## Diagnosis: Gonococcal Conjunctivitis **Key Point:** Gonococcal conjunctivitis (caused by *Neisseria gonorrhoeae*) is a medical emergency that can rapidly progress to corneal perforation and blindness if untreated. ### Clinical Features - Acute onset (2–7 days post-exposure) - Bilateral conjunctival injection - Thick, purulent (creamy) discharge — hallmark finding - Mild to moderate photophobia - Gram-negative intracellular diplococci on Gram stain ### Management Rationale **Systemic therapy is mandatory** because: 1. Topical antibiotics alone do NOT achieve adequate intraocular penetration 2. Risk of rapid corneal involvement and perforation 3. Concurrent urogenital infection is likely **Recommended regimen:** - **Intravenous ceftriaxone 1 g stat** (or 500 mg IM if IV unavailable) - **Topical cephalosporin drops** (cefazolin 5% or ceftazidime 5%) hourly - **Systemic doxycycline 100 mg BD for 7 days** (covers concurrent *Chlamydia*) ### Why Systemic Therapy? Gonococcal infection has a propensity for: - Rapid stromal invasion - Corneal ulceration and melting - Endophthalmitis if untreated **High-Yield:** Gonococcal conjunctivitis is the only bacterial conjunctivitis that requires **both systemic and topical antibiotics**. **Clinical Pearl:** Neonatal gonococcal ophthalmia neonatorum (acquired during birth) presents at 2–5 days of life and is a medical emergency — prevented by routine prophylaxis (silver nitrate 1% or erythromycin ointment). ### Differential Considerations - **Chlamydial conjunctivitis:** Slower onset (7–14 days), milder discharge, requires systemic doxycycline but not IV ceftriaxone - **Meningococcal conjunctivitis:** Rare; similar presentation but associated systemic meningococcemia [cite:Parson's Diseases of the Eye 21e Ch 5] 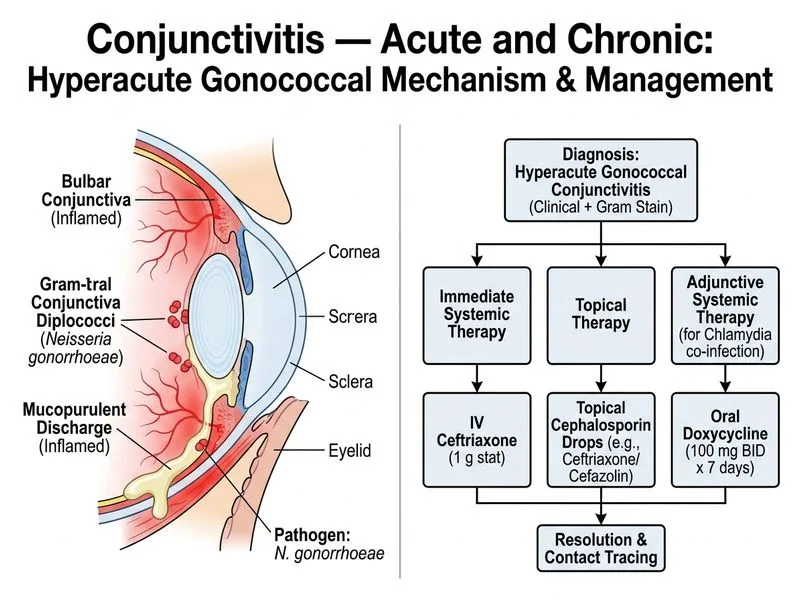
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.