## Clinical Diagnosis: Acute Compartment Syndrome **Key Point:** Compartment syndrome is a surgical emergency characterized by increased pressure within a closed fascial space, compromising tissue perfusion and function. Early recognition and intervention are critical to prevent irreversible tissue damage and loss of limb function. ### Pathophysiology In this case, the crush injury has caused soft tissue trauma and edema within the anterior compartment of the leg. The rigid fascial boundaries prevent expansion, leading to: 1. Increased intracompartmental pressure 2. Decreased capillary perfusion pressure 3. Ischemia of muscle and nerve tissue 4. Risk of rhabdomyolysis, acute kidney injury, and permanent disability ### Classic Clinical Features ("5 P's" — though pain and pressure are earliest) | Feature | Timing | Significance | |---------|--------|---------------| | **Pain out of proportion** | Early (within 6–8 hours) | Most sensitive early sign | | **Pain on passive stretch** | Early | Highly specific for compartment syndrome | | **Paresthesias** | Later (8–12 hours) | Nerve ischemia | | **Pallor** | Late | Indicates severe ischemia | | **Pulselessness** | Very late | Sign of irreversible damage | | **Paralysis** | Very late | Permanent if not intervened | **High-Yield:** Intact pulses and normal sensation do NOT exclude compartment syndrome. Vascular compromise and neurologic deficit are LATE findings; by then, irreversible muscle necrosis has begun. ### Diagnostic Approach **Clinical diagnosis** is based on: - High-risk mechanism (crush, fracture, tight cast, rhabdomyolysis) - Pain out of proportion to injury - Pain on passive stretch of muscles in the affected compartment - Tense, swollen compartment **Intracompartmental pressure measurement** is indicated when: - Clinical suspicion is high but not absolutely certain - Patient is unconscious or unreliable historian - Multiple compartments may be involved - Borderline clinical presentation **Fasciotomy threshold:** Pressure ≥30 mmHg absolute, or within 30 mmHg of diastolic BP ("delta P ≤ 30"), mandates urgent surgical decompression. ### Why This Patient Needs Pressure Measurement and Fasciotomy The patient has: - Crush injury (high-risk mechanism) - Severe pain out of proportion (6 hours post-injury) - Pain on passive dorsiflexion (stretch of anterior compartment muscles) - Tense leg swelling - Intact pulses and sensation (does NOT rule out early compartment syndrome) **Clinical Pearl:** The presence of normal neurovascular exam in the first 6–8 hours does NOT exclude compartment syndrome. Waiting for late signs (paresthesia, pallor, pulselessness, paralysis) results in permanent disability or amputation. ### Management Algorithm ```mermaid flowchart TD A[Crush injury / fracture / tight cast]:::outcome --> B{High clinical suspicion<br/>for compartment syndrome?}:::decision B -->|Yes: pain out of proportion<br/>+ pain on passive stretch| C[Measure intracompartmental pressure]:::action B -->|No clear signs| D[Observe closely, repeat exam q1h]:::action C --> E{Pressure ≥30 mmHg<br/>or ≤30 mmHg from diastolic?}:::decision E -->|Yes| F[Urgent fasciotomy]:::urgent E -->|No, but high suspicion| G[Repeat pressure in 1–2 hours<br/>or proceed to fasciotomy if clinical worsening]:::action F --> H[Prevent rhabdomyolysis complications]:::outcome D --> I{Worsening pain<br/>or new neurologic signs?}:::decision I -->|Yes| C I -->|No| J[Discharge with strict follow-up]:::action ``` **Tip:** In NEET PG exams, if the stem describes pain out of proportion + pain on passive stretch + high-risk mechanism, the answer is almost always "measure pressure and fasciotomize if elevated." Do NOT wait for late signs. ### Why Other Options Are Wrong **Option 1 (Antibiotics and observation):** Compartment syndrome is a mechanical emergency, not an infection. Antibiotics are irrelevant. Observation alone allows irreversible ischemic damage to progress. **Option 4 (Ice, elevation, NSAIDs):** These are appropriate for simple contusion or mild swelling, NOT for compartment syndrome. Elevation may worsen compartment pressure by reducing perfusion gradient. Waiting 12 hours for imaging is catastrophic — by then, muscle necrosis is established. [cite:Rockwood & Green's Fractures in Adults 9e Ch 1; Campbell's Operative Orthopaedics 13e Ch 48] 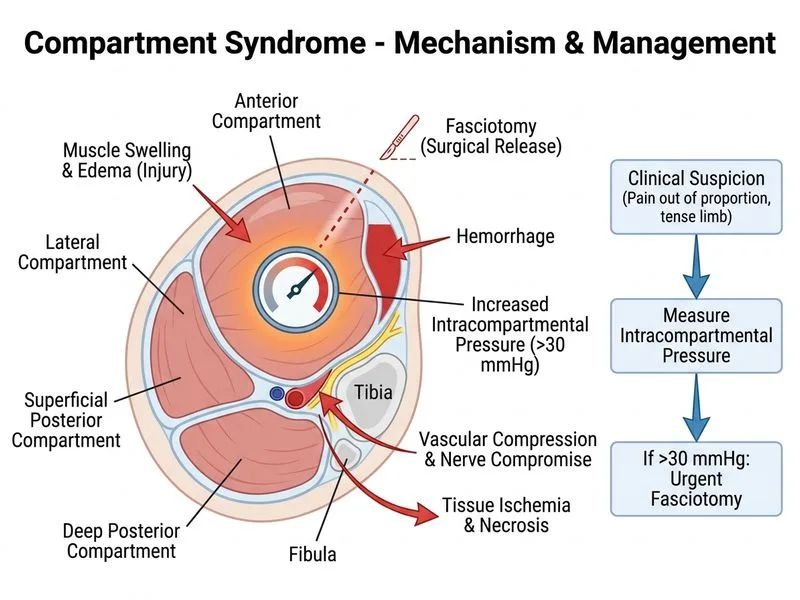
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.