## Critical Pressure Threshold in Compartment Syndrome **Key Point:** The critical threshold for intracompartmental pressure above which fasciotomy is indicated in acute compartment syndrome is **30 mmHg** (or when compartment pressure comes within 30 mmHg of diastolic blood pressure — the "Delta P" concept). ### Standard Fasciotomy Threshold **High-Yield:** According to Rockwood & Green's *Fractures in Adults* and standard orthopedic teaching: - Fasciotomy is indicated when intracompartmental pressure **exceeds 30 mmHg** (absolute threshold) - The more clinically nuanced criterion: **Delta P = Diastolic BP − Compartment Pressure ≤ 30 mmHg** This Delta P concept accounts for individual variation in perfusion pressure and is preferred in hypotensive patients (e.g., polytrauma), where a compartment pressure of 30 mmHg may still be dangerous. ### Pressure Interpretation Guide | Pressure Range | Clinical Significance | |---|---| | < 20 mmHg | Generally safe; observe clinically | | 20–30 mmHg | Borderline; monitor closely with clinical signs | | **> 30 mmHg** | **Fasciotomy indicated** | | > 45 mmHg | Emergent fasciotomy; irreversible tissue necrosis imminent if not decompressed | ### Why 30 mmHg? **Clinical Pearl:** Capillary perfusion pressure in muscle is approximately 20–30 mmHg. When intracompartmental pressure exceeds this range, local tissue perfusion is compromised, leading to ischemia → necrosis → Volkmann's contracture if untreated. - 45 mmHg represents the threshold for **imminent irreversible damage**, not the initial fasciotomy trigger - 30 mmHg is the universally taught and most commonly cited fasciotomy threshold in standard orthopedic references **Mnemonic:** **"30 = Go"** — When compartment pressure hits 30 mmHg, it's time to perform fasciotomy. [cite: Rockwood & Green's Fractures in Adults, 8th Ed., Ch. 1; Matsen FA — Compartment Syndrome] 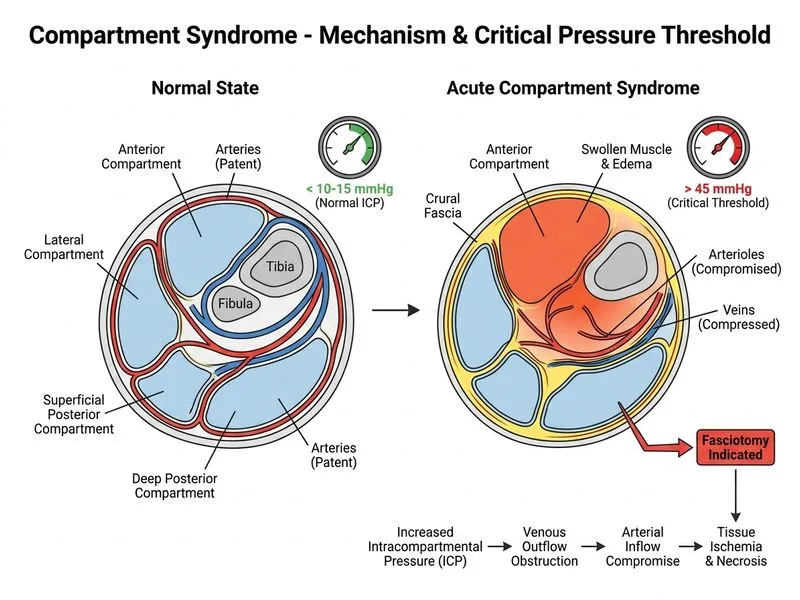
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.