## Diagnosis and Rationale **Key Point:** Acute compartment syndrome with classic clinical signs in a conscious, cooperative patient is a surgical emergency requiring **immediate fasciotomy** — compartment pressure measurement is NOT required before proceeding and should not delay definitive treatment. ## Clinical Features of Compartment Syndrome The classic presentation includes the **5 P's**: | Feature | Timing | Clinical Significance | | --- | --- | --- | | **Pain** (out of proportion) | Early & most sensitive | Present before other signs | | **Pressure** (tense compartment) | Early | Objective finding | | **Paresthesia** | Intermediate | Nerve ischemia | | **Pallor** | Late | Vascular compromise | | **Pulselessness** | Very late | Irreversible damage | **High-Yield:** Pain with passive stretch of muscles in the affected compartment is the single most sensitive clinical sign. This patient has **three cardinal signs**: pain out of proportion, pain on passive stretch, and tense compartment swelling — this constitutes a clinical diagnosis of compartment syndrome. ## Management Algorithm In a **conscious, cooperative patient** with clear clinical signs of compartment syndrome, the standard of care per Rockwood & Green's Fractures in Adults and Campbell's Operative Orthopaedics is: > **Immediate fasciotomy without waiting for compartment pressure measurement.** Compartment pressure measurement is reserved for: - Unconscious or sedated patients - Patients with altered mental status (polytrauma, intoxication) - Equivocal or borderline clinical findings - Patients who cannot reliably report pain (e.g., spinal cord injury) ## Why Option B Is Incorrect Here The stem describes a **conscious, cooperative 28-year-old** with **unequivocal clinical signs**. Delaying fasciotomy to measure compartment pressure in this scenario: - Wastes critical time (irreversible muscle necrosis begins within 6–8 hours of ischemia) - Is not the standard of care for a clinically obvious diagnosis - Risks permanent neuromuscular damage **Clinical Pearl (Harrison's / Campbell's):** Every 30-minute delay in fasciotomy after clinical diagnosis increases the risk of permanent functional deficit. The window for complete recovery narrows rapidly after 6 hours of ischemia — this patient is already at the 6-hour mark. ## Compartment Pressure Thresholds (for reference) When measurement IS indicated: - Absolute pressure **≥30 mmHg** (Whitesides criterion) OR **≥40 mmHg** (some high-volume trauma centers) - **Delta P ≤30 mmHg** (diastolic BP minus compartment pressure) — most widely accepted threshold ## Why Other Options Are Wrong - **C (Elevation + ice + monitoring):** Elevation reduces perfusion pressure and worsens ischemia in compartment syndrome — contraindicated. - **D (Mannitol + fluids):** No role as primary treatment; may be adjunctive in rhabdomyolysis but does not decompress the compartment. [cite: Campbell's Operative Orthopaedics, 14th ed.; Rockwood & Green's Fractures in Adults, 9th ed., Ch. 1] 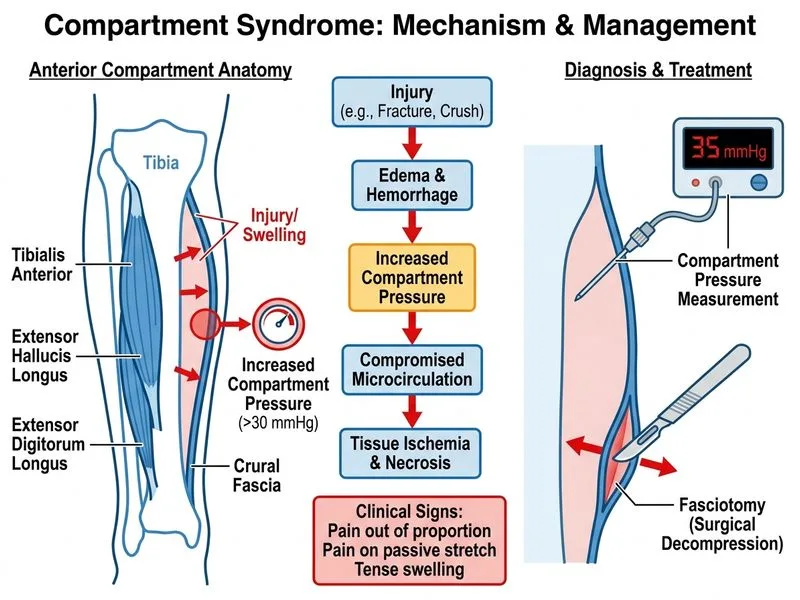
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.