle: 1. **Phosphate retention** → serum phosphate ↑ 2. **Reduced 1,25-OH vitamin D production** → serum calcium ↓ 3. **Hypocalcemia + hyperphosphatemia** → PTH secretion ↑↑ 4. **Chronic PTH excess** → parathyroid gland hyperplasia 5. **Result:** High bone turnover with increased osteoblast and osteoclast activity ### Biochemical Profile in Secondary Hyperparathyroidism | Parameter | Finding | Mechanism | |-----------|---------|----------| | PTH | ↑↑ (485 pg/mL) | Stimulus: hypocalcemia + hyperphosphatemia | | Calcium | ↓ (7.2 mg/dL) | Reduced 1,25-OH vitamin D + phosphate retention | | Phosphate | ↑ (4.8 mg/dL) | Reduced GFR → impaired urinary excretion | | 25-OH vitamin D | ↓ (18 ng/mL) | Substrate depletion + reduced 1α-hydroxylase | | Bone-specific ALP | ↑ | Osteoblast activity ↑ | | Bone biopsy | High turnover | Increased osteoblast + osteoclast activity | **High-Yield:** The **bone biopsy showing increased osteoblast AND osteoclast activity** is the gold standard for diagnosing high-turnover bone disease. This is pathognomonic for secondary hyperparathyroidism. ### Clinical Pearl: Why Bone Pain Occurs Bone pain in secondary hyperparathyroidism results from: - Rapid bone remodeling and microfractures - Increased osteoclastic resorption - Periosteal irritation from high bone turnover - This is different from osteomalacia pain, which is diffuse and associated with muscle weakness ### Management Strategy 1. **Phosphate binders:** Reduce serum phosphate (calcium-based or non-calcium agents) 2. **Vitamin D supplementation:** Calcitriol or active vitamin D analogs (paricalcitol, doxercalciferol) 3. **Calcimimetics:** Cinacalcet to suppress PTH secretion 4. **Dietary phosphate restriction:** <1000 mg/day 5. **Monitor:** PTH target in CKD 3–5 is 1.5–3× upper limit of normal **Mnemonic: SHPT** — Secondary Hyperparathyroidism in CKD = **S**erum phosphate ↑, **H**ypocalcemia, **P**arathyroid hyperplasia, **T**urbocharged bone turnover 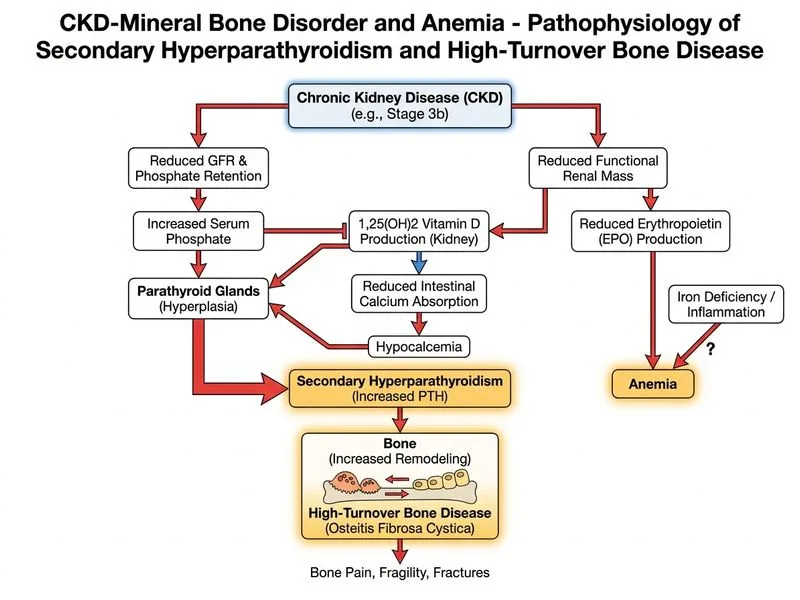
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.