## Clinical Diagnosis: Atopic Keratoconjunctivitis (AKC) **Key Point:** AKC is a chronic, bilateral allergic inflammation of the conjunctiva and cornea, typically affecting older adults (40–60 years) with a personal or family history of atopy (eczema, asthma, allergic rhinitis). ### Differential Diagnosis of Chronic Allergic Conjunctivitis | Feature | AKC | VKC | SAC | Chronic Bacterial | |---------|-----|-----|-----|-------------------| | **Age** | 40–60 years | 5–25 years | Any age | Any age | | **Seasonality** | Perennial, worse in winter | Seasonal (spring/summer) | Seasonal | Non-seasonal | | **Discharge** | Ropy, stringy, mucoid | Thick, ropy | Watery | Purulent | | **Papillae location** | Upper tarsal (mild) | Giant papillae (>1 mm) | Small papillae | Absent | | **Follicles** | Absent | Absent | Absent | Present | | **Lid involvement** | Lichenification, dermatitis | Absent | Absent | Absent | | **Photophobia** | Mild to moderate | Severe | Mild | Absent | | **Schirmer test** | Normal or ↓ | Normal | Normal | Normal | | **Corneal involvement** | Shield ulcer, scarring | Giant papillae, shield ulcer | Rare | Absent | **High-Yield:** The combination of **chronic (6 months) bilateral presentation, perennial symptoms, normal Schirmer test, ropy discharge, and papillary (not follicular) response** in a middle-aged woman is diagnostic of AKC. ### Pathophysiology of AKC 1. **Type I and Type IV hypersensitivity** — both IgE-mediated and T-cell-mediated responses 2. **Mast cell and eosinophil infiltration** of conjunctiva and lid margin 3. **Chronic inflammation** → fibrosis, lid margin scarring, and trichiasis 4. **Corneal involvement** → shield ulcers, scarring, and potential vision loss **Clinical Pearl:** AKC is distinguished from VKC by age (AKC: older adults; VKC: children/young adults) and lid involvement (AKC: lichenification and dermatitis; VKC: absent). SAC is seasonal and milder; AKC is perennial and more severe. ### Clinical Features of AKC - **Lid signs:** Lichenification, dermatitis, madarosis (eyelash loss), trichiasis - **Conjunctival signs:** Papillary hypertrophy (mild, <1 mm), ropy discharge, chemosis - **Corneal signs:** Shield ulcers (superior cornea), scarring, neovascularization - **Systemic associations:** Atopic dermatitis, asthma, allergic rhinitis **Warning:** Do NOT confuse AKC with VKC — VKC is seasonal, affects children, and presents with giant papillae and severe photophobia. AKC is perennial, affects older adults, and is associated with atopic dermatitis. ### Management Algorithm ```mermaid flowchart TD A[Atopic Keratoconjunctivitis diagnosis]:::outcome --> B[Mild disease?]:::decision B -->|Yes| C[Topical antihistamines<br/>Mast cell stabilizers<br/>Cool compresses]:::action B -->|No| D[Topical corticosteroids<br/>Tacrolimus ointment<br/>Cyclosporine drops]:::action D --> E{Corneal involvement?}:::decision E -->|Shield ulcer| F[Aggressive topical steroids<br/>Lubricants<br/>Consider bandage CL]:::action E -->|Scarring/vision threat| G[Systemic immunosuppression<br/>Cyclosporine/azathioprine]:::action C --> H[Follow-up in 2-4 weeks]:::action F --> H G --> H ``` **High-Yield:** Topical **tacrolimus 0.03% ointment** and **cyclosporine 0.05% ophthalmic emulsion** are steroid-sparing agents increasingly used in AKC to avoid long-term topical steroid side effects (glaucoma, cataract). 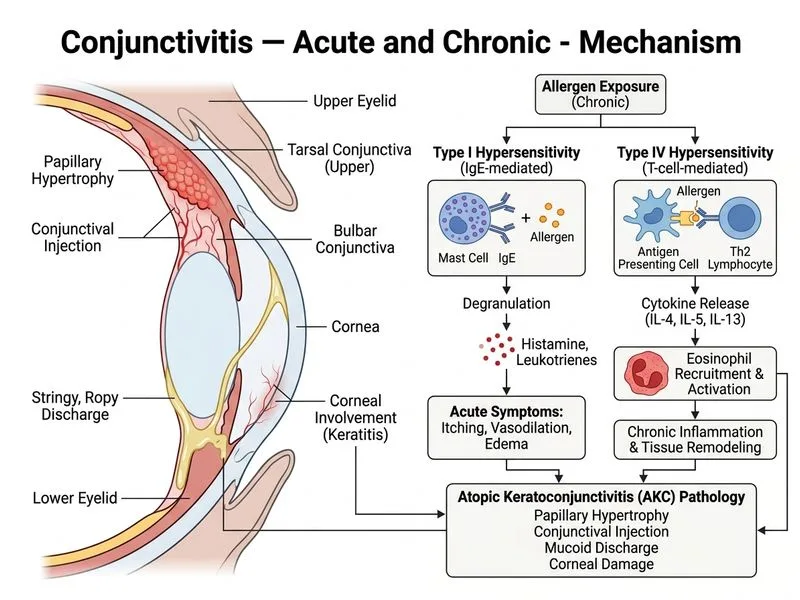
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.